Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
This is a case study of an ex-premature baby, now a toddler, who went home with tracheostomy after weaning from CPAP in hospital after prolonged hospital and initial NICU and then PICU stay through Intensive Care at Home.
Successful Transition & Better Standards of Care from Pediatric ICU to Intensive Care at Home for my Toddler with a Tracheostomy.
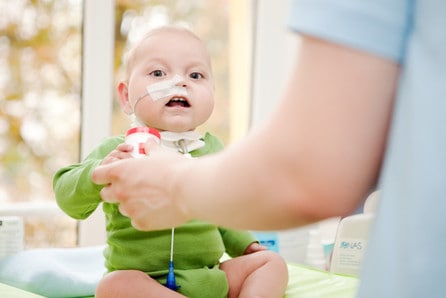
MEDICAL BACKGROUND:
This intensive care at home client was an ex-prem baby (24+5/40). CLD. Difficulties with weaning from CPAP led to further investigations, revealing tracheomalacia/tracheobronchomegaly requiring a tracheostomy.
No oxygen required.
Speaking valve: tolerated during day when awake under direct supervision for short periods.
Overnight CPAP ceased following sleep study. PDA resolved and small ASD. Difficulties with feeding and vomiting. Nasogastric tube feeding.
Findings from the Allied health team assessment indicated that the patient presents with global developmental delay characterized by delays in gross and fine motor skills, communication, and cognition compared to children of a similar age. This can be explained by both the prematurity and prolonged hospital stay due to other complex medical and surgical issues.
Hx began having seizures day 3-5 of life (bilateral jerking movements) requiring multiple AEDs to control.
EEG: focal seizures (right), background mildly dysmature for age. Seizures generalised. Phenobarbitone ceased. MRI Brain: structurally normal, normal white matter volume.
Baseline assessment – RR 32-50 bpm, Sp02 95-100% in RA normal suctioning requirements: daytime —30 minutely, overnight minimal. Bradycardia at times during sleep down to 70-75 bpm. Patient was discharged from Cardiology. An ECG and ECHO were performed at this time. Doctor approved for Iow HR alarm on oximeter to be changed from 85 bpm to 65 bpm.
Feed tolerance is an ongoing issue for patient. It is not unusual to have multiple small vomits per day, especially following a cough. On NGT feeds: 7 bolus feeds per day administered via pump over (Fortified Neocate Gold). Exploring oral purees and sipping thin fluids. No issues on full enteral feeds. Previous borderline hypoglycaemia (never below 3mmoI/L) after. Allergies: Cow’s milk protein and soy. On esomeprazole. Lower GI contrast study. NAD.
Client went home with tracheostomy after weaning from CPAP in hospital after prolonged hospital and initial NICU and then PICU stay.
The client was 12 months old when going home.
Our intensive care at home nursing team was managing the child overnight for 6 months until the child was ready for tracheostomy decannulation.
Our nursing team where we employ hundreds of years of intensive care and paediatric intensive care nursing experience combined was able to transition the child home from paediatric intensive care to an intensive care at home environment without any lowering of care standards.
Our clients get the same or better standards of care at home compared to an intensive care (ICU) environment, because clients can be in control of their routine and their wishes.
They can sleep at night in the comfort of their own home, whereas in intensive care it’s very noisy.
Also, our client’s family members also report to get some sleep at home because they know they have intensive care nurses that are comfortable with ventilation and tracheostomy.
Our intensive care at home nursing team enabled the toddler to transition to a holistic, loving and supported intensive care at home nursing environment instead of spending more unnecessary time in intensive care or even worse being discharged home with no support or with untrained support, I.e. support workers or general registered nurses. Neither support workers nor general registered nurses have the expertise, skill, training or know-how to look after tracheostomy.
Only intensive care trained nursing staff with a minimum of two years ICU/PICU experience are competent to provide intensive care at home nursing services and therefore are competent to look after ventilated and/or tracheostomy adults and children at home.
This is evidence based as per the mechanical home ventilation guidelines. The home mechanical ventilation guidelines are also demanding that services are third party accredited.
https://intensivecareathome.com/mechanical-home-ventilation-guidelines/
Currently, INTENSIVE CARE AT HOME is the only nursing service in the world that has achieved third party accreditation for INTENSIVE CARE AT HOME nursing services.
This enables long term ventilated and/or tracheostomy adults and children to leave intensive care much earlier than previously perceived I thought possible.
It also enables intensive care units to move away from saying that patients won’t have any quality of life if they survive their stay in intensive care.
They do have quality of life at home with a professional service like intensive care at home.
Intensive care units benefit from our service also, because we reduce the cost of an intensive care bed by approximately 50%.
Furthermore, INTENSIVE CARE AT HOME is freeing up in-demand ICU.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Mornington Peninsula, Frankston area, South Gippsland, as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
https://www.melbournehealthaccelerator.com/
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from intensive care at home, and I’ll see you again next week in another update.







