Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
WHAT IS THE PURPOSE OF A TRACHEOSTOMY?
You can check out last week’s blog by clicking on the link below this video:
https://intensivecareathome.com/what-is-the-purpose-of-a-tracheostomy/
In today’s blog post, I want to answer a question from one of our clients.
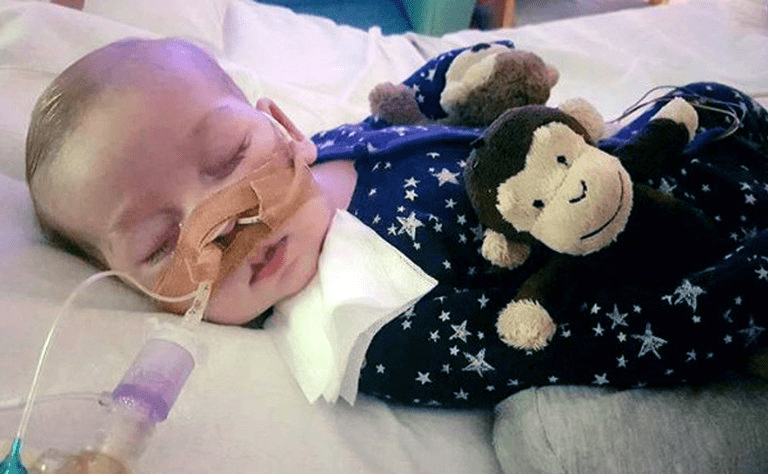
Is a Tracheostomy Going to Work?
Hello and welcome to another Intensive Care at Home and intensivecarehotline.com livestream.
Welcome to the show and I also want to welcome everyone that’s watching this stream on replay. As always, you are welcome to type in your questions into the chat pad. I will go through today’s topic and then I will also answer questions that came in during the week. So, let’s get started with today.
Before we get started with today’s topic, just a couple of housekeeping issues. In case you are wondering what makes me qualified to talk about today’s topic, which is, “Is a tracheostomy going to work?” It’s a question we get quite frequently from our readers and clients.
Before I go into today’s topic and break it down, what makes me qualified to talk about today’s topic? I’m a critical care registered nurse and I have been working in critical care intensive care for over 20 years in three different countries. I have been working as a nurse unit manager for over five years in intensive care. I’m the founder and managing director of Intensive Care at Home. With Intensive Care at Home, we provide a genuine alternative to a long-term stay in intensive care for predominantly long-term ventilated adults and children with tracheostomies. We also provided a genuine alternative to a long-term stay in intensive care for adults and children on BIPAP (bilevel positive airway pressure), CPAP (continuous positive airway pressure), or non-invasive ventilation. We also provide Home TPN (total parenteral nutrition), home IV infusions including electrolyte management such as potassium infusions at home, also IV antibiotics at home. We also do NDIS (National Disability Insurance Scheme) nursing assessments, or we provide nursing assessments in general. That’s what we do in a nutshell with Intensive Care at Home.
I’m also the founder and managing director of intensivecarehotline.com. Intensive Care Hotline is a consulting advocacy service for families in intensive care. We have been consulting and advocating for families in intensive care all around the world, for the last 10 years. You can find more information at intensivecareathome.com and intensivecarehotline.com.
With Intensive Care at Home, we are also now providing NDIS specialist support coordination. We are currently operating all around Australia with Intensive Care at Home. We are NDIS accredited. We are a TAC (Transport Accident Commission) provider, iCare in New South Wales provider, NIISQ (National Injury Insurance Scheme, Queensland) provider, DVA (Department of Veteran Affairs) provider all around Australia. We also have received funding through some public hospitals and departments of health. So, either way, if you have a loved one in intensive care and you want to go home for the conditions that I mentioned, please contact us and we can help you.
Now, without further ado, let’s talk about today’s topic, “Is a tracheostomy going to work?” It’s a question we get quite frequently, but the answer is that it really depends. It depends on the goals of care. So, let’s run through a few scenarios when a tracheostomy is working or what should be the goal.
For any patient in intensive care that’s on a ventilator with a breathing tube/endotracheal tube who’s in an induced coma, let me be very clear here. Once again, the goal should always be to wean someone off the ventilator and the breathing tube/endotracheal tube before we even talk about the tracheostomy.
It appears to me like a lot of our clients have come to us or read our stuff on our websites. They want to know about a tracheostomy and that’s a good thing, but they miss one crucial step. They’re missing holding intensive care teams accountable to get their loved ones off the ventilator and the breathing tube in the first place. They don’t know what to look for.
I’ve been saying it for the longest, the biggest challenge for families in intensive care is that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care.
So, before you are even thinking about is a tracheostomy going to work? The first question that you need to ask is the intensive care team doing everything beyond the shadow of a doubt to get your loved one off that ventilator in the breathing tube? That is the very first question you need to ask.
Once you’ve answered that question and you probably couldn’t answer that question without getting a second opinion, which is what we can give you here with Intensive Care at Home and with Intensive Care Hotline, only then once you can confidently say, “Yep, they’ve done everything beyond the shadow of a doubt. It’s not working. They can’t get my loved one off the ventilator and here are the reasons why.” Really, to answer that question, you need a crash course in intensive care. The devil is in the detail in intensive care. You can really only work in intensive care, whether you’re a doctor or a nurse after years of training and even then, you need to learn on the job day by day. Only then do you really know what you’re talking about. But again, we can walk you through that step-by-step here at Intensive Care Hotline and Intensive Care at Home.
So, once you can confidently say, “Well, they’ve done everything beyond the shadow for that, my loved one is not going to get off that ventilator with the breathing tube,” then you can ask the question, “So, if we do a tracheostomy, is it going to work?” So, then you can ask that question.
So then, and still I say, “Well, is a tracheostomy going to work?” Again, it depends. It depends on the goals of care. So, what are the goals of care? What should be the goal of care when someone is in intensive care and needs a tracheostomy? Once again, same goals of care to what I said right at the start. The goal of care for a tracheostomy should be to wean your loved one off the ventilator with a tracheostomy and then get rid of the tracheostomy. That should be the goal of care.
Now, there are exceptions to the rule, of course. Exceptions to the rule are, especially for our Intensive Care at Home clients who have, let’s just say cerebral palsy, who have motor neurone disease, who have C1, C2 spinal injuries, they would need a tracheostomy for the rest of their lives.
Other goals of care could be do you want a tracheostomy for your loved one or does your loved one want a tracheostomy to have end-of-life care at home to prolong life and then go home for palliative care? Which is also something we’ve done with Intensive Care at Home. So, it really depends on what the goal of care is.
Let’s take someone with Guillain-Barré syndrome in ICU. They often end up with a tracheostomy, those patients. Then, they stay in ICU for months on end to be weaned off the ventilator. There’s no need for that. They could go home with our service Intensive Care at Home. Absolutely no need for those patients to stay in ICU for 6, 9, 12 months sometimes and going through that very, very slow respiratory wean that could be done so much more effectively at home in a much more conducive patient and family-friendly environment because in ICU, there’s no day or night rhythm. There’s daylight every day. There’s noise every day. There’s no privacy, no dignity. There’s no quality of life in intensive care. Again, with Intensive Care at Home, there is a much better opportunity to do those slow respiratory weans at home.
So, can you now already see where is a tracheostomy going to work? I should have probably phrased the question differently from the start. Is a tracheostomy going to work for the goals of care that are set out for your loved one? You might be someone watching this with a tracheostomy, and you might be wondering, is it still working for me? What are my goals of care? Is there a better option? and so forth.
So, let’s take another example. Let’s just say someone goes into intensive care with a stroke. If they go into intensive care with a stroke and they can be weaned off a ventilator, but they’re unable to swallow or they’re unable to protect their airway, they’re unable to cough, they don’t have a good strong cough, they can’t clear their secretions, then a tracheostomy, but not necessarily a ventilator might be the right next step. So, can you see it all depends on the goals of care.
Other examples could be I’ve seen many patients in intensive care that had failed lung transplants, or they had a lung transplant that worked for quite some time and then they come back into ICU with maybe rejecting the organ or with complications and then they often die a very slow and terrible death in ICU for a number of reasons. The much better option would be for them to go home and have palliative care at home. Again, many of those patients end up with a tracheostomy. It would be so much nicer and also more cost-effective for these patients to be looked after at home and have palliative care and end-of-life care at home instead of in an ICU bed where there’s lots of noise, no day and night rhythm, lots of noise, no privacy, no dignity. Families live in intensive care day and night. It costs a lot of money. It costs five to $6,000 per day and it’s blocking an ICU bed that could be used for someone that’s more critically unwell, more acutely unwell. Maybe surgery gets cancelled because there is no ICU bed.
So, if you’re a hospital executive watching this or an ICU consultant, or an ICU bed manager, or a hospital bed manager, you know exactly what I’m talking about. You know that your ICU beds are blocked. You know there’s a long-term patient in there and you know that a service like ours can help you manage those bed blocks. You also know that the cost is approximately 50% of the ICU bed. But you can’t really weigh in monetary terms what we do because how much is it worth for you to have a free ICU bed and you can do surgery tomorrow? You can eliminate your ED bypasses. You can get people through ED, through the emergency department or emergency room and get them back into ICU. No brainer.
It’s a win-win for everyone whether it’s for patients, whether it’s for families, whether it’s for hospitals, whether it’s for ICUs, whether it’s for your staffing levels in hospitals because if you staff for an ICU bed whether it’s doctors, nurses, physios, you do the math. You need those staff for other patients. You know that.
So, it really comes down to goals of care when it comes to a tracheostomy, whether you should have one or you shouldn’t. The reality is that when you are at those crossroads in ICU where you are asking the question, should a tracheostomy be done or not? Well, the reality is that if a tracheostomy isn’t going to be done, that death is probably inevitable either in the short term or in the medium term because take someone with a stroke for example.
If they can’t swallow or if they can’t manage their secretions, if they can’t protect their airway in the short or in the long term, people will be drowning in their own secretions and will end up with an aspiration pneumonia or with pulmonary edema, and that’ll only lead to more complications and eventually will end up in death.
So again, it comes back to goals of care. It comes back to do you have an advanced care plan? Do you have an advanced care directive? What do you want in certain situations? And if your advanced care directive, for example, says, you don’t want a tracheostomy, then so be it. I’m not here to make any judgements. I’m here to give people opportunities to get people to think about what are the options that are available to me.
So, is the tracheostomy going to work? It’s a very general question. Then, there’s also some logistics maybe around that. Most of the time a percutaneous tracheostomy is possible. So, what that means is a percutaneous tracheostomy is often done at the bedside in ICU. The intensivist or intensive care specialists will do that with their colleagues. It’s a reasonably quick procedure. It takes 30 to 45 minutes for someone who’s skilled. It often goes hand in hand with a bronchoscopy. Then, on the other hand, sometimes patients have a surgical tracheostomy as well which will be done in the operating room, or the operating theatre done by an ENT surgeon. Either is fine. The percutaneous one is usually the quicker one, and the surgical one is possibly a bit more stable in the beginning especially. But if someone needs a tracheostomy in the long run, both forms of tracheostomy are pretty stable.
With a longstanding tracheostomy stoma, it doesn’t collapse usually quite easily. So, coming back to the goals of care for someone with a tracheostomy. Again, is it something that should be used to get someone off the ventilator in ICU quickly in order to take off sedation? That is the primary goal in ICU. When someone in ICU is having a tracheostomy one of the primary goals is take away sedation because an induced coma, it’s often necessary for patients with a breathing tube or an endotracheal tube and then take off sedation, mobilize someone as quickly as possible and wean them off the ventilator. That should be the ideal scenario. That should be the ideal scenario.
Then, if that can’t be achieved in case of some neurological conditions, like I mentioned, stroke, motor neurone disease, C1, C2 spinal injury, then it’s really a long-term treatment option to live a better quality of life at home. But again, the goal should always be to have that tracheostomy and the ventilator removed in most cases. That is your aim, your goal in the long run.
Does it work in the long run? Let’s just say God forbid, once again, your loved one does need a tracheostomy for the rest of their lives, does need a ventilator for the rest of their lives, then what? What do you need to do next? Well, that’s where Intensive Care at Home comes in.
We have helped countless patients and families and intensive care units to eliminate some of their bed blocks by taking patients home directly from ICU because the tracheostomy and the ventilator and sometimes the non-invasive ventilation keeps them in ICU and they can’t go anywhere within a hospital because it takes intensive care, medical and intensive care nursing skills to look after patients on ventilation, tracheostomy and so forth.
The only way to take them out of ICU is really to take them home, that’s what we help with Intensive Care at Home where we basically replicate the ICU bed, the intensive care bed in the home with 24-hour intensive care nursing at home where we send our ICU nurses, pediatric ICU nurses and sometimes emergency nurses into the home to manage the tracheostomy and ventilation. Now, I can assure you that if you’re trying to do this yourself or if you think you can hire support workers or even nurses without ICU or ED experience, you’re doomed to fail. Patients have died in the community. Many patients have died in the community because they didn’t have the right skill level.
I can verify that not only by unfortunately having or knowing of patients that have died in the community that had inadequate support, didn’t have the support with ICU nurses and they died because either family members, support workers, even general registered nurses without ICU or ED experience could not manage medical emergencies and people died before an ambulance could even arrive. So, it’s a very tricky situation.
I understand on the one hand, you and your family are stuck in ICU, and you want to go home as quickly as possible, and it often can’t get quick enough by the same token. Have a look at our website at intensivecareathome.com. Have a look at our evidence-based Mechanical Home Ventilation Guidelines. There, you will actually see that Mechanical Home Ventilation Guidelines say that only intensive care/critical care nurses with a minimum of two years hospital critical care nursing experience can make a safe transition at home and that the intensive care bed needs to be replicated in the home to make this safe for someone with a tracheostomy, for someone with a ventilator and a tracheostomy, for someone on BIPAP, CPAP ventilation.
So, this is evidence-based. It’s a result of over 25 years of Intensive Care at Home nursing in Germany in particular where I worked with Intensive Care at Home as well. Now, also a result of the last 10 years of Intensive Care at Home nursing in Australia where I set it up here because once again, patients that didn’t have 24-hour intensive care nurses at home trying to go home with ventilation tracheostomy either bounce back into ICU or worse, they die because once again, we have evidence that medical emergencies could not be managed by, again, family members. How traumatic for family members to see their loved ones going into a medical emergency and then seeing them die in front of their very eyes because they didn’t have the support, because funding bodies like the NDIS in particular didn’t want to fund what’s evidence-based and it’s actually a crime. That is murder. That is a crime.
I hope Bill Shorten your listening to this because that is actually what’s happening on the ground. You’re making all these promises around, “Oh yeah, we fixed the NDIS.” You haven’t fixed anything. You haven’t fixed anything. You’re just blowing hot wind out there without recognizing and without acknowledging that people have died, and it needs a quick fix from the NDIS, an urgent fix before things are getting worse. So, there’s the evidence.
Also, from our perspective, we are the only service provider in Australia in 2023 that has achieved accreditation for Intensive Care at Home, which includes obviously mechanical ventilation and tracheostomies. There’s no other service provider in Australia in 2023 that has achieved that. If there is someone, I’d like to hear from you, but as far as I’m aware, from my research, I haven’t seen any of it.
So, anyone in this space is really flying blind and it is like flying an airplane with a cabin crew instead of the pilot. Well, you know what will happen if you’re flying the airplane with a cabin crew instead of the pilot, there’s probably going to be a crash waiting to happen. This is exactly what we have seen that at least 5 ventilated tracheostomy adults and children have passed away in the last 7 to 8 years in Australia that weren’t funded for, that weren’t looked after by accredited healthcare services like we are for Intensive Care at Home and it’s causing so much pain for families. Children have lost their lives. It is absolute insanity, and it needs a fix.
We are bringing the standards in the community because there’s no other provider that brings in standards into the community. Look at our Mechanical Home Ventilation Guidelines. They’re the gold standard. That’s the quality that is needed in the community and not a cheap solution. We are cutting the cost of an ICU bed by 50%, but you can’t cut the cost of an ICU bed by 80% by bringing in people that are support workers or general registered nurses that have no idea what to do with an artificial and unstable airway, which is what tracheostomy is.
So, to come back to the original question from today, is the tracheostomy going to work? Now, that I’ve broken down to when a tracheostomy will work from a hospital point of view, now I need to elaborate on is a tracheostomy going to work in the community? I might actually make a YouTube live just about that topic. I actually need to write that down. I often get good ideas when I’m doing these YouTube lives, so I should write that down. Is a tracheostomy going to work in the community?
Now, that you’ve heard me saying, it’s a clear yes. But it’s only going to work with standards, with quality standards that we bring in with Intensive Care at Home. That’s the only way it’s going to work if you bring in quality standards, if you bring in intensive care nurses into the home, if you bring in third party accreditation for Intensive Care at Home, otherwise it’s not going to work.
Now, for anyone wondering or because we know there are some operators out there that look after ventilated and tracheostomy patients in the community with support workers, with registered nurses that are not ICU trained or sometimes with enrolled nurses, they’re not even registered nurses. So, let me ask you this, if supposedly a support worker, an enrolled nurse or a general RN without ICU experience can look after a ventilated/tracheostomy patient, why are ventilated and tracheostomy patients in ICU in a hospital? Why are they not in a hospital ward looked after by support workers or by family members or whatever, people you want to throw into the mix there? I’ll let you answer that question, but I think where that leads to is I should be making a video about is a tracheostomy going to work in the community? I think that’s another YouTube live here very soon. So, I think that I would hope concludes today’s topic.
Now, I can go back to all of the questions that came in during the week and there’s quite a few of them. If you have any questions to today’s topic about is a tracheostomy going to work? Type them into the chat pad and then we can go from there.
Like I said before, I want to highlight that again. Do not underestimate using a tracheostomy for end-of-life care as well. So, here’s the situation where we used or one of our clients used a tracheostomy for end-of-life care. We had a client a while ago, she was a 69-year-old lady. She was unfortunately in a motor vehicle accident, and she ended up in a trauma ICU, ended up with a tracheostomy, ended up in rehab and by the same time this lady unfortunately had chemotherapy for breast cancer as well. She had the will to live, but she knew unfortunately she didn’t have a lot of time left, but she was desperate to go home. So, we managed to take her home in spite of her having the tracheostomy and in spite of her having the chemotherapy and in spite of her having many, many medical issues, many complications, we managed to keep her home for the last 12 months of her life, which was her wish and she passed away at home.
It really depends on what goals of care you have. It’s not a one size fits all. Definitely not a one size fits all. It can be used for many, many circumstances when it comes to tracheostomy and ventilation. The most important part is that if you do decide to go down that track of a tracheostomy, know there’s help in the community and know that with that help in the community you can go home. You don’t need to stay in intensive care and that is very important for you to know and understand that there’s no need for you to stay in intensive care. You can go home with our service Intensive Care at Home.
Also, if you’re watching this and for example, you are an NDIS support coordinator, you might be wondering, is a tracheostomy going to work? I hope I’ve given you some insights here as well, that a tracheostomy is absolutely going to work, especially with intensive care nurses in the community within an accredited service like Intensive Care at Home and tracheostomy is absolutely going to work. Some of our clients have lived very good qualities of life at home for many years now and they’re very happy to be alive.
Sometimes I know families are asking the questions, is there any quality of life? Well, there definitely is quality of life at home. Maybe the question today should have been, is a tracheostomy going to work and will you have quality of life? But that was the very question we had been asked by a reader, is a tracheostomy going to work? So, I took that and ran with it.
Let’s go back to some questions that came in during the week. So, here’s a question from Vinod who says, “My mom is 73 years old, has been in ICU for 35 days now. Her history goes like this. She’s a COPD (Chronic Obstructive Pulmonary Disease) patient, Type 2 respiratory failure on oxygen BIPAP at night. She has been in this condition for two years now. She also is having issues with kidney disease. Body swells up at times.
She used to get admitted to the ICU mostly every six months. When we got her admitted this time, she was detected with H1N1 virus was first admitted to respiratory ICU and eventually moved to medical ICU.
She underwent the tube insertion and was on a ventilator. After a slight recovery, she was moved back to respiratory ICU. After a few days her condition deteriorated further, and we were told she got sepsis. She was again shifted back to medical ICU. Antibiotics were given.
After day 10 to 15, she was again moved back to respiratory ICU. She was conscious and started talking in between. However, lately her hemoglobin levels went low as low as 5.8 and she currently is having blood transfusions and albumin injections are administered.
Right now, they told me about acute kidney failure and issues with the liver. They moved her to end-of-life care with only necessary support for survival. I’m checking if dialysis is an option here. What’s the ideal that we should look at this moment?”
Well, what a great question and what sad story? Well, it keeps coming back to two things. It keeps coming back to our question today, is the tracheostomy going to work? That’s one question I want to throw in there. The next answer to your question is dialysis an option? Absolutely. Assuming she’s hemodynamically stable, dialysis is absolutely an option. Especially if she’s got Type 2 respiratory failure and she was on oxygen and BIPAP overnight at home, it would be very difficult for her to get off that ventilator.
At the moment with kidney disease, she’s probably in pulmonary edema. She’s got H1N1. She had a tube insertion. Now, if she’s not having a tracheostomy and you’re moving her to hospice care, she’s probably going to pass away very, very soon. So, here’s the thing. When does dialysis work? Dialysis works when someone is hemodynamically stable. So, what happens is when someone goes on dialysis or hemofiltration, which is the smoother and more gentle approach to get the kidneys going again, assuming someone is hemodynamically stable in ICU, you can get them on hemofiltration or dialysis. It works.
If someone is hemodynamically unstable and that includes your mom having a low hemoglobin. So, you didn’t mention anything that your mom is on inotropes. So, that’ll be very difficult to get her on dialysis if she’s on inotropes and she has a low hemoglobin. Now, assuming she’s getting the bloods topped up and then it should be fine. Assuming she’s still not on inotropes or vasopressors, assuming she’s still hemodynamically stable, then dialysis should absolutely be an option. I do believe that you haven’t been given all options. The only option you’ve been given is end-of-life care and that’s a one size fits all solution for ICU in this situation.
You’re talking about acute kidney failure. You’re also talking about issues with the liver. She’s probably been taking a lot of medications since she’s been in ICU. That will affect the kidneys and the liver. So, let’s just assume she’s been in an induced coma on and off. You haven’t mentioned that, but I presume if she’s got a breathing tube, she would’ve been in an induced coma most of the time. She’s been on heavy sedation, heavy opiates that can impact on kidneys and on liver. So, in order to offload the liver in particular, get rid of all of the sedatives, but that can only really happen if she has a tracheostomy or even better get extubated. But it doesn’t sound like to me extubation wasn’t an option here. So, this is the challenge that you’re facing.
I do believe you’ve been misled from the start and that’s why I keep saying over and over again, intensive care teams are only telling you half of the story unless you have professional guidance while you have a loved one in intensive care. This is what we do with Intensive Care Hotline. We walk you through the experience in ICU, step by step and many families come to us when it’s too late. You can’t come to us when it’s too late. You got to do your research day one.
Then you’re also talking about sepsis. Now, you didn’t share where the sepsis is coming from. Is it from the H1N1? H1N1 is a respiratory virus. I’m pretty sure it’s swine flu, which is a bacteria area. It is a virus. Anyway, so that’s the background here. So, you need to educate yourself right from the start. You can’t be dabbling around because now you are cornered. Where do you go from here? If you had come to me two weeks ago, I would’ve told you, “Well, this is probably what’s going to happen. Here’s why you will need to start advocating for a tracheostomy straight away, assuming you want your mom’s life prolonged, which sounds to me like you very much would like to.”
So, make sure she continues to get the blood transfusions. Make sure she’s continuing on the ventilation if that’s what you want, but now it is the time to make sure they know you’re talking to someone who knows intensive care inside out as they do and therefore advocate for the hemodialysis or hemofiltration as well as advocating for a tracheostomy and not for end-of-life care, assuming that’s what you want. It sounds to me like that this is what you want, otherwise you wouldn’t have reached out.
Let’s go to the next question, which comes from Zandy. Zandy says, “Hi, Patrik. My baby is 6 months old and he’s in ICU. She had a hole in her heart. She’s been ventilated since yesterday morning. What to expect?” Wow. I’m very sorry to hear that, Zandy. So, what to expect. So, what you’re not saying is that the hole in the heart lead to the ventilation and the tracheostomy.
So, is the hole in the heart the reason why your baby ended up on a ventilator? Let’s just assume it is. Let’s just say it’s some congenital heart defect, some septal defect. Either they need to fix the hole surgically, which I know they sometimes do that, sometimes they don’t. Especially if it’s an atrial septal defect, also known as ASD. It depends on whether it’s a small atrial septal defect or it’s a big one because a long term and a large one will damage the heart and the lungs, and surgery is often needed to get this repaired. If there’s a big hole, the heart won’t get enough oxygen supply, the lungs won’t get enough oxygen supply and other organs won’t get enough oxygen supply. Therefore, your child ends up on the ventilator. Therefore, the heart needs to be fixed, the hole needs to be fixed. Hopefully it’s not too big because otherwise your baby might end up on ECMO and hopefully that can be fixed very soon. Then, your baby should come off the ventilator.
If it can’t be fixed for whatever reason, surgically, your baby may end up in ECMO and then hopefully waiting for a heart transplant, waiting for surgery. Blood gases need to be checked very, very closely. But the sooner they can take her off that ventilator, the better it is.
Now, let’s move on to the next question from Mary. Mary says, “Hi, my dad is in ICU and has been for the last month at least or more. We are asking the ICU to continue ventilation so my dad can breathe. They have denied the request taking him off the ventilator on Thursday. He has a brain mass metastasized from his esophageal cancer, which was cured last August 2022.
He started getting severe headaches, got lost on the bus and could not get into his apartment and was confused. An MRI showed a brain tumor mass cancer growing larger. They did not do further chemotherapy and not sure radiation was done again. I had them bring him down for radiation. They said, could not as he might fall off the table or choke. So, it was a no-go.
Even an MRI was proving difficult according to medical staff, he would get combative, they said. When I first went to visit him, he was sitting up eating with a fork. Next time they had to feed him and his arms, and hands were shaking all the time like Parkinson’s disease.
A few months ago, he had been walking with a walker and was weak but was getting by. Not much talking however, from him.” If he’s shaking, Mary, he might also have some micro seizures, especially with a brain tumor.
“So, there’s not much talking from him. Then we took him home, but then he was so weak we had to bring him back to the ambulance in the hospital.
Then, they attempted to remove the ventilator about a month ago with very little success. He was given oxygen but at night could not breathe. He needed nasal surgery as he has deviated septum and a very crooked nose. Never got that done and so now he’s breathing through the ventilator. He’s hard of hearing too. So, I told them to speak up for him to do any commands you say he will not do, went on the ventilator and we took it off about a month ago. They had him in arm restraint so he would not remove the ventilator. I was terrified seeing my dad like that.”
Now, they’re saying they have done all they could for him. No facility will take him and that’s that. They’re pulling the plug this Thursday, has no chance to survive without ventilator, and we do not know where you can take him next.
We cannot afford a funeral and cremation, so I suggested to contact an attorney. Not sure whether the attorney will be clearing this. We also just hosted a memorial for my dad’s brother-in-law who also he had a very good relationship with, and he passed away in the meantime. So, I’m not sure how he had lung issues though.”
Now, she’s talking about things that are not relevant to the ICU admission. “We really hate to lose him in these circumstances. We have to try to get to another hospital for care, but we cannot afford the cost of transport by ambulance, however.
It’s just a nightmare for us and as a family and for me, myself and certainly for my dad as the ICU patient being treated this way. We had to go to a hearing to allow for nutrition for him via his nasogastric tube.
Recently, they repaired the PICC (Peripherally Inserted Central Catheter) going for nutrition as the line was kinked. For how long? I don’t know. His arm swelled up too from a blood clot back in May and we’ve just found out now they flushed out the PICC line. Now, the swelling is gone. My question is, would he wake up from his coma after the ventilator is removed on Thursday? Not even sure if he’s induced coma. They say no, it is the brain mass cancer taking him over and he will not wake up ever again. What are his options at this point?”
Well, the options at this point, Mary, are that he’ll have a tracheostomy and you do not give in and you want to continue treatment. Those are the options. Do not take no for an answer. If you want to take him home, for example, with a tracheostomy and a ventilator, again, come to us at Intensive Care at Home. Or if you want to spend more time with him, and even if that’s in hospital, we can help you advocate for a tracheostomy. No reason why he can’t have one.
It looks like your dad might be having end stage brain cancer, but that doesn’t mean you shouldn’t try prolonging his life assuming that’s what you and what he wants. That’s the bottom line. If you want to continue his life, get a tracheostomy done and take him home with Intensive Care at Home, and have end-of-life care at home and the ICU you will see might support you because they want to free up their beds, which is probably why they’re pushing for end-of-life care.
You can push for a tracheostomy and empty the bed. So, if you can bring it on that common denominator, you both want the same. You both want to free up the ICU bed. ICU wants to kill him or wants to let him go. Whereas you say, “Well, let’s do a tracheostomy and take him home.” Two different approaches with the same goal and it provides a win-win situation. So, I hope that helps. I hope that answers your question, Mary.
Let’s see if we have another minute for another question. This is a question from Jim. Jim says, “My daughter is in ICU and her United Healthcare Insurance will not approve her to go to a local hospital that can help her get weaned off the ventilator. What would you recommend?” Well, I would recommend you to stay in ICU because ICU is the best place for her to get weaned off the ventilator. I know you’re in the U.S. I can see that from your email. Keep her in ICU because the minute you consent to a tracheostomy and a PEG (Percutaneous Endoscopic Gastrostomy) tube, that’s the minute she’ll end up in LTAC (Long-Term Acute Care) and that’s when things will go really, really pear-shaped. So, it sounds to me like she’s in the right place anyway. So, why would you upset the apple cart? Assuming you are happy with the care that she’s getting there. But the minute she goes to LTAC with the tracheostomy, they won’t be able to wean her off the ventilator.
I was just on a call to another client this morning where she was more or less, her mom, 80-year-old mom after with asthma, ended up in ED in the emergency room about two weeks ago. She ended up being intubated, had a tracheostomy, couldn’t wean off the ventilator, and after about 11 days in ICU and the tracheostomy and the PEG, she’s now in LTAC. The daughter rang this morning saying, “Oh my goodness, this is all terrible. I’ve just seen your videos now. I can already see she won’t be coming off the ventilator. What should we do?” Well, what you should be doing is you should have never gone into LTAC in the first place. That’s why I keep saying, you need to do your research and you need to take responsibilities for outcomes. You are the only person responsible here. No one cares. You need to take responsibility and you need to take matters in your own hands. You need to take responsibility for outcomes and results.
So, to come back to Jim’s question, so yes, this particular client wants her back in the ICU and we can help her with that of course. However, you, Jim, are at crossroads here and if you let her go to LTAC. She will be in the same boat. She won’t get off that ventilator. She will end up either bouncing back to ICU or she will go to subacute from LTAC, which will even be worse.
The healthcare system is broken. Can you see it? Because ICUs are shipping out patients to LTAC and then LTACs ship them out to subacute facilities because LTACs even though you can read on their website, apparently, they can wean patients off the ventilator. I haven’t seen it in reality. Very rarely have I seen it in reality, meaning it’s not the right step for your daughter. You need to keep her in places where she can be weaned off the ventilator and God forbid, if she can’t be weaned off the ventilator, then she can come to Intensive Care at Home.
So, look, I really want to wrap this up today. Unless you have any other questions, I still have a couple of minutes left. Please type them into the chat pad.
Now, if you have a loved one in intensive care and you want to go home, contact us at intensivecareathome.com. Call us on one of the numbers on the top of our website or simply send us an email to [email protected].
If you are an NDIS support coordinator and you’re looking for solutions for your NDIS participants with a ventilator with the tracheostomy, please contact us. We can help you. If you’re wondering how and why the NDIS funds nursing care and situations like that, please contact us. We have been there many, many times and we wouldn’t be in business if the NDIS wasn’t funding nursing care. Same with other providers. Please contact us.
If you have a loved one in intensive care or you are at home on a ventilator, tracheostomy, you don’t have enough support, you’re not happy with your provider, they’re telling you, you can’t have nursing care with intensive care nurses. That’s a whole lot of nonsense. You can because otherwise I wouldn’t be making these videos here. Please contact us as well at intensivecareathome.com. Call us on one of the numbers on the top of our website or email us at [email protected].
If you are a critical care nurse, please contact us if you are after a career change. If you’re looking for new and exciting opportunities, please contact us as well. We have work available in Sydney, Melbourne, Brisbane, including Country Victoria and most likely in New South Wales country as well very soon. So, we’re certainly interested in your applications as well. You can broaden your portfolio of clients with Intensive Care at Home when working for us. You can broaden your horizon in particular. You can see what’s possible outside of intensive care.
If you are an intensive care specialist and you’re looking for work, we are also expanding our medical team at the moment. Please contact us at intensivecareathome.com as well. Intensive Care at Home, we are currently operating all around Australia. We are an NDIS, TAC in Victoria, iCare in new South Wales, NIISQ in Queensland, and DVA approved community service provider. We also have received funding through the Department of Health Child Protection, some public hospitals. So, please contact us if you need help with managing your ICU beds.
If you are an intensive care medical director, nurse manager, bed manager in a hospital, hospital executive, you know where the bottlenecks are, and we can help you with that.
If you need an NDIS nursing assessment, please contact us as well. We provide NDIS nursing assessments. We also provide medical record reviews for patients in intensive care. We can give you a second opinion. We also review medical records after intensive care.
If you need consulting help or advocacy in intensive care, please contact us at intensivecarehotline.com. Again, call us on one of the numbers on the top of our website.
So, if you like this video, if you find value in my videos, give it a like, subscribe to my YouTube channel for regular updates for families in intensive care and Intensive Care at Home, click the like button, click the notification bell, and comment below what you want to see next, or what questions and insights you have.
Please also check out our membership for families in intensive care and Intensive Care at Home at intensivecaresupport.org. There, you have access to me and my team, 24 hours a day, in a membership area and via email and we answer all questions intensive care and Intensive Care at Home related.
Thank you so much for watching.
This is Patrik Hutzel from intensivecareathome.com and I will talk to you in a few days.
Take care for now.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Sunbury, Bendigo, Mornington Peninsula, Bittern, Patterson Lakes, Frankston area, South Gippsland, Drouin, Warragul, Trida, Trafalgar and Moe as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran Affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care at Home, and I’ll see you again next week in another update.