Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies whilst providing quality care and where we also provide tailor made solutions for hospitals and Intensive Care Units to save money and resources and where we provide win-win situations for all of our stakeholders and clients.
So in last week’s blog, I talked about
HOW LONG CAN YOU SURVIVE WITH VENTILATION AND TRACHEOSTOMY?
You can check out last week’s blog by clicking on the link below this video
https://intensivecareathome.com/how-long-can-you-survive-with-ventilation-and-tracheostomy/
In today’s video blog. I want to answer another question from one of our readers and clients. And today’s question is, my mom is 53 and she’s in ICU with sepsis for over three weeks and the ICU doesn’t want to do a tracheostomy.
We Want My Mom at Home and Let Her Approach End of Life at Home. What Should We Do?
So, one of our readers and clients Charlotte writes the following email.
My 53-year old mother got sepsis and had been in ICU for three weeks on a ventilator. She also has leukemia and COPD. The kidneys were failing. And so they did dialysis for the last 10 days. They’ve had her in an induced coma the whole time she’s been in ICU, the liver is failing.
She went into atrial fibrillation, so they had to shock her heart back into a regular sinus rhythm. And now she contracted pneumonia. They can’t get her off the ventilator now because she keeps dropping her oxygen levels.
The ICU said her kidneys have recovered, but they have been requesting for me to sign a DNR or “Do Not Resuscitate” order and they are suggesting that a hospice might be best for my mother because they can’t get her off the ventilator.
They won’t reduce the sedation because when they do, she gets agitated and her heart rate gets up too high. They finally let me see her today and they told me if she recovered, she’d be in a nursing facility for the rest of her life.
They again asked me to put the DNR in place and Friday we are supposed to bring the hospice people in. They don’t want to try the tracheostomy because she’s already had one a couple of years ago and the scar tissue would make it difficult they said.
Last week they had the ventilator support down to 35% oxygen and she was even able to breathe with just BiPAP for two hours but then they put the ventilator back on and it’s working at 80% FiO2 now, and she’s on a PEEP of 15. https://intensivecarehotline.com/questions/my-dad-is-still-vulnerable-and-needs-a-higher-level-of-monitoring-why-did-they-put-him-at-a-spot-far-from-the-nurses-station/
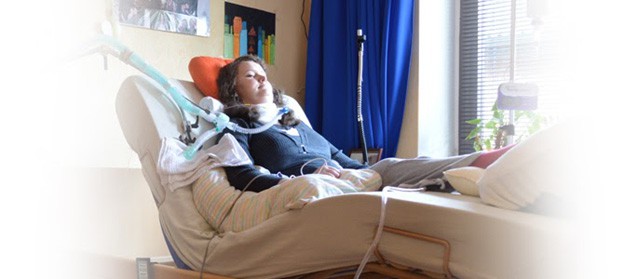
They said she has squeezed hands and eyes on command a lot but when I’ve seen her, she was lifeless.
I asked the ICU if they can get the sedation down enough for me to see her eyes one last time before they want to bring in the hospice and they said no, because of the COVID situation.
I don’t trust the doctors and the nurses, and she never filled out any advanced care directives so I’m having to make all the decisions that I believe by mother deserves a chance and she should have everything done. I believe she should have a tracheostomy and then go home with intensive care at home. So what should we be doing?
From Charlotte
Hi Charlotte,
first of all, thank you so much for writing in and asking your questions. Well, here is what I can see, Charlotte. Your mother is 53 years. She’s very sick. There’s no question about that. And if she’s been in ICU for over three weeks on a ventilator and they can’t wean her off, she should have had a tracheostomy by now. It’s as simple as that.
And especially since she’s been in an induced coma for the whole time, doing a tracheostomy would eliminate the need for an induced coma. So therefore this whole story about the ICU team lowering sedation, and then she wakes up and she can’t breathe could be eliminated and solved by your mother simply having a tracheostomy because the tracheostomy, once again, does eliminate the need for sedation and the induced coma in most cases.
So therefore, waking up would be much smoother for your mother. Now, you were mentioning that your mother has a lot of co-morbidities and she has a long pre-medical history with the liver failing. She’s got atrial fibrillation, she contracted the pneumonia and she keeps desaturating.
Now, those are all significant issues. There is no doubt about that, but again ICU policies or ICU guidelines suggest that a tracheostomy should be done after 10 to 14 days of mechanical ventilation. And therefore the mother should simply have had a tracheostomy by now.
Now that leads me to the DNR and the hospice. Now, first of all, if you, as your mother’s medical power of attorney believes she should have everything done, then you should not be pushed towards a DNR and you’ve done the right thing by not signing anything if this is your mother’s wish.
Now, as you’ve correctly pointed out, if hospice comes in, what the ICU will do is they would probably remove the ventilator and your mother is most likely going to die. And that will be the end of your mother’s life, as opposed to, get a tracheostomy and then potentially send your mother home and let her spend more time at home.
I understand she’s on dialysis, but even dialysis at home is possible with services like intensive care at home. So I also don’t buy, that with your mother having had a tracheostomy in the past and having scar tissue, I don’t buy that since they haven’t tried.
There must be a solution to do a tracheostomy and prolong your mother’s life if that is what you want, especially at such a young age. Also, it goes to show that if your mother had a tracheostomy before, that she’s a fighter and that she can come back from those medical challenges.
I understand the situation at the moment. It’s very difficult because you can’t visit your mother because of the COVID-19 situation and your mother with leukemia in particular would be in a high risk group and would be at high risk of potentially getting COVID-19 in an ICU in particular.
Therefore that’s even a bigger reason for your mother to go home with a service like intensive care at home to be removed from the infection risk. And even if your mother was going to approach her end of life, you wanted to approach her end of life in an environment that you choose and not the ICU.
So, that is what I recommend from here, Charlotte. So I hope that’s enough for you to digest and there is definitely a way forward for your mother to go home with intensive care at home.
So thank you for watching this video blog.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Mornington Peninsula, Frankston area, South Gippsland, as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from intensive care at home, and I’ll see you again next week in another update.







