Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies whilst providing quality care and where we also provide tailor made solutions for hospitals and Intensive Care Units to save money and resources where we provide win-win situations for all of our stakeholders and clients.
So in last week’s blog, I talked about
CAN YOU DISCHARGE A PATIENT HOME FROM ICU DIRECTLY?
You can check out last week’s blog by clicking on the link below this video
https://intensivecareathome.com/can-you-discharge-a-patient-home-from-icu-directly/
In today’s blog, I want to answer a question that we get quite frequently from our clients, but also people who are interested in our service and the question that I want to answer today is
How Long Can You Survive with Ventilation and Tracheostomy?
What a great question because obviously when somebody is having a mechanical ventilation and a breathing tube (endotracheal tube) in ICU, they can’t be weaned off the ventilator then the next step often is to perform a tracheostomy.
And that can lead to several outcomes. It could be a short-term measure to wean patients off the ventilator in ICU but it could also be a long-term treatment plan for somebody to potentially be weaned off the ventilator and the tracheostomy at home.
But it could also be a lifelong treatment option depending on the situation. For example ventilation and tracheostomy could be a lifelong treatment option for patients that have a C1 spinal injury, that have issues such as a motor neuron disease.
Or a tracheostomy could turn into a weaning plan at home for patients with Guillan Barre syndrome.
Or a tracheostomy and mechanical ventilation could become an option for patients for a better quality of end of life at home instead of approaching their end of life in ICU or a hospice. This could be an option for a patient with end stage COPD for example, also after lung transplant where a patient is having a rejection of a donor lung.
Most hospices wouldn’t be able to look after tracheostomy and ventilation anyways, hence intensive home care would be the much preferred option.
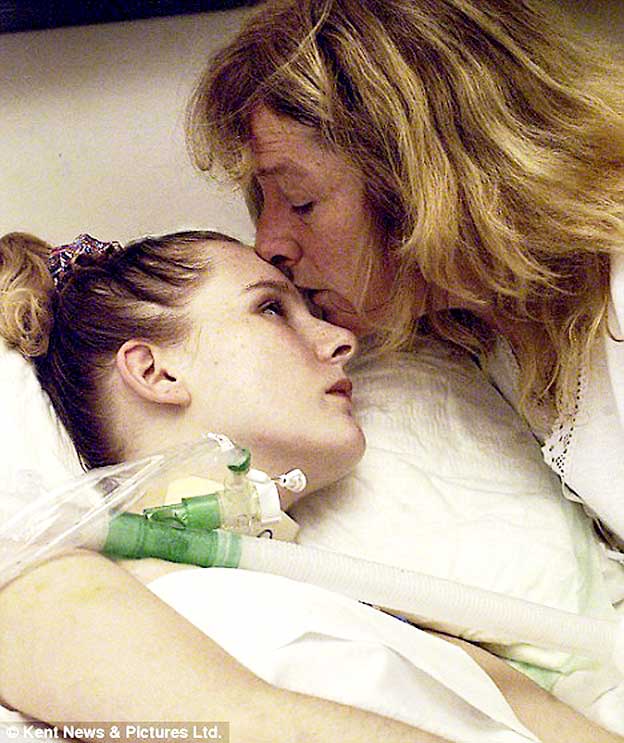
So there could be a number of issues that could lead to lifelong ventilation and tracheostomy. It could also be sometimes an end of life situation where somebody needs ventilation and tracheotomy to prolong their life. Maybe only in the short-term, maybe only for a few weeks or for a few months, maybe they want to spend time at home instead of in intensive care and approach their end of life at home.
But with most of our clients, it’s definitely prolonged ventilation and tracheostomy, and they can live at home sometimes for many years to come and they can actually live a good quality of life in the comfort of their own home with basically having intensive care nurses coming into the home and providing the intensive care at home service 24/7.
This provides a genuine alternative to a long term stay in intensive care.
Again, there are no firm timelines around this. It can be sometimes weeks, months, and it can sometimes be many years. And again, with our clients, many of them report a very good quality of life. They can be at home instead of in intensive care and they can also be enjoying time around their family.
They can be going sometimes to school, they can be doing meaningful activities in their own home with their families. Again, sometimes it’s school university, sometimes it’s even work that they can do from home on the computer. You know, a lot of things are possible in this day and age at home that are not possible in intensive care.
So by going home with intensive care at home, with 24 hour nursing care, we can replicate the ICU just in a much nicer, in a much more family friendly and client friendly environment. And that can go on for many years sometimes.
So, we know of one gentleman in particular, he’s been on a ventilator for almost 35 years now. He sustained a C1 spinal injury when he was a child and to this day he’s still alive and he’s living a very good quality of life, even though he’s on a ventilator and he’s got a tracheostomy.
So, I hope that clarifies your questions. Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section
Intensive care at home Case studies
Also, we are currently hiring intensive care nurses in the Melbourne metropolitan area, as well as in country Victoria in Gippsland. We are hiring intensive care nurses on the Morning peninsula in Victoria, we’re hiring intensive care nurses and pediatric intensive care nurses in Mornington, in Trafalgar, in Warragul. We are also hiring ICU/PICU nurses in Wollongong NSW. You an check out our career section on our website here.
www.intensivecareathome.com/careers
And if you have a loved one in intensive care and you need help, contact us at intensivecareathome.com. Give us a call in one of the numbers on the top of the website, or send me an email to [email protected].
Also, if you are at home already with your loved one, and you don’t have enough support, if your loved one is on a ventilator with a tracheostomy, please give us a call as well. And if you’re looking for funding, give us a call as well. We can help you with all of that.
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from intensive care at home, and I’ll see you again next week in another update.