Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and otherwise medically complex Patients by improving their Quality of life and where we also provide tailor made solutions to hospitals and Intensive Care Units to save money and resources, whilst providing Quality Care!
In the last blog I shared
DISCHARGING PATIENTS HOME FROM ICU POSES NO ADDED RISK!
You can check out last week’s episode by clicking on the link here.
In this week’s blog I want to answer a question that we get quite frequently from our clients and also from people all over the world that visit our website.
When can a tracheostomy be removed?
Many mechanically ventilated Patients in Intensive Care in an induced coma require a breathing tube/endotracheal tube to facilitate such mechanical ventilation during critical illness.
The goal should always be to wean mechanical ventilation, get a critically ill Patient out of the induced coma, get them extubated (removal of the breathing tube/endotracheal tube) so that they can breathe spontaneously and unaided so that they can leave Intensive Care and eventually go home.
If for whatever reason, weaning off mechanical ventilation and the breathing tube/endotracheal tube fails, a tracheostomy might be considered as a next step.
When is the right time and right situation to do a tracheostomy?
Here are articles and videos that will give you all the knowledge you need if your loved one should have a tracheostomy or not
Once a tracheostomy has been done, your loved one can hopefully take the first steps to wean off ventilation and tracheostomy!
Once the ventilator has been weaned, then the next step is to remove the tracheostomy!
How does ventilation get weaned when having a tracheostomy?
Here are articles and videos that will explain it for you!
In most cases, a tracheostomy is temporary, providing an alternative breathing route until other medical issues are resolved. If your loved one needs to remain connected to a ventilator indefinitely, the tracheostomy is often the best permanent solution.
In order to have the tracheostomy removed (decannulation) your loved one needs to be off the ventilator completely and can breathe via trachea mask, trachea hood, trachea collar or trachea shield then it’s time to assess if your loved one can have the tracheostomy removed!
Certain criteria need to be met for tracheostomy decannulation such as
- Good strong cough/gag needs to be present in order to protect the airway
- Swallow reflex needs to be present so that your loved one is not aspirating secretions, sputum, gastric content or food
- Able to obey commands (In the non- neurologically compromised patient)
- Adequate cough and ability to clear secretions effectively and independently.
- Cardiovascular and hemodynamic stability.
- No new lung infiltrates on chest x-ray.
- Tolerates cuff deflation for 24 hours.
- Tolerates speaking valve 12 hours or more (usually during daytime) or decannulation cap for up to four hours (If air flow is present on finger occlusion). In patients following head and neck surgery, the decannulation cap may be left for longer periods at the discretion of the surgeon
Whenever weaning off ventilation and removal of tracheostomy in Intensive Care fails or is prolonged, INTENSIVE CARE AT HOME of course is a viable and genuine option, creating a win-win situation for all parties involved by
- Getting Patients out of Intensive Care into a holistic Patient and family friendly environment by having 24/7 ICU nurses come to your home
- Improving Patients and families quality of life and in some instances quality of end of life
Related:
- reducing the cost of an Intensive Care bed which is $5,000 per bed day, by more than 50% therefore making health insurances and health funds wanting to support INTENSIVE CARE AT HOME services
- Freeing up an in-demand and expensive Intensive Care bed that the hospitals need for other critically ill Patients
- Helping families to stay economically viable. I.e. when they have a loved one in Intensive Care, families often spend day and night in Intensive Care leaving them unable to produce an income. By having 24/7 Intensive Home Care instead of Hospital Intensive Care, families don’t have to worry about financial issues because they can go back to work
We also have some case studies here so you can see how we have provided INTENSIVE CARE AT HOME services to Patients with tracheostomies.
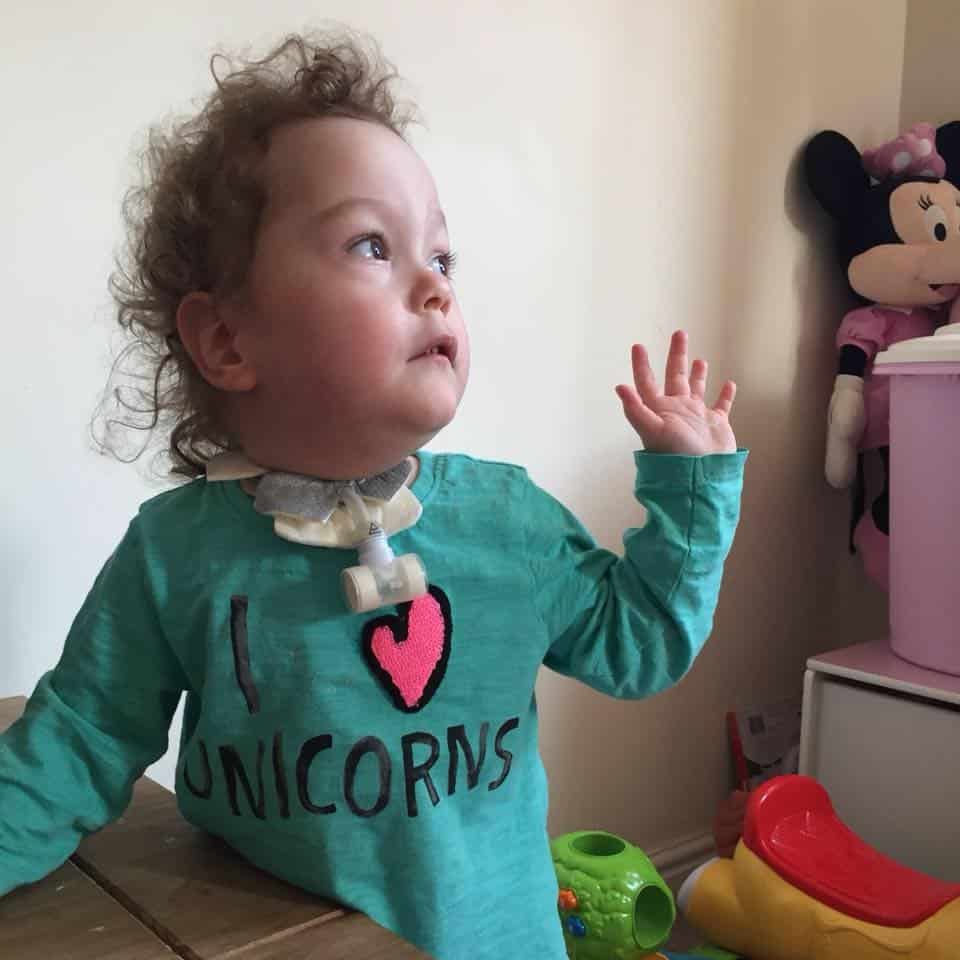
The first case study is where we looked after a 15 month old toddler with tracheostomy at home. The toddler eventually had the tracheostomy removed, therefore it ties right in with our topic. Here is a link to it
Another client we looked after at home, where we provided palliative care whilst the client was ventilated with tracheostomy is here
Last but not least, here is also some advice for our readers and clients in the USA.
Many families contact us from the USA and they have a loved one in long-term acute care(LTAC) with a ventilator and tracheostomy.
It always saddens me deeply when we get those enquiries, because LTAC’s are not the right place for Patients on ventilation with tracheostomies!
Many Patients in LTAC die because the facilities simply lack the skills, expertise and know-how when it comes to ventilation and tracheostomy.
Ventilation and tracheostomy require ICU trained doctors and ICU trained nurses, period!
Therefore, the only safe environment for ventilated adults and children with tracheostomies are either ICU or a home care environment with ICU nurses like you can get here at INTENSIVE CARE AT HOME.
But if you have a loved one in LTAC, please contact us here and we can help you take the next steps to get your loved one home ASAP!
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care(also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator, if you want to know how to get funding for our service or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
Also, check out our careers section here
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in Melbourne, Sunbury and in South Gippsland/Victoria.
We are an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
We have also been part of the Royal Melbourne health accelerator program for innovative health care companies last year!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update!








