Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to share an article published on December 5, 2021 from “The Guardian” and this is about,
Terminally ill NDIS (National Disability Insurance Scheme) Participant Facing Re-Hospitalisation After Funding Cut for 24-hour nurse
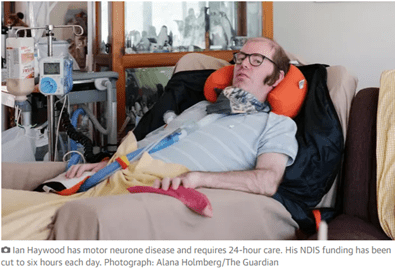
Ian Haywood’s partner is blunt when asked to sum up the couple’s latest battle with the National Disability Insurance Agency.
“They don’t think it is ‘reasonable and necessary’ for Ian to have nursing funding,” Bianca* told Guardian Australia, referring to the key legal test for NDIS funding.
“We think it is reasonable for him to stay home and it is necessary in order for him to live. It’s cheaper for them if he dies.”
Haywood, 43, lives with the terminal illness motor neurone disease and is the latest NDIS participant to speak out about what the federal Labor party and disability advocates claim are “stealth cuts” being seen around the country.
Communicating with Guardian Australia via email as he is non-verbal, Haywood said the NDIS had been funding 24-hour nurse care that allowed him to live at his home on the Mornington Peninsula rather than remaining in hospital.
But when his plan was renewed for 12 months in October, he learned it would only cover six hours of care each day from a nurse.
Haywood said he needed 24-hour care from a trained nurse because he cannot breathe for himself: he is mechanically ventilated via tracheostomy and needs urgent help if something goes wrong.
“Usually it’s something simple like a leaking valve, a nurse with ICU experience can identify the problem and resolve it,” Haywood said. “But without a nurse I would be long dead of asphyxia before the ambulance arrived.”
The funding was initially provided by the agency after he won an internal review of an earlier decision last year, Haywood said.
Now, the NDIA has said it will no longer fund the same level of support.
“My particular concern is that I have a ‘deadline’ of around mid-January when the nursing funding runs out, at which point in the worst case I would have to go to ICU and wait for it to be resolved,” Haywood said.
During question time in parliament last week, the government was asked about several cases where participants and their families have been forced to appeal large cuts to NDIS plans.
Disability advocacy organisations have also told Guardian Australia they are being swamped with requests from participants for help to appeal against the NDIA’s decisions.
“It just seems so pointless to have to re-litigate the same issue [24-hour nursing care] when the need has previously been established,” Haywood said.
Bianca said she had experienced nightmares during that last process. “I’d be like dreaming that he died,” she said.
Haywood was diagnosed with motor neurone disease five years ago this week.
Until then he’d worked as a child and adolescent psychiatrist.
“Now I can’t move very much at all,” Haywood said. “I can wiggle my wrists, I can turn my head slightly, and I can blink and move my eyes. Some additional movements are still present but not under my voluntary control: for example I will smile if told a joke.”
Still, Haywood said there was plenty he could do. He uses a button under his left wrist that allows him operate a computer to use the internet, watch films and read books.
Last week, Haywood took part in a kitchen table Zoom meeting with the Voices of Mornington Peninsula political group.
He prepared his contribution and shared it with the group when it was his turn.
“People might look from the outside and just write him off, but he actually feels like he has a reasonable quality of life at the moment,” Bianca said. “A large part of that is the nursing staff look after him really well.”
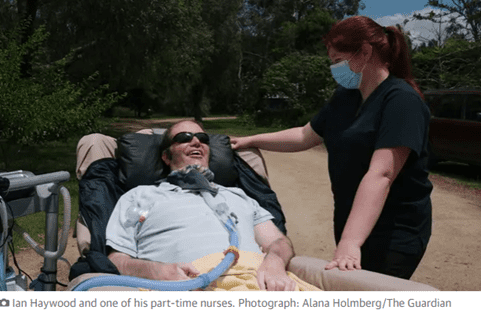
After he was hospitalised in 2019 with pneumonia, Haywood made the tough decision to be intubated and ventilated.
He said he did it so he could spend more time at home with his family. They had briefly trialled aged care nurses caring for Haywood, but that was a “disaster” due to the technical expertise required in his case.
In many cases, the workers themselves did not want to continue at the home due to the complicated nature of the role and the high risks involved.
Since then, they have found a provider with ICU-trained nurses and Bianca says the care has been excellent.
“This is what [the nurse are] skilled at, this is their job,” Bianca said. “This is what we’ve been trying to explain to the NDIA, ‘There can be a problem any day or night, you never know when there is going to be a problem.’”
A NDIA spokesperson said the NDIS “continues to provide a significant level of funding for Mr Haywood’s disability-related supports, including 24/7 support”.
“In some cases, such as this, where a participant requires nursing supports that can be delivered by a disability support worker, a transition will occur for a nurse to work closely with the disability support worker to implement a care plan, and provide appropriate training to support the participant safely,” the spokesperson said.
Haywood and Bianca insist the current arrangement is the only one that is safe. They had not heard anything about a so-called “transition” until the NDIA’s statement to Guardian Australia.
If the funding is not reinstated, Haywood will probably be forced to back to hospital. The other option is a group home for people who are ventilated in Thornbury, more than an hour’s drive from where the family currently lives.
“So maybe Ian would end up there, rather than in his own family home,” Bianca said. “It’s just ridiculous.”
With Haywood at home, he can still spend plenty of time with his eight-year-old son. “Ian has introduced him to Doctor Who,” Bianca said. “They’ll play chess together, they’ll do other stuff together.
“They’ve got their other YouTube videos they watch together. We’ll play other board games … and stuff like that together.”
Bianca said the family was “just exasperated” to be going through their second appeal process in two years.
“Will we have to do this next year?” she said.
*Name changed for privacy reasons
REFERENCE:
- Terminally ill NDIS participant facing re-hospitalisation after funding cut for 24-hour nurse
- Images credit to:
Now, if you have a loved one in intensive care and you want to go home with our service Intensive Care At Home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive Care At Home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Mornington Peninsula, Frankston area, South Gippsland, as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
https://www.melbournehealthaccelerator.com/
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care At Home, and I’ll see you again next week in another update.









