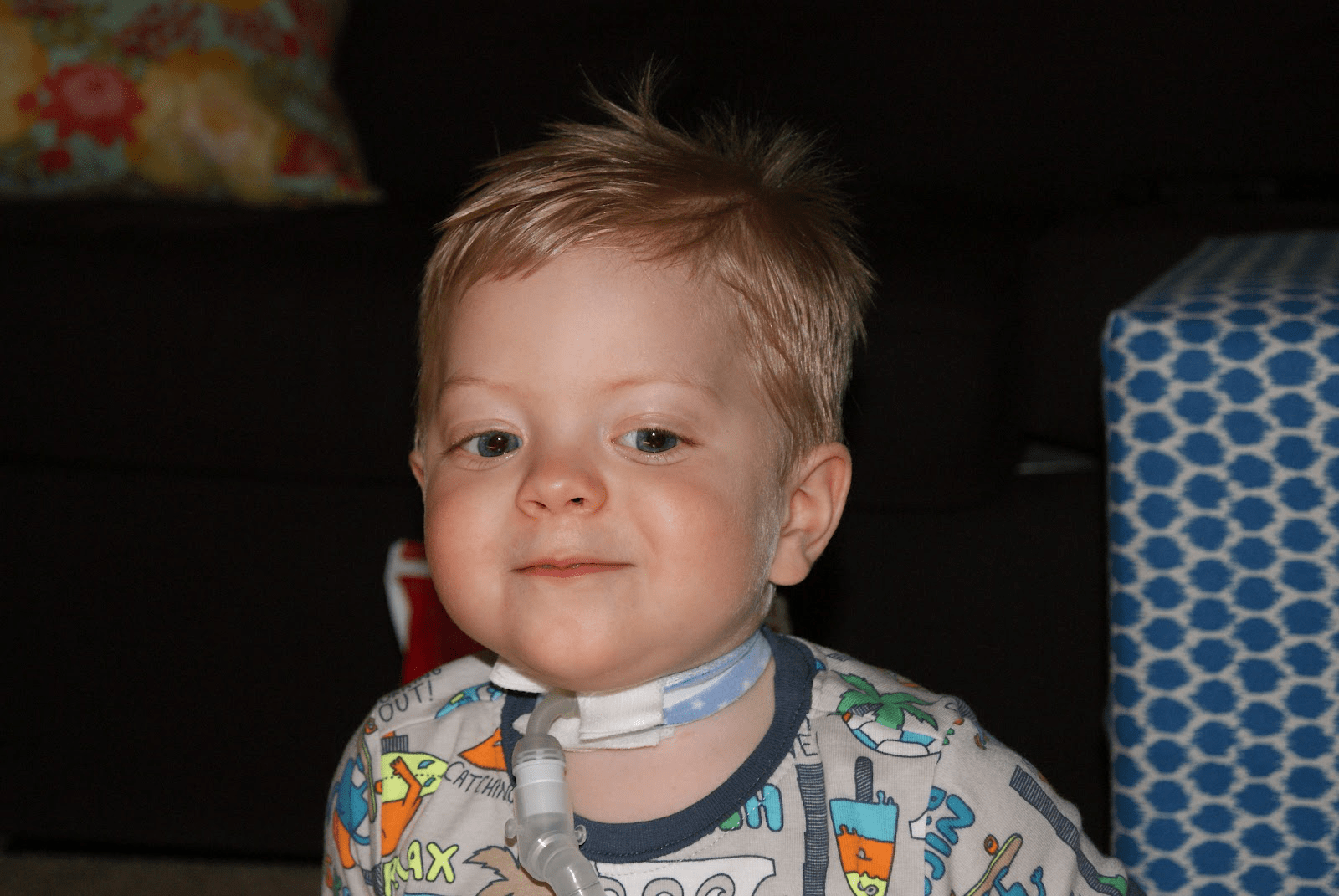
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies by improving their Quality of life and where we also provide tailor made solutions to hospitals and Intensive Care Units to save money and resources, whilst providing Quality Care!
In the last blog I talked about
THE 10 QUALITY FEATURES TO LOOK FOR WHEN IT COMES TO HOME VENTILATION AND TRACHEOSTOMY!
You can check out last week’s blog by clicking on the link here.
In today’s blog I want to present another INTENSIVE CARE AT HOME case study to add on to our long list of case studies.
One-way extubation at home for a newborn baby!
Today’s case study is somewhat unique as it’s a one-way extubation at home.
For those of you reading and you haven’t heard about one-way extubation in this context, it’s basically removal of life support by removing the breathing tube/endotracheal tube and the ventilator for end of life care.
This happens in ICU/PICU/NICU regularly and it’s often not the right environment for Patients and their families.
Thankfully with accredited services like INTENSIVE CARE AT HOME Patients, their families and ICU’s/PICU’s and NICU’s can extend their end of life care/palliative care services in to people’s homes which is more often than not their choice!
Related articles/videos
Case study:
Serena was born with Hypoxic Ischemic Encephalopathy (HIE) which is a type of brain damage that occurs when an infant’s brain doesn’t receive enough oxygen and blood.
Initially her APGAR was 9.
A few hours after Serena was born she had a cardiac arrest and she needed CPR, inotropes and intubation.
After cardiac arrest, Serena received therapeutic hypothermia for four days and after rewarming, Serena had ongoing seizures requiring medication management such as Midazolam, Phenobarbitone, Phenytoin (Dilantin), Levetiracetam (Keppra) as well as Pyridoxine.
Day five Serena was seizure free on those medications.
On a respiratory level Serena required intubation after CPR, she then had a brief period on CPAP only to be reintubated after status epilepticus needing further midazolam infusions.
Serena had issues with oral secretions and protecting her airway. She developed a right lower lobe collapse which required deep suctioning.
Serena therefore was commenced on IV antibiotics.
She also had feeding difficulties and couldn’t absorb NG feeds.
Serena’s MRI was consistent with severe central HIE changes.
Given Serena’s ongoing neurology the decision to redirect care in the comfort of her parents home was made and Serena was transferred home on day 24 after birth.
At home Serena was electively extubated and comfort care with the palliative care team and with the intensive care at home team was made possible for baby Serena and her loving parents.
The following medication was provided for baby Serena’s comfort and symptom management.
Clonazepam, Glycopyrrolate, Keppra (Levetiracetam), Midazolam, Morphine, Phenytoin (Dilantin), Paracetamol.
A nasogastric tube was left in situ and a subcutaneous butterfly for administering medications post-extubation to avoid distress and provide comfort.
Family and friends attended this ceremony at home with a photographer present to capture the last hours of baby Serena.
This provides a nice contrast compared to providing end of life care in ICU/PICU or NICU. It also provides holistic end of life care, where the family and their needs are considered.
We felt very privileged to be able to provide this service to Serena and her family as well as to the referring NICU.
End of life care for ICU/PICU and NICU Patients should and will become more mainstream because that’s what Patients and families want.
It creates a win-win situation.
It gives Patients and families what they want, it frees up in-demand, expensive and highly sought after ICU/PICU and NICU beds and it cuts the cost of a $5,000- $6,000 per bed day ICU/PICU/NICU bed by 50%.
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care (also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator, if you want to know how to get funding for our service or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
Also, check out our careers section here
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in the Melbourne metropolitan area, northern suburbs, Mornington Peninsula and in South Gippsland/Victoria.
We are an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
Also, have a look at our range of full service provisions here
https://intensivecareathome.com/services
We have also been part of the Royal Melbourne health accelerator program for innovative health care companies last year!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update!