Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies by improving their Quality of life and where we also provide tailor made solutions to hospitals and Intensive Care Units to save money and resources, whilst providing Quality Care!
In the last blog I talked about
Home mechanical ventilation quality standards!
You can check out last week’s blog here.
In this week’s blog I want to answer a question that we get quite frequently from our readers and also clients
Can you be discharged home from hospital with ventilator, tracheostomy and feeding tube?
Many families in intensive care have loved ones in ICU/PICU with long-term ventilation and tracheostomy requirements.
Their loved ones usually experience either difficulties, delays or complete failure in weaning off the ventilator and tracheostomy.
What are the reasons for mechanical ventilation and tracheostomy?
Causes of admission to ICU/PICU for mechanical ventilation and tracheostomy are: acute respiratory failure with underlying chronic co-morbidities 176 (24.4%); exacerbation of Chronic Obstructive Pulmonary Disease 222 (34.4%); neuromuscular diseases 200 (27.8%) (i.e. Guillan Barre syndrome, Motor neuron disease or MND); surgical patients 77 (10.7%); thoracic dysmorphism 28 (3.8%); obstructive sleep apnea syndrome 16 (2.2%). Percutaneous tracheostomies were 65.9%. Major complications after tracheostomy were 2%. 427 tracheostomies were evaluated for decannulation: 96 (22.5%) were closed; 175 patients (41%) were discharged with home mechanical ventilation; 114 patients (26.5%) maintained the tracheostomy despite weaning from mechanical ventilation and 42 patients (10%) died or lost.
Reference: https://www.ncbi.nlm.nih.gov/pubmed/20122822 Tracheostomy in patients with long-term mechanical ventilation: a survey.
Further to this reference above, what leads to prolonged mechanical ventilation, tracheostomy and then the ability to wean a critically ill Patient off the ventilator eventually are the inability to wean somebody off the ventilator.
This often begins with prolonged induced coma, intubation (insertion of the breathing tube), breathing tube/endotracheal tube and the failure to extubate (removal and the breathing tube).
Generally speaking intubation for respiratory failure leads to induced coma, mechanical ventilation and this also goes hand in hand with a nasogastric tube (NG tube) for feeding.
Again, if weaning off the ventilator and the breathing tube (extubation) can’t be achieved, the next step is to perform a tracheostomy!
When is the right time to perform a tracheostomy?
Here are some articles and videos for you to answer that question
When a tracheostomy is done, a PEG tube or feeding tube also known as gastrostomy is done as well.
A PEG is a permanent feeding tube through the abdominal wall into the stomach.
Nevertheless it is often doctors and family preference whether a PEG tube is inserted or a nasogastric feeding tube is left in place to continue feeding.
Anybody on a ventilator with either a breathing tube or tracheostomy is unable to eat orally, hence the nasogastric feeding tube or the PEG feeding tube.
In either case with a tracheostomy, mechanical ventilation and feeding tube a patient can definitely be discharged home with a service like intensive care at home.
Mechanical ventilation, tracheostomy and feeding tube is definitely not an obstacle for intensive home care.
Ideally, patients are medically and hemodynamically stable before going home and they should ideally be off intravenous inotropes and vasopressors.
However, low doses of inotropes or vasopressors are not a hindrance for intensive home care, because intensive care at home provides an intensive care substitution service in the home.
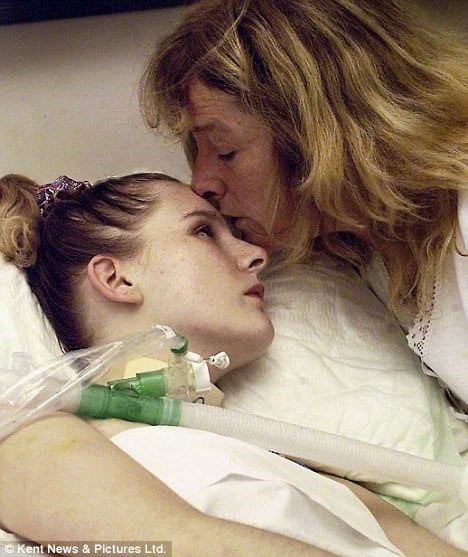
Multiple care and treatment options are available at home for long-term ventilated patients with tracheostomy and feeding tubes.
This also includes ventilation and tracheostomy weaning at home. Especially when it comes to prolonged weaning in intensive care, ventilation and tracheostomy is much better at home because it’s being done in a more holistic and therefore patient and family friendly environment!
How much nicer is it being at home compared to a sterile intensive care unit especially if you can get the same care and treatment at home than in ICU/PICU?
End of life care is also part of our intensive care substitution service at home!
If you think about it, when it comes to end of life in intensive care, nobody wants to approach their end of life in ICU/PICU and we are enabling ICU/PICU patients to leave ICU/PICU and approach their end of life at home.
Last but not least, you may wonder if this is safe?
To see for yourself, just check out our case studies here
https://intensivecareathome.com/case-studies/
We are providing intensive care at home services exclusively with ICU/PICU nurses that have a minimum of two years ICU/PICU experience and have completed a post-graduate critical care certificate. In fact our nursing team on average have a total of 8-10 years ICU/PICU experience.
Furthermore, on top of our highly skilled nursing team we have also accomplished 3rd party accreditation for intensive care at home nursing including mechanical ventilation.
You can find out more about our quality and accreditation here
https://intensivecareathome.com/accreditationquality/
Kind Regards
Patrik
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care (also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator, if you want to know how to get funding for our service or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
Also, check out our careers section here
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in the Melbourne metropolitan area, northern suburbs, Mornington Peninsula and in South Gippsland/Victoria.
We are an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
Also, have a look at our range of full service provisions here
https://intensivecareathome.com/services
We have also been part of the Royal Melbourne health accelerator program for innovative health care companies last year!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update!








