Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients.
How to Get My Mother Home with Equipment That She Needs, She’s in ICU with Tracheostomy & Dialysis
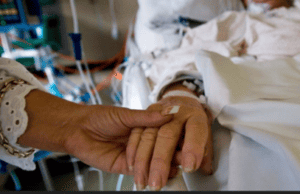
Hello and welcome to another Intensive Care at Home livestream.
Today’s topic is about a question again that we had from a reader and prospective client, and the question today is, “How to get my mother home with equipment that she needs? She’s in ICU with tracheostomy and dialysis.” So, that is the question we are going to address today.
Hi, Tom. Thanks, nice to see you. I hope you’re well and I hope your son is well in particular. Nice to see you.
So, before we go into today’s topic, just a couple of housekeeping issues. If you have questions, please type them into the chat pad and I will address them as we go along. If we have time, I will also give you the option to call in live on the show and ask questions. Depends on how much time we’ve got. We’ll be going for up to an hour. I also want to welcome the viewers that watch this recording in the replay. So, also want to welcome those viewers.
Now, before I go into today’s topic, what makes me qualified to talk about today’s topic? I am a critical care nurse by background, and I have been working in intensive care/critical care for over 20 years in three different countries. I have extensive experience within the Intensive Care at Home space. I was part of first successfully setting up Intensive Care at Home in Germany in the late 1990s, early 2000s before I started my own Intensive Care at Home service here in Australia. So, I know this space right from the start, from the ground off. We were pioneers there and then in Germany, no other country had done this before and now we have launched it on a larger scale here in Australia and we are on the verge of launching it into the U.S. as well.
So then, I have worked in intensive care for over 20 years. I’ve also worked as a nurse unit manager in intensive care for over 5 years and I have been consulting and advocating for families in intensive care for the last 10 years as part of my intensivecarehotline.com consulting and advocacy service for families in intensive care. So, I’m literally talking to people in intensive care or within intensive care at home every day of the week and that is all around the world really.
Now, with Intensive Care at Home at the moment, we are predominantly operating all around Australia. We have clients predominantly on the East Coast, Sydney, Melbourne, Brisbane, but also country Victoria, and also country New South Wales. If you are watching this and you are in Australia, please contact us and we can help you with taking your loved one home from intensive care.
Most of our clients in Australia are getting funding through the NDIS (National Disability Insurance Scheme) but some of our clients also get funding through the TAC, the Transport Accident Commission in Victoria. Also, through the DVA, the Department of Veteran Affairs, iCare in New South Wales, as well as NIISQ (National Injury Insurance Scheme in Queensland), as well as funding from hospitals directly.
Bear in mind when we take someone home from intensive care, it’s a win-win situation. We are cutting the cost of an intensive care bed by approximately 50%. We are freeing up an in-demand ICU bed and most importantly, we are providing quality of life and in some instances, quality of end-of-life for patients and families in intensive care. So, it’s a win-win situation all around.
So, that’s a little bit about me to set the scene, what we’re talking about today. Once we’ve answered our reader’s question, we will also answer other questions that came in during the week.
I do these YouTube live streams, usually once a week on a Sunday morning, 10:30 AM Sydney, Melbourne Time, which is 8:30 PM Eastern Standard Time in the U.S., 7:30 PM Central Time, 6:30 PM Mountain Time, and 5:30 PM Pacific Time. Those are on a Saturday in the U.S. or in North America. For our U.K. audience, at the moment it is just about 1:30 AM so you’re probably watching this on the replay and not on the livestream. But for anyone who has inquiries or questions in the meantime, please go to intensivecareathome.com and contact us there if you have questions or if you need help.
If you are an NDIS support coordinator or NDIS specialist support coordinator in Australia and you are looking for specialist home care services, please contact us as well. Especially, if you don’t know how to get funding for NDIS participants, please contact us.
So, let’s get onto the question today, “How to get my mother home with equipment that she needs? She’s in ICU with tracheostomy and dialysis.” So, obviously Sarah, this comes from Sarah. Sarah, you’re encountering a stumbling block here with your mother, how to go home with care needs that more or less hold your mother hostage to intensive care? So, anyone going home with a tracheostomy needs 24-hour nursing care with tracheostomy competent nurses.
Now, nurses that are tracheostomy competent are generally speaking, CCRNs, critical care registered nurses, that have worked in ICU, pediatric ICU, or sometimes ED (Emergency Departments) for prolonged periods of time. We usually only hire them if they have a minimum of two years ICU, pediatric ICU, or emergency department experience, ideally a combination of all of it, and who ideally have completed a postgraduate critical care qualification. That pretty much sums up the qualifications and the skills of our workforce that we have employed at Intensive Care at Home.
Now, if someone has dialysis needs on top of that, yes, they would be confined to the four walls of an ICU because in ICU, again, the current perception or the current paradigm that most ICUs still operate in is that there’s two options for ICU patients. One option is to get better and leave intensive care alive or the second option is to die, to pass away. The first option is if they get better to leave to hospital floor or to a hospital ward or in the U.S., sometimes they go to LTAC (Long-Term Acute Care), whereas we have a third real option where patients can go home.
Now, Sarah, what you’re also saying in your email here is that you haven’t even considered care at home, you were just looking for the equipment. So, your question is probably incomplete, and your question comes with knowing what you don’t know and not knowing what you don’t know. You don’t know what you don’t know. You don’t know what to look for, you don’t know what questions to ask, and you certainly don’t know your rights, and you certainly don’t know how to manage the intensive care team there because your question should be around, “How to get my mother home with equipment and nursing care that she needs. She’s in ICU with tracheostomy and dialysis.”
Now, you haven’t said that your mother is ventilated as well. There’s a high chance she is ventilated, but you haven’t mentioned that. But let’s just base your question on the assumption your mom has a tracheostomy and needs dialysis. Well, getting the equipment is not as difficult as you think it is. We are setting up ICU beds at home all the time and we’re setting up the equipment so that it’s safe and a home care and not getting readmitted to hospital is predictable.
Our promise really is to keep our clients at home predictably, and it’s very important that we keep them home predictably. Imagine we would be providing Intensive Care at Home services and it’s not predictable. So that would be a disaster, really.
Why would it not be predictable? We couldn’t promise Intensive Care at Home if our clients would go back to ICU all the time. So, chances are, Sarah, that if your mom goes home just with equipment and not the appropriate nursing care, it’ll fall apart. Case in point. So, when you look on our website at intensivecareathome.com, there’s a section on our website, mechanical home ventilation guidelines.
So, with the mechanical home ventilation guidelines it’s evidence-based, it’s research-based, and it’s a result of the last 25 years of Intensive Care at Home services in Germany in particular. Obviously, the space has been researched enough and enough evidence has been gathered that anyone at home on mechanical ventilation, tracheostomy, non-invasive ventilation, even for clients that “only have a tracheostomy without ventilation.” They need 24-hour nursing care with critical care trained nurses with a minimum of two years critical care nursing experience, everything else is unsafe.
So, by you, Sarah, thinking you can take your mother home once she has the right equipment is a disaster waiting to happen. Not only is that a result from an evidence-based research paper, it’s also a result of unfortunately some very tragic real-life experience. So, let me give you an example.
We’ve had some clients where we looked after them at home with a tracheostomy. One client was with a tracheostomy, a child, who did not have 24-hour nursing care, was only funding for night shifts for critical care registered nurses. During the day, the parents or laypeople, i.e., disability support workers or nursing aides were looking after this child. Just as we predicted at the time, the child passed away during the daytime when a critical care nurse was not funded, and the child died from a medical emergency that could not be managed by either parents or a support worker. Not even a general registered nurse without critical care nursing experience can safely manage a tracheostomy, let alone a family member or a support worker. That’s one example but there are countless other examples.
There was another client, very similar, that we looked after and there was only funding for night shift. During the day, a ventilated and tracheostomy child was looked after by family and by a mixture of support workers or a general registered nurses. Again, the child passed away during the day when we were not there, just as we predicted. Unfortunately, that was a drastic or a very dramatic outcome which resulted in the death of a child, two children, and they were both inadequately NDIS-funded. The NDIS is now busy trying to sweep this under the carpet.
Mr. Bill Shorten, I urge you to look at those cases. You know who they are. I’ve emailed you the names of the cases and I urge you to look into this failure of the system, into the negligence from the NDIS by not funding the appropriate nursing care for these children. They resulted in the deaths of children. So, Mr. Bill Shorten, I urge you not to sweep this under the carpet because I will keep talking about it publicly until the issue has been resolved and the appropriate funding is made available for clients in similar situations.
Coming back, Sarah, to your question. So, what needs to happen in your situation is really to get the equipment but also get the nursing care, which is 24-hours with a tracheostomy, potentially ventilation and dialysis. So, I presume your mom might have the vascular catheter for dialysis or she might have a fistula in her arm. I don’t know, you haven’t shared that. But either way, we can do all of that at home for your mother.
Funding, you might want to know how to go about funding. It really depends. I presume you are in Australia. Again, if your mom is less than 65 years of age, she will get NDIS-funding. If your mom is above 65 years of age, I don’t know whether what led to your mom’s situation, is she compensable? For example, did she have, God forbid, a car accident? Did she have any other sort of accident where there’s some form of compensation? Let’s just assume there is no compensation, then we should get this in front of the Department of Health or in front of private health insurance. Or if you are in the U.S, then we should get that in front of your insurance.
Again, it’s a win-win situation. The insurances will pay for an ICU bed, five to $6,000 per bed day anyway. We might as well make the proposal for Intensive Care at Home where you pay or where the insurance only pays half of the cost. So, no matter who is paying for it, the taxpayer will be much better off by paying only half of the cost of an intensive care bed. Plus, the general public has another benefit by having another intensive care bed available. The hospitals have a benefit from it by having an intensive care bed available.
There are also industry intricacies I want to call them. If you have a long-term patient in intensive care, it’s sort of the intensive care team is getting tired of looking after them. I’ve walked in those shoes of course, where you’re coming to a shift and then you’re going into bed nine or whatever. Mr. Smith who’s been there for three months, and if you’re allocated there, people go, “Oh, not again. I’ve looked after Mr. Smith already enough times, and I don’t want to look after him anymore.” We are not in those shoes because we want to look after those patients, and we want to improve their quality of life at home. So, for us, this is very exciting if we can look after your mother at home or after anyone at home because we are not jaded by looking after someone long-term because that’s our specialty, that’s our area of expertise to look after patients long-term.
So, please keep that in mind that whether it’s from a hospital perspective or from a family perspective, we want to look after these patients. We are the experts of looking after these patients. We have been doing this for the last 10 years now. We know exactly what to do. We also know how to negotiate with funding bodies, how to get or how to obtain funding for home care instead of hospital care. We also know how to set up the home, what equipment is needed, where to get equipment from, where to get the ventilators from, where to get the tracheostomies from, how to set up for emergency equipment, how to set up the rooms, what else needs to happen in someone’s home if, assuming a patient is immobile, how to organize a ceiling hoist or a lifting machine, hospital bed and the list goes on. So, I hope that answers your question, Sarah.
Also, we know how to make a discharge from ICU seamless so that your mother can go home seamless and safely, more importantly, so that she doesn’t bounce back to hospital pretty quickly. We also know who to organize for home care such as Allied Health professionals such as occupational therapists, physical therapy, physiotherapy, speech therapy, dialysis nurses and so forth. So, we know all of that, how to organize that. So, please contact us with what needs to happen next.
As I said, because you are asking for equipment only, it’ll burn you out pretty quickly, you and the rest of your family looking after your mom. (A), it’ll burn you out. (B), it’s not sustainable. (C), it’ll be life-threatening for your mom. Looking after a tracheostomy ventilation, dialysis takes years of training and practice, therefore, you’d be putting yourself into a compromising situation.
Whilst we also know it can be very stressful for families to have a team of ICU nurses coming into their home. It can be very daunting. You can trust that we can find you the right team, can find you the right nurses. It’s very important for us that we have the right nurses for the right clients. We know that this can be very daunting for clients, but your alternative is to stay in ICU where you have a different nurse every day anyway. Those nurses, generally speaking, are probably nowhere near as motivated as our nurses who have signed up to keep our clients at home predictably. So, keep that in mind, Sarah, as well. So, I hope that answers your question.
I also want to then move on to other questions that have come in this week. Just give me one second. I just quickly need to look at my emails so that we can go through those questions. The first question that came in this week came from Veronica, and Veronica writes, and she says, “My mom is in intensive care and unresponsive after she fell and hit her head. How long will she stay like that?” Wow. I’m very sorry to hear that, Veronica. Here is what to expect in a situation like that.
So, if she hit her head, it really depends on what happened after she hit her head. Does she have a concussion? Does she have a brain bleed? Does she have a skull fracture? Does she have a bleed that’s leading to a midline shift in the brain? Is she on ICP (Intracranial pressure) monitoring? Does she have an intracranial brain monitor? If she does have that, what are her brain pressures like? Are her brain pressures increased to the point where she needs close ICP intracranial pressure therapy and treatment? Because if her brain pressure is too high, she is at risk of irreversible brain damage because of oxygen starvation to the brain.
Another question is, did she have surgery on the brain or are they just managing it with an ICP monitor? Are they just managing it with an EVD (External ventricular drain), for example, to drain CSF (Cerebrospinal fluid) and to drain potentially blood from the brain? So, that’s some questions there. Other questions are, is she in an induced coma? Is she ventilated? Does she have a breathing tube? Does she have a tracheostomy? How long has she been in this situation?
So, let’s just assume the worst-case scenario here. She’s had a hemorrhage, she’s got ICP monitoring, she has internal brain bleeding. Her ICPs are high, so that means she would need to get treatment for that, i.e., she might need another evacuation of a bleed in the brain. She will need constant ICP monitoring until ICPs are stable.
She’s probably in an induced coma with strong sedatives and strong opioids such as midazolam, propofol, potentially phenobarbital. She might need fluid drainage from the brain by either using an EVD drain, but also by other therapies such as mannitol, hypotonic saline to minimize the brain pressure in the brain. Sometimes patients are even paralyzed in those situations because no amount of sedation will get the high pressures down in the brain and therefore sometimes patients are even paralyzed in situations like that.
So, therefore, there can be a prolonged induced coma, Veronica, and if there’s a prolonged induced coma, if you’ve watched any of my other videos, you would’ve found that with a prolonged induced coma, there goes deconditioning hand in hand, muscle wastage, and then when patients wake up or are ready to be woken up, assuming that the brain pressures will be controlled eventually, there can be confusion, there can be apathy, there can be not waking up for prolonged periods of times. So therefore, you will need to be very patient here or potentially will need to be patient if things are not progressing as quickly as you would like to see.
If your mom is waking up, there’s no guarantee she will be waking up and she has a good memory and she remembers everything that’s happened, or she can sort of tack into the life that she was living before the accident. It’s hard to say what’s happening and it’s hard to predict the outcome in a situation like that.
But you are asking how long will she stay like that? That’s a question that is difficult to answer. But what I can tell you is when we work with clients one-to-one with our consulting and advocacy service, once we talk to the doctors and nurses directly, when we look at medical records, then we can handhold you through the process step-by-step. We can almost predict to you what’s happening next. Whereas ICUs are always guarded in what they’re telling you because they also always want to stay in control of the narrative. Whereas we are probably more objective, and we can tell you why they’re not telling you what’s going to happen, and we can walk you through it step-by-step and really handhold you through the process. So, I hope that helps, Veronica, and answers your questions.
I really encourage you to reach out to us so that we can talk to the doctors and nurses directly and look at medical records because you will need a second opinion in a situation like that, so that the intensive care team will not cloud your own judgement of the situation.
Now, next question from Chad who says, “My loved one went to ER after a tonic-clonic seizure and another tonic-clonic seizure in the ambulance. In the doctor’s notes, from less than an hour and a half in the ER, he had recognized status epilepticus, but she never got even an EEG until 36 hours later and 10 hours later intubated. Is this the reason she’s still in a vegetative state and has not been able to breathe three weeks later?” Wow.
Okay, so let’s read this again, “My loved one went to ER after tonic-clonic seizure and another tonic-clonic seizure in the ambulance. In the doctor’s notes, from less than an hour and a half later in the ER, he had recognized status epilepticus, but she never got even an EEG until 36 hours later and then she got intubated 10 hours later. Is this the reason my loved one is still in a vegetative state and has not been able to breathe three weeks later?” Well, this is actually almost tying right in with our previous question from Veronica.
So, if your loved one had a status epilepticus without the doctors even doing an EEG (Electroencephalogram), well, it really comes down to making that judgement in real-time when someone has a status epilepticus, because it’s easy to work out when someone has a status epilepticus as with their tremors, shivering, shaking, rolling eyes, and unconsciousness. So, it doesn’t really need an EEG to make that judgement whether someone has a status epilepticus or not. An EEG is something that can be followed up on.
Probably more importantly in a situation like that is CT scan of the brain, MRI scan of the brain. Yes, EEG might be important and could be monitored for a few days to see whether there are other seizures happening, major seizures, minor seizures. Sometimes minor seizures can happen as well and no one will detect it, but the only way it can be detected is actually through an EEG. So, it’s not a bad idea to hook up an EEG in those situations if you can, but you are now telling me that this is three weeks later and she’s still in a vegetative state and she has not been able to breathe three weeks later.
Now, so the first question here is why is she still in a vegetative state? Is it because of her brain or is it because she was in a prolonged induced coma? Was she potentially chemically paralyses? That’s one question. The other question is what does her CT scan of the brain show? What does her MRI scan of the brain show? What does an EEG show potentially? Again, what sedatives has she been on and for how long? What opioids has she been on and for how long? Are kidneys and liver working or is there some form of impairment that potentially delays waking up because sedatives and opioids cannot be metabolized or excreted through kidney and liver?
Next, with status epilepticus or any seizures, your loved one is most likely on anti-epileptic drugs such as Keppra, phenytoin/Dilantin, Vimpat, sodium valproate, or other antiepileptic drugs. So, if that’s the case, is that contributing to her not being able to breathe and not being able to wake up? I.e., she’s still in a vegetative state.
Next, if she’s not being able to breathe, why is that? What was your loved one’s premedical history, if any? Is there a premedical history that potentially contributes to this situation? I would assume that after three weeks in ICU she would be having a tracheostomy. What are they doing? Have they tried to wean her off the ventilator? If so, why is it not working? Or is her vegetative state at a point where she’s not even breathing? What’s her Glasgow Coma Scale like?
Please have a look on our website and look for Glasgow Coma Scale, type into the chat pad Glasgow Coma Scale, also known as GCS. It’s a neurological assessment tool to assess how awake your loved one is and what their neurological status is. That’s a very important assessment tool that you should familiarize yourself with. It may well be the reason why a loved one is not being able to breathe in three weeks, but there could be other contributing factors again. But that’s what I would be looking for.
Look at what sedative she’s been on and for how long. Are kidneys and liver working? What’s MRI and CT scan of the brain showing? How significant is the brain damage from the seizures? Has there been irreversible brain damage, for example? Those are the type of questions you should be looking for.
But once again, the quickest way to deal with this situation is for me to talk to the doctors directly or to look at medical records. Ideally do a combination of both. Please chat, reach out to us to get those questions answered.
So, the next question comes from Jerry. Jerry says, “I was in an induced coma for three weeks and have no memory of it. I have no memory of anything for weeks prior to ending up in the hospital. Though I came to in intensive care and talked to people, I have no memory of any of it. My first memory is waking up in the regular hospital not knowing where I was, how I got there or why I was there.” Well Jerry, thank you so much for sharing that with us and with our viewers. We have many families at Intensive Care Hotline reach out to us and ask whether people can hear them in their induced coma.
They ask questions such as, “Should I talk to my mom and my dad? Should I talk to my spouse? Should I talk to my child? Should I talk to my brother and sister?” Well, my advice is always yes, because you just don’t know. Now, just because Jerry says she can’t remember, doesn’t mean that others can remember or can’t remember. We have other emails coming in where people say, “Well, I can remember every little thing even though I was unconscious. I remember my mom, my dad, my brother, my sister talking to me.” So, it’s not a one-size-fits-all. I would’ve read out other emails on this in a livestream where people would’ve said, “Well, I remember everything in ICU.” It’s not a one-size-fits-all, but let’s read this out again so just for everyone to understand what it looked like for Jerry when she was in an induced coma.
So, Jerry writes, “I was in an induced coma for three weeks and I have no memory of it. I have no memory of anything for weeks prior to ending up in the hospital. Though I came to in intensive care and talk to people, I have no memory of any of it. My first memory is waking up in the regular hospital not knowing where I was, how I got there or why I was there.” It’s not dissimilar to my experience when I worked in ICU for over 20 years in three different countries that in ICU, when people wake up after an induced coma, they can be confused, they can be agitated, they can be aggressive sometimes, they can be very pleasantly confused, they can even be funny, but it’s not a one-size-fits-all.
But the good news is here again for anyone wondering, “Oh, why is the intensive care team so negative?” Well, you can hear from Jerry, she made it through and so will others. So, most ICU patients will make it through. So, it’s also a good testimonial from Jerry that people survive intensive care and they’re able to go back to a normal life. And she was in an induced coma for three weeks, keep that in mind. Three weeks.
So, let’s move along to the next question. Next question is from Daniella and Daniella is in the U.S. Daniella writes a lengthy email, and she says,
“Hi, Patrik. My brother is in ICU and has been in ICU for one month at Kaiser in Sacramento in the U.S. following a heart attack. The ambulance arrived 20 minutes while someone administered CPR. The doctor deemed him brain dead, 92% with prognosis of maybe waking up but remaining a “vegetable”.” And I put vegetable in quotes. I think that’s a terrible term”
“Not knowing who is around him and asks us to make a decision. If he wakes up, he will need open heart surgery. Two weeks later my brother opens his eyes at the sound of our voices sometimes or when he’s shaved, yawns, flexes his muscles, arms, legs, more the right than the left, as if he would like to push or do something or get up? But that’s about it.
We ask for more time and for a second MRI and/or EEG to see what percentage of new connections were made or just see differences between the two to see what progress, if any. We were refused categorically because they deemed him brain dead and for them to do another MRI, he has to sit on the side of the bed and show the peace sign when asked.
At our request, they did a tracheostomy and feeding tube and transferred him into a regular salon in the hospital telling us that they will discharge him either to a nursing home or our home. Nursing home will only keep him for three weeks.
We need guidance on what we can do at this point and take informed decisions. The patient, my brother, is on medical and money is scarce. We are not equipped to care for him at home. I live out of town. My mom is 92 with four stents following two heart attacks. Other siblings could not care for him 24/7.
I wanted to get a second opinion. However, every time I call, I’m being asked to provide either $7,500 or a referral from a doctor or a different insurance. Can you guide us?”
Thank you so much, Daniella, for writing and I’m very sorry to hear about your brother’s situation. That sounds terrible. Now let’s break this down. Let’s break this down, Daniella. Your brother is definitely not brain dead. It’s very frustrating for me that so many families are being misled by ICU teams when it comes to someone being brain dead or brain damage because there’s a big difference between the two and there’s no correlation between the two.
If your brother was brain dead, he would not respond to anything. He wouldn’t breathe, he wouldn’t respond, he would show no reflexes, whatsoever. Now, by you telling me that, “He’s moved, your brother opens his eyes at the sound of our voices, and sometimes when he’s shaved, he yawns. He flexes his muscles, arms, legs, more to the right than to the left as he would like to push or something to get up?” So, that’s a very good sign. So, that means he’s definitely not brain dead.
For someone to be considered brain dead, there’s also two independent doctors need to do testing for brain dead and there’s a series of tests they need to go through. So, it doesn’t sound to me like this has been done at all otherwise they would’ve probably told you that.
So, in a situation like that, you cannot just take the doctor’s word for gospel. As I said, I do believe the term brain dead is often being misused in ICU and it can be scientifically verified by doing some brain death testing. That has not happened here.
Again, families in intensive care don’t know what they don’t know and that’s their biggest challenge. They don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care.
Now, before I want to break this down, I also want to quickly read out the category for brain death, the criteria. So, here is the criteria according to the NHS, “There are a number of criteria for diagnosing brain death. For a diagnosis of brain death, a person must be unconscious and fail to respond to outside stimulation.” Fail to respond to outside stimulation. Your brother has already responded to outside stimulation. Now, we could stop here, but I want to clarify this here.
“A person’s heartbeat and breathing can only be maintained using a ventilator.” Now that may or may not be the case for your brother, but even if that is the case, he’s not failing to respond to outside stimulation. He is responding to outside stimulation.
Then next, “there must be clear evidence that serious brain damage has occurred, and it cannot be cured.” That may be the case for your brother, but because he’s responding, there may be a cure that he may wake up.
Now it also says, “Ruling out other conditions. Before testing for brain death can begin, doctors must carry out a series of checks to ensure that the symptoms are not being caused by other factors such as an overdose of illegal drugs, tranquilizers, poisons or other chemical agents.” So, your brother might not have taken illegal drugs, but he might have been on heavy sedation or opioids that still keeps him sedated.
So, I just wanted to clarify that you need to be clear of the terminology and you need to be clear that intensive care teams are often trying to create a negative narrative from the start so that it’s easier for them to “sell you” on an end-of-life situation. And they’re often using the term brain death and mislead families. I’ve seen it over and over again. Your brother is definitely not brain death. So, don’t get swayed by incorrect terminology here and do your own research, which is what you’re doing now anyway.
So, waking up in intensive care sometimes can take weeks, days, sometimes months. So, it’s also like the doctors are saying of him maybe waking up but remaining a vegetable, which I think is a terrible term. We are human beings, not vegetables. It’s terrible that a term like that is even being used. Another much better term for that is your brother may well be in a vegetative state, but vegetative state is different compared to someone labeling a human being as a vegetable. That’s terrible.
So obviously, they asked you to make a decision. You’ve made the decision of a tracheostomy, which I believe is a wise thing for you to do. By you, being patient, you’ve obviously noticed your brother has opened his eyes, that is really good. You ask for more time, which is very wise. You ask for a second MRI or an EEG to see what percentage of new connections were made or just see differences between the two to see what progress has been made. But you have already seen progress here, Daniella, by seeing that your brother is waking up.
Now, you are also saying, “We were refused categorically because they deemed him brain dead and for them to do another MRI, he has to sit on the side of the bed.” Now, I call nonsense on that. No one has to sit at the side of a bed for an MRI. An MRI can be done without sitting at the side of a bed. As a matter of fact, many patients in intensive care have an MRI and they’re definitely not sitting on the edge of the bed. They’re actually lying flat. So again, they’re clearly misleading you here and I don’t know why.
Again, it probably all comes down to their agenda. By them refusing an EEG, they’re basically saying your brother won’t improve. But like you said, you want to see whether the brain has made any new connections. You want to get a follow up EEG and a follow up MRI and find out what’s exactly happened.
Get a new report and see whether there has been any improvement because physically, there has been improvement clearly from what you are actually observing. Your brother’s waking up, he’s showing signs of life, and now he’s got a tracheostomy, which means he can come off sedation, which should help him by waking up, which should help you and the doctors there and the ICU team to make an accurate assessment of his current neurological status and then make the next steps from there.
Probably, he needs to go into neurology rehab and if he can’t be weaned off the ventilator or if he remains with the tracheostomy, then he can go home with intensive care at home once again.
“And he’s also got a feeding tube now. Hospital telling us that they will discharge him either to a nursing home or a home. We need guidance on what we can do. We are not equipped to care for him at home.” No, and you’re not, just like in our original question, “Can my mother go home with equipment, with the tracheostomy and dialysis?” Yes, she can go home similar to your brother.
Your brother can go home with a tracheostomy, with the ventilator, with the feeding tube, even with brain damage because with intensive care nurses, 24 hours a day, that’s all doable. A home care environment is probably so much more conducive than a sterile ICU and hospital environment.
Now, once again, from a funding perspective, a hospital bed costs a lot of money and Intensive Care at Home costs half of that. So, you will have a really good argument to make for your brother to go home and not pay for it because the insurance will have an interest in paying for it because they’re saving money. So, I hope that helps, Daniella, to shed light on your situation.
But I can’t reiterate that often enough for any family in intensive care, do not get confused between the terms brain death and brain damage. There is no correlation between the two, whatsoever. Please also keep in mind when ICUs talk about brain death, once you know that is potentially being determined, the next conversation they’re wanting to have with you is whether you want to donate the organs of your loved one. That’s often where this is leading towards, whether you want to donate the healthy organs of your loved one. So, keep all of that in mind.
ICU is sort of the Pandora’s box for any family that doesn’t know enough about it. It’s a minefield if you don’t know what to look for, if you don’t know how to interpret information, they’re throwing at you. If you don’t know what it all means, you need to be educated, you need to do your research from day one. You can’t start early enough.
It’s not only when you first go into intensive care knowing what can happen, knowing what to look for, knowing what to ask for, knowing how to negotiate with intensive care team. You don’t even know that this is necessary. You will need to negotiate with the intensive care team all the time, but you need to know what to negotiate for because you need to be able to recognize the patterns. You need to be able to predict what they’re going to do next.
That’s where we can help you with here with Intensive Care Hotline and also then with Intensive Care at Home if you are interested in going home. I think in your situation, Daniella, I think this is inevitable that you are going home in a situation like that.
Then last question before we wrap this up today, from Roma, “Hi, Patrik. My mother is in a coma since the 20th of February 2023. The doctor has removed a tracheostomy seven days ago, but she’s still unconscious. She opens her eyes occasionally, doesn’t respond on verbal command. What should we do?” Now, okay, Roma, what you should be doing in a situation like that, I do believe your mom will need some neurological rehabilitation. You should also ask whether all sedation has really been removed, including maybe they’re giving her medications to sleep at night, similar to other questions that I answered before. Is she potentially in kidney failure, liver failure? Has all sedation not been cleared? But in a situation like that, you may want to look at neurological rehabilitation.
Now, it’s interesting to me, you are saying they have removed a tracheostomy seven days ago, but she’s still unconscious. That’s a little bit of a surprise to me because if someone is unconscious, there is the risk of aspiration, there is the risk of them not being able to swallow. Therefore, I see it as a risk of having the tracheostomy removed. Have they potentially set up your mom for an aspiration pneumonia and then she’s going to die from that? Let’s just assume your mom is able to swallow, but she doesn’t respond to verbal commands. She probably needs to go onto neurological rehabilitation.
Now, you haven’t shared why is she in a coma? Is it a natural coma? Is it a coma induced from a brain injury, anoxic brain injury, traumatic brain injury? Is it a coma that’s still kind of a “hangover” situation from opioids and sedation? That would be my question here.
So, many unknowns, but neurological rehab, check with them that she’s not aspirating. Check with them that she’s able to swallow and breathe, maintain her airway, that she’s able to cough. If she’s unconscious, is she able to cough? If she’s not able to cough, if she’s not able to swallow, she needs the tracheostomy back in most likely. So, just some thoughts there. So, I hope that helps, Roma.
Now, let’s wrap this up today.
If you have any other questions, please type them into the chat pad. As I said, I am doing these YouTube lives every Sunday morning, 10:30 AM Sydney Melbourne time, which is Saturday evening, 8:30 PM Eastern Standard Time in North America, 5:30 PM Pacific Time.
So, let’s wrap this up. Still got time for another question if you want to type into the chat pad. If not, like I said, with Intensive Care at Home, anything is possible at home really for long-term ventilation, tracheostomy, but also non-invasive ventilation, BIPAP (bilevel positive airway pressure), CPAP (continuous positive airway pressure), medically complex patients, seizure management, but we’re also looking after tracheostomy patients at home that don’t need ventilation, but still need the intensive care nurse 24-hours a day because otherwise it’s not safe. As I mentioned to you, go and have a look at our mechanical home ventilation guidelines on our website.
If you are an NDIS support coordinator, please contact us as well. For our clients, if you’re a good NDIS support coordinator, in particular if you know all about funding for registered nurses through the NDIS, please contact us. We can help you with the advocacy. We do nursing reports for the NDIS nursing assessments, but we also know a lot about the advocacy with the NDIS. Also with other funding bodies, we know a lot about the advocacy.
Next, if you are at home already and you have insufficient support, please contact us as well. You might have support workers at home and you’re going back to ICU all the time, or you might balance back to hospital all the time, please contact us. We can help you keeping you at home predictably again, especially around the conditions that I mentioned, ventilation, tracheostomy, BIPAP, CPAP, tracheostomy without ventilation, home TPN (Total Parenteral Nutrition), IV infusions at home including potassium infusion, palliative care. Please contact us as well.
As I said, we are operating all around Australia at the moment and we are in the process of opening up a branch in the U.S., probably in Texas. Stay tuned.
Also, if you are a critically care nurse and you’re looking for a career change, please contact us at intensivecareathome.com. We are currently having exciting opportunities for critically care nurses in Sydney, Melbourne, Brisbane, and including country Victoria. If you are an intensive care consultant, ICU specialist, we are currently trying to expand our team of ICU consultants to take our service to the next level, please contact us as well.
Now, if you are having a loved one in intensive care and you need consulting and advocacy, please go to intensivecarehotline.com and call us on one of the numbers on the top of our website or simply send us an email to [email protected].
If you want intensive care at home, again, contact us at intensivecareathome.com. Call us on one of the numbers on the top of our website or send us an email to support, sorry to [email protected].
Now also, have a look at our membership for families in intensive care and Intensive Care at Home. There, you have access to me and my team, 24 hours a day, in the membership area and via email and we answer all questions intensive care and Intensive Care at Home related.
If you need a medical record review, please contact us as well. We review medical records in real-time, give you a second opinion in real-time. We also review medical records after intensive care, especially if you have unanswered questions, if you need closure, or if you’re looking for medical negligence.
Again, we are also providing nursing assessments for our clients and for the NDIS as well, including NDIS support coordinators.
Now, subscribe to my YouTube channel for regular updates for families in intensive care and Intensive Care at Home, share the video with your friends and families. I would love to see you again next week in the next YouTube Live next Sunday, 10:30 AM Sydney Melbourne time, or 8:30 PM Eastern Standard Time in the U.S. on the Saturday, 5:30 PM Pacific Time, in the U.S. on the Saturday. Like the video, click the notification bell, and comment below what you want to see next, or what questions and insights you have from this video.
Thank you so much for watching.
This is Patrik Hutzel from Intensive Care at Home and intensivecarehotline.com and I’ll talk to you in a few days.
Take care.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Sunbury, Bendigo, Mornington Peninsula, Bittern, Patterson Lakes, Frankston area, South Gippsland, Drouin, Warragul, Trida, Trafalgar and Moe as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran Affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care at Home, and I’ll see you again next week in another update.







