Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
IS A TRACHEOSTOMY GOING TO WORK?
You can check out last week’s blog by clicking on the link below this video:
https://intensivecareathome.com/is-a-tracheostomy-going-to-work/
In today’s blog post, I want to answer a question from one of our clients.
Will a Tracheostomy Work in the Community?
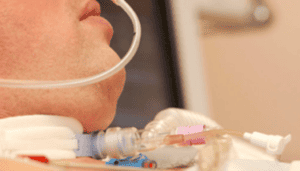
Hello and welcome to another Intensive Care at Home and Intensive Care Hotline YouTube livestream.
Today’s topic is, “Will a tracheostomy work in the community?” And that’s a question we get quite frequently. It’s actually a question that ties right in from my last podcast or my last YouTube live stream last week. The topic last week was, “Is the tracheostomy going to work?” And out of the questions that came in from that live stream, I thought, “Well, that is a question that needs to be answered as well, “Will the tracheostomy work in the community?””
So, last week’s YouTube live was all about what’s a tracheostomy? How is this going to work? When should it be used? What are the outcomes? and so forth. So, today we look much deeper, and look will the tracheostomy work in the community? Let’s just say someone needs a tracheostomy for much longer periods of time than expected. Let’s just say someone needs a tracheostomy for the rest of their life, God forbid. Then you need to inevitably think about whether you can go in the community, and we will break that down today, when a tracheostomy is advisable in the community? What resources you will need to make that safe in the community and avoid hospital readmissions, avoid ICU readmissions and make home care and home stay predictable so that an admission back to ICU or a hospital is not necessary full stop. But we’ll talk about that today.
So, in more detail on today’s topic, in case you are wondering what makes me qualified today to talk about today’s topic, my name again is Patrik Hutzel. I’m a critical care nurse by background. I have worked in intensive care/critical care for over 20 years in three different countries. I have worked as a nurse unit manager for over five years in intensive care. I’ve been the founder and managing director of Intensive Care at Home, where we provide Intensive Care at Home as a genuine alternative to a long-term stay in intensive care where we take patients home from intensive care directly. We avoid emergency department or emergency room admissions, so we deliver on what we are promising, which is Intensive Care at Home.
I’m also the founder and director of the Intensive Care Hotline at intensivecarehotline.com. We are providing consulting and advocacy service for families in intensive care all around the world. We have been consulting and advocating for families all around the world for the last 10 years, just as much as we have been providing Intensive Care at Home for the last 10 years.
We are predominantly working, or we are operational with Intensive Care at Home all around Australia. We are an NDIS (National Disability Insurance Scheme), TAC (Transport Accident Commission), iCare, NIISQ (National Injury Insurance Scheme in Queensland), and DVA (Department of Veteran Affairs) approved community service provider. We have also received funding through departments of health and through hospitals directly. So, whether you are a patient in intensive care, whether you’re a family having a loved one in intensive care and you’re considering Intensive Care at Home, please contact us one way or another.
You may also want to contact us if you’re an NDIS support coordinator and you’re looking for nursing care for your participant, for your client. If you don’t know how to go about the advocacy for funding for your NDIS participant, please contact us. We can help you with all of that. If you’re an intensive care consultant, please contact us as well. If you’re a hospital executive and you’re looking how to more efficiently manage your ICU beds and partner with your consumers, which is part of the accreditation standards for hospitals, you know where we are. Please contact us on one of the numbers on the top of our website at intensivecarehome.com or send us an email to [email protected].
If you are a critical care nurse and you know of patients in ICU and I’m sure you do, please contact us as well. We also offer jobs for our critical care nurses here in Australia and also for intensive care specialists. We are expanding our nursing and our medical team as well. If you’re in the United States or in the U.K., please contact us as well. We can help you one way or another, whether you have a loved one in intensive care with consulting and advocacy, with Intensive Care Hotline or with even home care. We can point you to the right directions. We have helped families in the U.S. and in the U.K. to get on the path of Intensive Care at Home with other providers. So, one way or another we can help you.
I also want to welcome our viewers that are watching this on replay. Again, type your comments in the chat pad. I will answer your questions whether it’s in a short quick tip video or on these broadcasts. I will get to those questions one way or another, but the quickest way is obviously to talk to us directly. Just reach out to us over the phone or via email as well.
A bit of housekeeping, type your questions into the chat pad, but if we have time, you can also dial into the show if you want to, but only after we’ve been through today’s presentation, then there’s time for other questions to answer.
So, let’s dive right into today’s topic, “Will tracheostomy work in the community?” Again, is almost a sequel from last week where I had a YouTube live where the question was, “Will a tracheostomy work?” Again, these are questions we’re getting from families in intensive care. They’re not questions that I’m making up. These are questions that our audience find extremely valuable, and which is why I am answering them in the weekly shows.
So, “Will tracheostomy work in the community?” Well, I don’t want to recap my video from last week, but one thing I need to make, once again, very, very clear here. If you are having a loved one in intensive care on a breathing tube in an induced coma, the goal should be to have the breathing tube removed and avoid the tracheostomy. That should be the goal. There’s no left right from here. The goal should always be to have a breathing tube removed, avoid the tracheostomy. Irregardless of Intensive Care at Home, that is the goal full stop. Now, let’s say your loved one does need a tracheostomy while in ICU, then the next goal should still be, wean off the ventilator, get the tracheostomy removed. That should be the goal.
Now, let’s just say, God forbid that’s all failing, all going to fail, your loved one or you need a tracheostomy potentially for the rest of your life. Then of course you need to consider options in the community and that’s when Intensive Care at Home comes in. So, for example, at the moment we are working with a client for Intensive Care Hotline who has their husband in ICU on a breathing tube, and she’s already thinking, “Oh, should he have a tracheostomy and then come home?” No, the goal is to have the breathing tube removed, avoid a tracheostomy, and then go home. So, don’t use a tracheostomy as a vehicle to go home. Going home might be a vehicle if you need a tracheostomy and it’s not avoidable. I hope I cleared that up once and for all.
Then, will a tracheostomy work in the community? Well, it works if the support is safe. So, what do I mean by that? So, healthcare is all about evidence-based. Healthcare is all about evidence-based. Healthcare is about accreditation and certification. So, what do I mean by that? With Intensive Care at Home, we are a specialist service. We are an accredited specialist service. We are the only service in Australia in 2023 that has accreditation for Intensive Care at Home services at home. We have policies, procedures, quality manuals, more importantly, we have the staff, the critical care nursing staff that make this happen. We employ hundreds of years of intensive care and emergency department nursing experience. So, what that means is we have the skills and expertise to manage tracheostomies at home.
Now, when you think about it, let’s just say someone is at home with a tracheostomy and they go back to hospital or worse, they go back to ICU. The only people that can look after tracheostomy and ventilation patients in the hospital are intensive care or critical care registered nurses. No other nurses have the skills. So, why should that be different at home? So, makes perfect sense that you want to have the same setup at home, which again is Intensive Care at Home.
So, before we started being in business about 10 years ago, there were no regulations in home care. Anyone and their dog could look after tracheostomy at home, often with catastrophic consequences, i.e., patients have died because they weren’t looked after at home with critical care registered nurses. So, you’ve got to have the right setup.
So, coming back to evidence-base, in a hospital you wouldn’t send someone with a tracheostomy to a ward where they don’t have critical care registered nurses. So why would that be different at home? So, comes back to once again to accreditation and certification, which we have. It comes back also to the Mechanical Home Ventilation Guidelines. When you look at the Mechanical Home Ventilation Guidelines on our website at intensivecareathome.com, you will see that these evidence-based guidelines will only permit patients to go home from intensive care or hospitals with a tracheostomy or with a ventilator even on ventilation without a tracheostomy such as non-invasive ventilation such as BIPAP or CPAP. It’s only safely possible with critical care registered nurses with a minimum of two years critical care nursing experience in the hospital.
So, the quality standards that we’re setting in the community are very high and so it should be because if those standards are not met, if the accreditation that we are having is not met, patients will inevitably die.
So, just quickly coming back to the Mechanical Home Ventilation Guidelines, when you look at them on our website, you will actually see that they are coming out of Germany. Now, why are they coming out of Germany? Well, Germany was the first country worldwide who embraced Intensive Care at Home as a viable, holistic, and obviously patient and family friendly model of care that provides a win-win situation. I have firsthand experience with that. You can hear me speak with an accent. I was born in Germany, I did my nurse training in Germany and when I first started working in ICU in Germany a long time ago, then I became part of a pioneering service in Germany where we were the first ones to provide Intensive Care at Home. So, I’ve been working in the Intensive Care at Home field, including intensive care for the last 25 years.
In Germany in particular, this is a massive industry, but once again, it’s a very holistic and patient and family friendly industry. But that provides a win-win situation because it’s also not only about what patients and families want, it’s also what hospitals want, which is an empty ICU bed, which is cutting the cost for the most expensive bed in the hospital, which is the intensive care bed. It’s the most sought-after bed in a hospital, is the intensive care bed. Costs around five to $6,000 per bed day to have someone in intensive care and at home it’s about half of the cost. Plus, you have the added-on benefit that you can use the intensive care bed for other more critically unwell patients. So, it’s win-win all around for everyone.
It also takes the pressure off ward or floor beds in a hospital because what sometimes happens is that patients in intensive care go to a hospital floor to take the pressure off the intensive care bed with a ventilator or a tracheostomy, but it doesn’t eliminate the problem because then on a hospital floor or a hospital ward, they’re looked after still one and one with an intensive care nurse. They’re just shifting the problem to another area without really improving the quality of life for patients and for families. So, what needs to happen is simply that patients can go home straight away and eliminate those bed blocks. But more importantly, improve the quality of life or in some situations, quality of end of life for patients and their families.
Now also, you will see that some providers say they can provide tracheostomy and ventilator care at home. Again, we have evidence that patients have passed away if they’re not looked after by accredited and specialized health services like we are, I’ll give you a few examples actually. So, I know of at least five clients in the community that died with a tracheostomy, sometimes with a ventilator and the tracheostomy because they weren’t looked after by critical care nurses. They weren’t looked after by accredited health services like we are at Intensive Care at Home. So once again, there are no quality standards in the community, which is really very sad. If there are quality standards in a hospital, why are there no quality standards in the community?
Now, there are with Intensive Care at Home, we’re pretty much bringing the intensive care into the home, making sure you and your family are safe whilst having community access, very important. Very important that with Intensive Care at Home, it’s not as simple as we’re just replicating intensive care bed in the home, it’s also having community access.
So, before I come to community access, I just quickly want to talk about the pitfalls when a tracheostomy is not working in the community, which is when critical care nurses are not there, 24 hours a day, again, as per the Mechanical Home Ventilation Guidelines on our website at intensivecareathome.com. So, case in point, we had three clients in 2020 that were not funded for 24-hour critical care nurses at home. Three out of those three clients had a tracheostomy, one was ventilated, two, “only” had a tracheostomy, but bear in mind the tracheostomy is still an artificial and also unstable airway. If that airway goes, patients die. It’s as simple as that, which is exactly what’s happened with two of those three clients we were only funded for overnight shifts and no critical care nurse during the day.
We highlighted that to the funding body at the time, which was the NDIS, and we said to them, “Well, the minute we are leaving this patient’s life is in danger, it’s hanging at a threat.” And we were laughed at. We said, “Oh yeah, you just want to promote your business.” Yeah, we do, but for only good and ethical reasons, because all of those three clients passed away during the daytime just as we predicted. Let that sink in.
So, coming back to our original question, will a tracheostomy work in the community? The answer is yes, with 24-hour critical care registered nurses, that’s when a tracheostomy in the community works. Anything less than that could be a death sentence. Another patient or another client, I should say, passed away in hospital. We had funding for two short visits a day, one hour in the morning, one hour at night for a tracheostomy patient who otherwise would be in intensive care. Always think about that, let that sink in. The patient was at home with a tracheostomy. We had a visit funded one hour in the morning, one hour at night, and if they weren’t at home, they would be in intensive care otherwise.
Cutting a long story short, this particular patient passed away in hospital after she was put on the ward on a hospital floor. She had a tracheostomy blockage and she passed away of her respiratory arrest that eventually led to a cardiac arrest because she wasn’t looked after in a hospital as per Mechanical Home Ventilation Guidelines. They didn’t have an ICU bed at the time.
There’s two other participants or clients that I know of that have passed away in the community that died because of support workers or family members not being able to manage a medical emergency for what’s an intensive care patient. So, I’m not making this up. I have actually evidence to back up what I’m saying here.
So also, when it comes to tracheostomy care at home or ventilator care, you want to be looked after by a specialist, not by a generalist. When you look at some provider’s website, you will see that some providers, they do aged care, they do disability and then on that list you might see tracheostomy care. If someone is doing that, your alarm bells need to go off because the reality is that you need to be a specialist. You wouldn’t be having a tracheostomy patient in a hospital on the day surgery ward or on the dental ward or whatever the case may be. You would have them in intensive care and the same is applicable at home.
You will need them in a safe home care environment where intensive care can be replicated, but where all the resources, all the skills are available to manage whatever comes along or whatever goes hand in hand with the tracheostomy at home or in many instances also a ventilator. But today, I want to just focus on tracheostomy. Many tracheostomy patients in the community are also ventilated, but it’s a mixture of course.
Also, what else do you need? You also need to make it safe at home. You also need a very good, if you’re in Australia, you need a good NDIS support coordinator who can advocate for nursing care, for specialist nursing care at home for patients. So, it’s very much needed. Without a good NDIS support coordinator, nothing’s going to work. We have found there are some excellent NDIS support coordinators out there that we work with that can help with the 24-hour funding for nursing care.
So, if you are an NDIS support coordinator watching this and you want to know more about it, please contact us. We can help you with the advocacy. If you’re a hospital executive and you’re listening to this and you want to know, “Hey, how can we go about an NDIS support coordinator and funding so we can help our patients go home, improve their quality of life?” Partner with consumers, because that’s obviously an accreditation standard for hospitals, then I would like you to contact us as well. We can help with an NDIS support coordinator.
Other things you need at home on the question will the tracheostomy work in the community? Things like, you need a physiotherapy, physical therapist, OT (Occupational Therapist), you need a dietitian, you need a speech therapist. So, it’s not only the intensive care nurse. Again, if you look at the network or support that’s there in a hospital, you pretty much need the same in the community to make it safe. So, very important that you have all the resources, but once again, we can help you with all of that. So, we have the network to set you up with the right people in a home care environment of course.
Then also, what often happens, not all the time, but often it happens that when someone needs a therapist, they also need a PEG tube. When they need a tracheostomy in the long run, they often also need a PEG tube. There are some tracheostomy patients out there that can eat and drink, but they’re far and few in between. If they can’t eat and drink, patients need often a PEG (Percutaneous Endoscopic Gastrostomy) tube. Sometimes the nasogastric tube can be placed temporarily, and you would’ve seen me make videos about don’t give consent to a PEG tube. The exception to the rule there is that if you need a tracheostomy or a ventilator and a tracheostomy for the rest of someone’s life, then a PEG is advisable. But I’m very clear on when a PEG is advisable and when not.
But even if you choose to continue with the nasogastric tube, for example, we are now doing nasogastric tube changes at home. There are home x-ray companies who can follow up with the chest x-ray at home. So, there are more and more organizations doing what we are doing with the same goal, simply taking patients home and keeping them out of hospitals, keeping intensive care units empty in particular. So, there are more and more organizations who work on the same goals that we do.
We’re also currently providing an E.D. or emergency department bypass service for the Sydney area Western Health District. So, we are not only providing intensive care in the home, we’re now also providing an emergency room service at home, bypass service. So, there’s a lot of things we’re doing with Intensive Care at Home where we help the healthcare system to manage their resources better, but also improve the quality of life and quality of end of life for patients and families at home.
I also want talk about community access again, I did briefly mentioned that earlier. So, when you look at a long-term patient in intensive care, community access is not something you would associate with a patient in intensive care. Well, this is the major difference. While we are going home into someone’s home with Intensive Care at Home, there’s not one of our clients that doesn’t have community access. All of our clients have community access. So, not only are we bringing the intensive care to a home, but clients also have community access. They’re going out, they’re visiting their friends, they’re visiting their family, they’re going to school, they’re going to university. Whatever makes people’s world go round, this is definitely not happening in intensive care where people are confined to their rooms, to their beds. They’re confined to the routine of a hospital, whereas our clients can determine their own routine.
They determine what’s happening on a day-by-day basis. We are there to facilitate that. So, community access is a very important point, and most people think that’s not possible because they’re so shortsighted by this long-term stay in intensive care. They can’t really think of what’s possible outside of intensive care. So, I think that is really important to understand.
Now, also, coming back to the safety aspect when it comes to intensive care and Intensive Care at Home. So, I’ve been in a series of meetings with a public hospital, and I’m not mentioning names here, but I’ve been in a series of meetings with a public hospital here in Australia in regard to discharging a young man from intensive care who’s been in intensive care for 12 months initially. Then he went home for about three months, not with our service, but it didn’t work because the provider did not have any quality standards. The provider wanted to do it cheaply. He can’t do Intensive Care at Home cheaply. You can do it cheaper compared to an ICU bed, but I’m trying to avoid the word cheap. I’m trying to use the word cost-effective, cost-effectiveness, by sending enrolled nurses into someone’s home with a ventilator, with technically an intensive care patient.
Here is what’s happened. The provider couldn’t keep the client home, ended up back in ICU because the provider couldn’t provide community access because they didn’t have the skills, the knowledge, and the confidence to make community access possible for someone that’s technically an intensive care patient. They perceived that they couldn’t take the risk to make community access possible for this particular client because they didn’t work with intensive care nurses. Of course, that got this patient back into intensive care in no time. So, by trying to save even more money, it backfired.
Now here’s a question for you. So, if someone thinks that a patient an intensive care patient at home can be looked after by enrolled nurses or by support workers or by families, why are they in intensive care when they bounce back and why are they not on a hospital floor or hospital ward looked after by support workers and enrolled nurses? I’ll let you answer that question. I’m sure you can come to your own conclusions.
The interesting part was that when I have been on these meetings that there were about 20 people in the meeting from hospital executive, intensive care nurse managers, intensive care specialists, NDIS, and so forth. So, that’s how big the problem is when someone is in intensive care, long term. It rallies way more than a handful of people in meetings because the problem is so big.
What do we do with someone, their brain is working, they want to go home. How do we make this happen? Well, here is how we make it happen with Intensive Care at Home. We set it all up for you with equipment, with the nursing team, and we also help you with setting up the funding.
Also, for any of you watching that are an NDIS support coordinator for example, or a case manager for other funding bodies, I really encourage you to contact us as well. We can walk you through the advocacy process. We’ve also found that many NDIS support coordinators or even advocates or case managers, they don’t even know when Intensive Care at Home can be used. They don’t even know why a critical care nurse is needed in the community. In a nutshell, well, it’s needed in the community because they’re needed in intensive care and hospital, so they’re needed in the community to continue the same level of care and make it safe and more importantly, keep clients at home predictably. I think that’s really what we’re in the business in, that we’re in is keeping our intensive care clients at home predictably without any hospital admissions. It’s one of our KPI’s, key performance indicators, that we have no non-elective readmissions back to ICU. We are achieving that pretty much 99.9% of the time.
Again, if you have a family member in intensive care in a situation like that, I encourage you to contact us to take the next steps with us so we can help you get your family member home. You might be watching this, and you might be stuck in intensive care yourself. If you don’t know what to do next, contact us at intensivecareathome.com and contact us on one of the numbers on the top of our website or simply send us an email to [email protected].
If you’re a hospital executive, if you’re an intensive care specialist in ICU, medical director, ICU nurse manager, who knows you’ve got a problem with bed blocks in ICU exit blocks, you know where we are. If you’re worried about funding, don’t worry about it. We can help you with NDIS support coordinators. So, that’s when a tracheostomy will work in the community.
Other things that need to happen when there’s a tracheostomy in the community of course is the setup in terms of there need to be spare tracheostomies at home. There needs to be an Ambu bag at home. There needs to be a tracheal dilator at home. There needs to be nebulizers at home, spare inner cannula, assuming this particular when a patient goes home with an inner cannula. Humidifiers for the tracheostomy collar or tracheostomy mask, oxygen in case of an emergency. But more importantly, a critical care register said nurse with a minimum of two years critical care nursing experience. A doctor should be overseeing the care of course.
Again, if you’re an intensive care specialist here or a respiratory physician and you have patients that would benefit from our service, please contact us. I also encourage you that if you want to work with us, we are currently expanding our ICU Intensive Care at Home medical team as well.
So, if there are any questions in regard to today’s topic, “Will a tracheostomy work in the community?” Any questions, comments, please type them in the chat pad. If there are no other questions, then I would like to move on and go to some questions that came in during the week. I will just have a look at my email and then I will go through my questions. In the meantime, feel free to type your questions into the chat pad.
On today’s topic, “Will a tracheostomy work in the community?” I also want to give an example from a client that we worked with for many years, and this is maybe not the client that you… It actually has nothing to do with a tracheostomy, but it has everything to do with the client that has high respiratory needs.
There’s a client that we worked with actually in the U.K. Initially, we were working with a family as part of our consulting and advocacy service at intensivecarehotline.com and there the client went home on BIPAP. Even on BIPAP, if you look on our website at the Mechanical Home Ventilation Guidelines, you will see that on BIPAP or CPAP, a client needs a one-to-one intensive care nurse or critical care nurse at home. This client never had this and has been bouncing back between hospital and home for the last year and a half, and now she’s back in hospital. She’s been in contact with us. She’s now back in hospital on high flow during the day, BIPAP overnight. She’s very, very unwell and I argue that would’ve never happened if she had Intensive Care at Home to begin with.
It’s critically important that when it comes to the transition of patients going home, that you know what you’re doing and you know what setup you need, and that’s what we are specialized on. That is what we are specialized on. We’re specialized on home care for what are technically intensive care patients, but we don’t want to medicalize them at home because it’s really important that they can live a better quality of life and that they can have community access.
Let’s look at a question that’s come in during the week from Annette. Annette writes, “Hi, Patrik. I wonder if you can give some advice. My husband has had a brain stem stroke. He has been improving slowly. However, he was placed in a nursing home. He had been there for 17 days. He developed a collapsed lung and chest infection. He was admitted to the hospital in April and chest had been treated. He had several infections while in hospital. He’s also PEG tube fed, and there seems to be an issue with the PEG feeding, he was not keeping the feeds down. So, they put the PEG further down in the lower bowel, which he seems to be tolerating the feeds now. He’s now ready to go back home.”
Now also, this is just a side note, so when they put a PEG further down into the lower bowel, it’s often called the PEJ, percutaneous endoscopic jejunostomy tube. It goes into the duodenum, not in the stomach. If there’s absorption issues in the stomach, you can place the feeding tube lower into the jejunum and then it can absorb the feeds there. The feed regime needs to be changed. It’s just as a side note that you understand what this lady is talking about here.
So, I’ll continue with Annette’s email, “He’s now ready to go back to the home. The doctor of the home says he will not accept him back unless the family signs a peace document stating he’s not to be admitted to hospital should he become unwell. We as a family have not agreed to sign this because everyone needs to be treated if they are unwell. The family have agreed to palliative care because they say he has long-term medical issues and agree to treat him at home first should he become unwell before going to hospital? He also has a tracheostomy. I feel we are being pressured into signing this peace document. I don’t believe anyone should be pressured into doing this. Am right on saying this? From Annette.”
Oh, I’m so sorry Annette, to hear about your situation. Well, I think this ties right in with today’s topic. I mean, if your husband has a PEG tube and the tracheostomy tube and they’re pressurizing you for palliative care, it means they’re trying to deny you Intensive Care at Home. Now, you have not shared which country you are in. I do not know where you are. You have not shared the country you’re in, but clearly your husband needs Intensive Care at Home and that may include palliative care. But I also know for a fact that with Intensive Care at Home, palliative care is no longer needed because we keep people alive, that’s part of what we do.
Obviously, if you don’t want that and if you want palliative care, fair enough. I’m not here to make a judgement, I’m just giving you options. In your case, it sounds to me like your husband needs to go home with proper care, and I’m not surprised that he develops a collapsed lung in a nursing home. Do not send your husband to a nursing home if you can work with us, Intensive Care at Home. So, I wouldn’t sign anything.
What I would do is advocate for Intensive Care at Home and take him home. That’s what I would do if I was you, but I do believe that the next step here is for you to contact me directly at intensivecareathome.com, and then I can walk you through the steps. Depending on if you’re in Australia, we can help you one way or another, but even if you’re in another country, we can help you. We’ve helped clients in other countries to go home with intensive care or more similar type services. Don’t sign anything, do not agree to palliative care and work towards getting your husband home. That would be my advice where we are to take this further, Annette.
Let’s move on to the next question. Question from Tracy, who says, “Do you provide home care services for TPN (Total Parenteral Nutrition), dressing changes, and pathology or blood pathology checks, i.e., blood draws?” Yes, Tracy, we are. We have clients at home that are on home TPN. Now, for any of you’re watching, if you’re wondering what’s TPN is, TPN stands for Total Parenteral Nutrition. It’s another term for intravenous nutrition. So, we’ve talked about PEG tubes before. If for whatever reason your loved one can’t tolerate PEG feeds or nasogastric tube feeds for whatever reason, maybe they have decreased gastric motility, they have gastroparesis, they have absorption issues, they’ve had some form of abdominal surgery and parts of the bowel, or the guts removed or whatever the case may be, then TPN is absolutely an option, and we can do that.
So, with TPN or intravenous nutrition, patients need a PICC line (Peripherally Inserted Central Catheter), a central line, or a Hickman’s line or sometimes a midline, and then TPN can be given. When you go home with a midline or a PICC line or a central line or a Hickman’s line, you need, again, the skill of a critical care registered nurse to manage that line because those lines are usually put in and used in intensive care. Again, going home with the PICC line and TPN is the exception to the rule, but it does happen, and we have looked after a number of clients at home with home TPN. Again, that is bread and butter for us.
Now, Tracy is also asking, she’s talking about dressing changes and blood draws. Yes, absolutely. So, when someone has a PICC line or Hickman’s line, central line, or midline, they need dressing changes once a week. They also need the line managed by flushing the line that it doesn’t block. The last thing you want is line blocking because if it blocks, patients are back in hospital in no time. So, that line needs maintenance at least twice a day with unblocking it, flushing it, sterile connection, and disconnection of the TPN. You need an infusion pump, and then with the line, we can also do the blood tests. So, I hope that answers your question, Tracy.
Then, let’s move on to the next question, which is from Carly. Carly says, “Things I’ve seen and experienced in the ICU and hospitals staff is something like a plot of a horror movie. I took my daughter home and care for her by myself until recently they said, I can get help from my family members and they can get paid for it. They don’t want to give services to my daughter and try to trick me into doing things that would kill my daughter as if I don’t do my own research and call them on it. They really don’t like that I do my own research. The doctor even told me that he can refuse medical care and medications refills and make sure all other doctors do not give her care because it’s wasting resources.”
That’s terrible, Carly. I’m very sorry to hear that, and that’s very unethical if that’s what you are experiencing, and I’m constantly shocked by what’s happening out there in the community. I would still hope in 2023 that most doctors and nurses are ethical and do the right thing for patients and families. That they are there to help prolong life whenever possible and cure people whenever possible. But I also know that many of our families report something very differently, a very stark reality.
I only want to make a comment here of the recent case that I was made aware of actually just only one week ago. If you Google Grace Schara, that’s Grace, G-R-A-C-E, Schara, S-C-H-A-R-A, I should say, the late Grace Schara. Grace Schara was a 19-year-old girl with Down Syndrome who was in ICU on a ventilator with pneumonia. The ICU made her DNR without family consent, and she passed away from what the family thinks was murder. They are the family’s words, not my words. You can Google Grace Schara.
The family has launched a website there to raise awareness about her case. Her dad’s name is Scott Schara. I hope that I can get Scott on one of my podcasts in the next few weeks. He’s already agreed to that. I hope I can schedule a time. Scott, if you’re watching that, please reach out to me with a good time I’ve emailed you. I can’t wait to talk to Scott because it’s a very sad story, what’s happened there, but it’s also unfortunately what we’ve disclosed over the years with Intensive Care Hotline in particular that there are some unethical people out there and it almost feels like its population control and not what’s in the best interest of patients and families.
So Carly, I can concur with you what you are seeing there, and unfortunately we’ve seen it, but do not give up fighting. You can’t give up the fight just because things are hard. Keep speaking up, keep fighting for what you know is right.
Next question from Devon. Devon writes, “Thank you, Patrik, for your incredibly valuable information, assistance, and advice. My partner just came out of ICU to ward bed. He had an accident at home a few weeks ago, which left him with a fractured pelvis in four places, four broken ribs, and a few fractured vertebrae. He then developed a DVT (Deep Vein Thrombosis) and subsequently several small but life-threatening pulmonary embolism. Your videos helped me understand how ICU works and what decisions they may ask us to make. Fortunately, we didn’t have to make any of those decisions, although knowing that there’s advocacy for ICU patients makes the process much less stressful and less lonely. Thank you, from Devon.” Well, Devon, you’re most welcome and I’m very pleased to hear that you were able to find help just through the videos and the information we put out there. I really appreciate your feedback on that.
Next question from Candice. Candice says, “My boyfriend has been in a coma for 17 days with blood draining from the brain, high blood pressure. They have a tracheostomy in his throat now and he won’t wake up. He’s breathing on his own with the help of the tracheostomy. What is going to be the outcome?” Well, Candice, that’s a good question, but it’s also a question that I can’t answer you straightforwardly without having more information, without having access to the medical records. If he’s got blood draining from his brain, it sounds to me like he might’ve had a hemorrhagic stroke. He might’ve been in a head strike in a car accident. He might’ve fallen off a roof. I don’t know what got your boyfriend in this situation.
I would imagine that 17 days in ICU after a traumatic brain injury, which sounds like he’s had, is way too early to say where this is going. You should definitely not give up. You haven’t shared how old your boyfriend is, but you can’t give up here. The good news is he’s still alive. What I don’t have here, in any case, I never have a quick fix for people. Sometimes I do, but in most cases, it’s a long-drawn-out process when it comes to cases like this. You have to be patient, but you can’t give up. The good news is your boyfriend is alive. That is the most important part here and get the medical records to us and then we can help you and really break this down for you, that would be my advice here.
Then, next question from Shirley. Shirley says, “Hi Patrik. My dad is currently in ICU. I have been told that his brain has been affected due to anoxic brain injury when he fainted, which lasted about 25 minutes. Firstly, I find it odd considering that CPR was done immediately. He has had movements and even opened and closed his eyes briefly, and he teared. He also moved up and got red when they were moving the breathing tube. The neurologist is saying it’s just jerking movements. They’re basically pushing for us to stop treatment, but I still find some things very, very odd. From Shirley.” Well, Shirley, if you find it odd, you should trust your gut feeling here, and if your gut feeling is telling you something’s odd here, you need to get help. What that means is you should be contacting us. We can talk to the doctors and nurses directly. When I talk to them, I will ask questions you haven’t even conceded asking.
You are probably right if CPR was done immediately. I mean, there’s no guarantee that CPR is efficient. There’s never a guarantee for that of course, but it’s a good sign that CPR was done immediately. If he’s opened his eyes and his tearing, that’s a good sign. You also should be asking if he has any seizures. Seizures are not a good sign after cardiac arrest and potentially anoxic brain injury, but if he doesn’t have seizures, that’s a good sign. Do not let anyone push you to stop treatment if you don’t feel like it. You have a right to demand continuing treatment. That’s a basic human right, so do not give up here.
Many patients have come out of similar situations like that. Many patients had a tracheostomy, got slowly weaned off the ventilator, got slowly weaned off the tracheostomy. The same might happen here for you and for your husband. Do not give up here under any circumstances, and if you need help, you know where we are. But even, let’s just say even your husband has an anoxic brain injury, that doesn’t mean he won’t have any quality of life. Maybe he wants to live. Maybe you want him to live. Don’t let other people sway you about your opinion and about what you want as a family.
Let’s move on to the next question. Question from Sims. Sims says, “ICU wants to take my mom off the ventilator and send her to acute living, and our family wants to keep her on the ventilator since it’s only been six days.” Well, six days in ICU is not very long. Now, what might happen here is maybe they want to take your mom off the ventilator because she’s ready for it. If she’s ready to be coming off the ventilator, well, I argue you should jump on it. But if she can’t come off the ventilator, then she should be having a tracheostomy first before she’s going anywhere else. You haven’t made any mention.
The way I interpret your question is that your mom is on a ventilator, and it’s only been six days. She doesn’t have a tracheostomy yet. She won’t be going anywhere without a tracheostomy. They can’t just send her out of ICU without a tracheostomy, assuming she can’t come off the ventilator.
If she can come off the ventilator, well then maybe acute living and rehabilitation might not be a bad thing, but again, I don’t have enough information here. So, it comes down to that the biggest challenge for families in intensive care is that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights. They don’t know how to manage doctors and nurses in intensive care, and this is exactly what you’re dealing with here, Sims. You don’t know what you don’t know. So, I hope that answers your question.
Six days in ICU is not a long time. I doubt that your mom has a tracheostomy already, I doubt that. So therefore, she won’t be going anywhere with a breathing tube anyway, so do your research. The best thing for you to do is contact us at intensivecareathome.com or intensivecarehotline.com. Call us on one of the numbers on the top of our website or send us an email to [email protected] or [email protected].
There’s time for one more question, assuming it’s not too long. From Sumit. “Hi, Patrik. I just want to know what other chances of my mother’s recovery? I have seen it has been more than seven months now she’s unconscious.” Well, again, Sumit, you are giving me very limited information here. I would need to know a lot more in order to determine what your mom’s recovery is going to be. If there are any chances for it, there may not be. I don’t know, but I don’t have enough information from you.
Again, when you contact us, please give us as much information as possible. Ideally, have access to the medical records or make sure that you set it up in a way that myself, that I can talk to the doctors and nurses directly. That’s when I can do my best work. I can’t do my best work with limited information.
Question is, why is your mother unconscious? Is she breathing? Is she opening eyes? What’s her Glasgow Coma Scale like? What led her to this situation to begin with? Without any of that information, it’ll be very difficult for me to answer your question.
So, let’s wrap it up here today. So, that was will a tracheostomy work in the community? My presentation from today, I hope I’ve made myself clear. If you have a loved one in intensive care or you are a patient in intensive care and you want to go home with a tracheostomy or a ventilator or both, but even if you want to go home with a BIPAP, CPAP, home TPN, you’ve come to the right place, contact us at intensivecareathome.com.
Don’t worry about the funding, just talk to us. We can set you up with an NDIS support coordinator if you are in Australia. But even if you are in the U.S., U.K., New Zealand, wherever, please contact us. We can help you, point you in the right direction.
If you are a patient or family at home and you don’t have enough support, maybe your loved one. You don’t feel safe, your loved one is bouncing back between hospital and home all the time because no one can keep you more predictably, I encourage you to contact us, that is what we’re doing best. We are keeping our clients at home predictably.
If you are an NDIS support coordinator and you’re watching this and you want to know more about our service, you want to know how does it exactly work? How do NDIS support coordinators get funding for nursing care for those patients? Please contact us, we can help you. We’re also in the process of employing our own NDIS support coordinator team. If you have experience with nursing care and the NDIS in particular, we want to hear from you as well.
Now, if you are a critical care registered nurse and you are looking for a career change, for a job opportunity, we want to hear from you as well. If you’re interested in working in the community and you think you have what it takes working with highly vulnerable clients, we want to hear from you as well. Please contact us at intensivecareathome.com. Call us on one of the numbers on the top of our website or email us at [email protected]. We currently provide jobs all over Australia, so please don’t be shy reaching out to us. Also, have a look at our career section on intensivecareathome.com.
If you are an intensive care specialist, we want to hear from you as well. We are currently expanding our medical team to increase the number of clients we can take home, make a real difference to people’s lives.
So, if you’re an intensive care specialist in Australia, please contact us as well. If you’re a hospital executive watching this, we want to hear from you as well. You might feel challenged having ICU bed blocks or ward bed blocks because of tracheostomy. If you’re worried about safety for these patients in the community, we can alleviate that concern because we can keep our clients at home predictably.
So, let’s wrap it up here.
Well, if you find these videos valuable, give it a thumbs up, subscribe to my YouTube channel, click the notification bell, share the video with your friends and families, and comment below what you want to see next, or what questions and insights you have from this video.
Also, have a look at our membership for families in intensive care and Intensive Care at Home at intensivecaresupport.org. There, you have access to me and my team, 24 hours a day, in a membership area and via email. We answer all questions, intensive care and intensive care at home related.
We also offer NDIS nursing assessments and also, we offer medical record reviews in real time. If you need a medical record review in real time, please contact us as well. We also offer medical record reviews after intensive care, if you have unanswered questions, if you need closure, or if you are simply suspecting medical negligence.
We are now coming to the hour mark, and I’m going to wrap this up right now. Look out for another YouTube live next Sunday, 10:30 AM Sydney Melbourne time. 8:30 PM Eastern Time in the U.S., North America. 5:30 PM Pacific Time, and it is starting at 1:30 AM U.K. time, very early for our U.K. audience, but you can watch it on a replay.
Thanks again and I will talk to you in a few days. Take care for now.
This is Patrik Hutzel from intensivecareathome.com, and I will talk to you in a few days.
Take care.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Sunbury, Bendigo, Mornington Peninsula, Bittern, Patterson Lakes, Frankston area, South Gippsland, Drouin, Warragul, Trida, Trafalgar and Moe as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran Affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care at Home, and I’ll see you again next week in another update.








