Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
WHAT ARE THE LONG-TERM EFFECTS FROM A TRACHEOSTOMY BESIDES BEING ALIVE? LIVE STREAM!
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients and the question today is
Why is There a Negative Impression of a Tracheostomy? I Thought it Was Part of the Course in ICU?
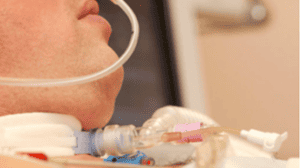
Hello and welcome to another Intensive Care at Home and intensivecarehotline.com livestream. Today’s topic is “Why is There a Negative Impression of a Tracheostomy? I thought it was part of the normal course in ICU”. I’m your host, Patrik Hutzel, founder and managing director of Intensive Care at Home and Intensive Care Hotline. I am bringing this topic to you today, and it was actually a request from one of our viewers who was actually on another live stream who asked the question and I didn’t have time to elaborate on it then, which is why I’m doing a designated live stream to that very question today.
We will be going for approximately an hour. I will go through today’s topics and then I will also have time to answer some questions that came in during the week. Or if someone wants to dial in live on the show and answer their question on the phone live on the show, I can also share the phone number that you can contact me on while I’m on the live stream here. So just let me know what you would like to do.
Now, before I get into today’s topic, you may wonder what makes me qualified to talk about today’s topic. So again, my name is Patrik Hutzel. I’m the founder and managing director of Intensive Care at Home and intensivecarehotline.com. With Intensive Care at Home, we are providing services for predominantly long-term ventilated adults and children with tracheostomy at home, but also for adults and children that are not ventilated, have a tracheostomy, but also for adults and children that are BiPAP (bilevel positive airway pressure), or CPAP (continuous positive airway pressure) ventilated that require home TPN (Total Parenteral Nutrition), home IV fluids, home IV antibiotics, seizure management and so on. Basically, everyone that needs an intensive care nurse in the home or a critical care nurse in the home to keep them out of home predictably.
We are currently operating all around Australia in all major capital cities, including rural and regional areas. We are also starting to operate in the United States as well as we have inquiries from the UK as well. If you’re in the UK, please contact us as well. We can point you in the right direction one way or another.
My background is critical care nursing. I have worked in critical care for over 20 years in three different countries where I also worked as a nurse unit manager for over five years. I was also part of pioneering Intensive Care at Home in Germany nearly 25 years ago and we successfully rolled out Intensive Care at Home there and then just as much as we rolled it out successfully in Australia in the last 10 years. I have also been consulting and advocating for families in intensive care for over 10 years as part of my intensivecarehotline.com consulting and advocacy service for families in intensive care. I’ve been consulting and advocating for families in intensive care all around the world.
So enough talk there. Let’s get into today’s topic, “Why is There a Negative Impression of a Tracheostomy? I thought it was part of the course in ICU”. What a great question actually, and let me get the record straight here today. That first of all, a tracheostomy is not part of the normal course in intensive care. And as much as sometimes in my videos I might give it a negative impression too, the reality is that with our Intensive Care at Home service, most of our clients have a tracheostomy, but it’s still not part of the normal course in ICU. So again, let me get the record straight here. For any patient in ICU, the ultimate goal should be to wean them off a ventilator and avoid a tracheostomy. Full stop.
Let me repeat that. The ultimate goal of a patient in ICU who’s on a ventilator with a breathing tube in their mouth, the ultimate goal is to take out that breathing tube as quickly as possible. That is the ultimate goal. And if someone goes into intensive care and is not ventilated, maybe they go into intensive care for inotropes, for vasopressors, for any condition that doesn’t require a ventilator and the breathing tube, the goal once again is get those patients out of ICU as quickly as possible without even needing to think about mechanical ventilation, right?
Now, once I argue that the majority of patients in intensive care is mechanically ventilated with a breathing tube, once again, the goal is to remove that breathing tube, wean them off the ventilator as quickly as possible and avoid the tracheostomy. Now, here with Intensive Care at Home and with Intensive Care Hotline, we are very much serving a niche market, which means a lot of the videos and content that we’re putting out there is about tracheostomy, is about how to avoid a tracheostomy, what to do if someone has a tracheostomy, what are the options, right?
But we are still talking about when you look at the bigger scheme of things, intensive care is a niche. That’s number one. Number two, having a tracheostomy in intensive care is also a niche, right? So we’re talking about a niche within a niche, but it gets better than that. With Intensive Care at Home, we are a niche within a niche within a niche because once someone has a tracheostomy in intensive care, then what’s next? If the tracheostomy can’t be removed, if the ventilator can’t be removed, then what’s next? Then you got to look at services like Intensive Care at Home. But the bottom line is this, only a minority of patients in intensive care has a tracheostomy. And I’m sure there’s some smart people out there who have the statistics for that, how many the percentage of patients in intensive care that require tracheostomy. I wouldn’t know. I don’t have the statistics. I would think from my experience, 10 to 20% of patients in intensive care have a tracheostomy. Some of them temporarily, some of them on an ongoing basis.
So I hope that you can understand now that it’s not part of the course in ICU on a large scale. Why do we talk about tracheostomy here so often with Intensive Care at Home or Intensive Care Hotline? Simple. If you have a loved one in intensive care and all of a sudden the discussions around a tracheostomy are started and you start doing your research, well, of course you want to understand, “What is a tracheostomy? What does it mean? Can it be reversed? What if it can’t be reversed? What are our options?” Now, of course, you got to do your research, and then that’s when you are coming to find my videos and my content because I’m talking about it and I’ve talked about it a lot for the last 10 years.
So this is why probably when you’re entering our world here, you think a tracheostomy is the normal course of action. It’s not. It’s, again, a niche segment. But it’s a niche segment that creates a big flow on effect. It creates a lot of issues, it creates a lot of problems. What can we do to, (A), eliminate the tracheostomy? (B), if the tracheostomy is needed, how can we get it removed? If we can’t get it removed, how do we manage quality of life going forward? Quality of end of life going forward. And the list goes on.
Right. So this is why I want to make this video today because I guess there’s a lot of misinformation out there. When you are confronted with your loved one having a tracheostomy or maybe yourself, you got to go down this rabbit hole of, “Okay, what does it all mean? Can it be reversed? What if it can’t be reversed? What are the options?” So that’s probably why you’ve coming to my videos because you’re having this massive issue. But for now, let’s go one step back. Again, isn’t a tracheostomy part of the normal course in ICU? Once again, it is not. There is a video and a blog post that I wrote a couple of years ago maybe, something along the lines of how to remove the breathing tube in intensive care. How to remove a breathing tube in intensive care, and that is the ultimate goal. That is the ultimate goal for every patient in intensive care. Nothing else. Nothing else.
Let me be very clear here that nothing else is the goal. Now, of course, there are situations where this can’t be achieved. But for the overwhelming majority of patients in intensive care, this can be achieved. I’m just looking for the article that I wrote because I think this is a really good resource. I can’t find it now. But anyway, I will find it eventually. That the ultimate goal is to remove the breathing tube. Full stop. If that can’t be achieved, then discussions need to be started about a tracheostomy. Now, also to explain, if a breathing tube can’t be removed and someone can’t come off the ventilator, the cutoff time to move towards the tracheostomy instead of the breathing tube is about day 10 to day 14. Now, during COVID you would’ve seen there would’ve been huge delays around that. It wasn’t at the day 10 to day 14 mark, (A), because of high oxygen dependency, high PEEP, and also resource availability. But generally speaking, when you look at the research, it’s day 10 to day 14 when someone should have a tracheostomy, when the breathing tube can’t be removed.
But once again, what we are seeing over and over again is that intensive care teams do not move towards extubation as quickly as possible. They know that a tracheostomy is their safety net. It shouldn’t be their safety net. Their safety net should be to do all the right things, wean sedation off as quickly as possible, get patients mobilized as quickly as possible. That should be the safety net. Only if all of that fails and people have done what it takes beyond the shadow of a doubt, only then can you move towards a tracheostomy. I can’t stress this enough.
So when it comes to the discussions around tracheostomy or no tracheostomy at day 10 to day 14, often what ICUs say is, “Well, it’s either tracheostomy or it’s end of life.” It’s sort of this black and white approach. My argument around that is, “Well, what’s the rush with end of life?” A tracheostomy has its time and its place. I’m not opposed to it at all. I’m opposed to it if the right things haven’t taken place before a tracheostomy is offered. And what needs to take place before a tracheostomy is offered is wean someone off a ventilator as much as you can, take them out of an induced coma, mobilize them, do physical therapy, do breathing exercises, wake them up.
And that’s sometimes not possible because someone might have a brain injury and they can’t wake up in spite of people switching off sedation. But let’s just assume there’s no neurological condition, i.e, there’s no stroke, there’s no brain injury, then move towards extubation. Extubation is the removal of the breathing tube as quickly as possible. Because once a tracheostomy has been done, that’s when the real issues start. It’s much easier in the long run to deal with issues before a tracheostomy needs to happen. It’s much easier to remove the breathing tube and then move towards a hospital floor or a hospital ward as quickly as possible, because once a tracheostomy is done, you can no longer move towards a hospital floor or a hospital ward because it requires the skills of intensive care nurses or seize a critical care nurses to manage tracheostomy predictably, right?
So then if it comes to that sort of point where the ICU team is telling you, “Okay, well we either can do a tracheostomy or we can move towards end of life,” my recommendation here is this. Number one, what’s the hurry with end of life? You can do a tracheostomy and then you can reassess. Once someone has passed away, there’s no time for reassessment, right? So my advice is always make a decision today that you don’t regret in 12 months, in 24 months. And if you move towards end of life today, you might regret it tomorrow. You might regret it 12 months later because there is no return from that as far as we know, right?
I can’t tell you how many families come to us that had loved ones in intensive care and the loved one passed away maybe 12 months ago, 18 months ago, and they come to us and they say, “Hey, I’ve just found your website now, and I had no idea that there’s consulting, there’s advocacy, there’s information out there because we felt like our only option was end of life. And now I feel depressed because I didn’t realize I have a choice.” Well, you always have a choice. Everything in life is negotiable. Everything. So you got to approach it with that mindset and don’t make the mistake of giving in to the perceived pressure from intensive care. It’s only perceived, not more than that. And don’t let them guilt trip. I’ve made a whole video about that. “What if the intensive care team is guilt tripping you?” Don’t let anyone guilt trip you.
This is a once in a lifetime situation that you can’t get wrong. You can’t afford to get this situation wrong, right? By doing a tracheostomy, if it comes to that point, it buys you time, it buys your loved one time. You can see where it’s going. If it’s not going well, okay, there’s still plenty of time to talk about end of life. Still plenty of time.
Okay, so what’s next? If a tracheostomy has taken place, if that’s the only option besides end of life, then that buys your loved one time, but it also increases the chances of your loved one getting off the ventilator because what happens next is you can pretty much stop sedation straight away. So when someone has a breathing tube in their mouth, it’s very uncomfortable. That’s why they need to be induced into a coma. And there are alternatives for that as well. I actually did a podcast with Kali Dayton from Dayton ICU Consulting a few weeks ago. Kali is a nurse practitioner in the U.S. and she’s worked in a unit, I believe, in Colorado in the U.S. where they never sedated a patient when they had a breathing tube. And they had fantastic outcomes. They never had patients with a tracheostomy really.
One of the main reasons why patients end up with a tracheostomy is really that when you put the breathing tube in and you induce them into a coma, patients decondition very, very quickly because they’re asleep for the next 5, 6, 7, 8, 9, 10 days. Muscle wastage is real. And then when you try and wake them up, their muscles have deteriorated. They deconditioned so quickly that it’s a real challenge to actually work them up towards weaning off the ventilator. They can’t breathe because they’re so weak.
So often the reason why your loved one can’t be weaned off the ventilator and needs a tracheostomy is not so much that that disease process has led them to not being able to breathe. What’s happened really is that the induced coma has made them so weak that they can’t be weaned off the ventilator. But that is an advantage of a tracheostomy that when you have done the tracheostomy from, I argue, with nine out of 10 patients, you can stop sedation straight away. You can get them to wake up, assess their neurological condition and talk to them and help them through weaning off the ventilator pretty quickly.
It’s also easier to mobilize a patient once they have a tracheostomy. It can be perceived as unsafe to mobilize someone with a breathing tube instead of a tracheostomy. And I agree that it’s more risky, but it’s still can be done. A good ICU will mobilize someone even with a breathing tube instead of a tracheostomy. But once someone has a tracheostomy, there are no excuses not to mobilize your loved one with a tracheostomy. There are exceptions to that rule. The exception to that rule is if someone has trauma, they have fractured ribs or they are waiting for surgery after a motor vehicle accident or whatever. Yes, there are exceptions to the rules in terms of when you can mobilize someone. But let’s assume there are no fractures, there’s no head injury with increased brain pressures, which is also a contraindication to mobilize someone. There’s no reason why your loved one with a tracheostomy can’t have sedation and opiates off and start the mobilization process very, very quickly.
Now, I do need to make a distinction here probably between what’s happening in the U.S. and also in other countries. In the U.S. you have the LTAC (long-term acute care) facilities after intensive care. One of the reasons ICUs in the U.S., from my perspective, are not doing what they’re supposed to be doing and weaning someone off the ventilator and the breathing tube as quickly as possible and sent them to LTAC is simply because they know the LTAC is there. Whereas in other countries like in the U.K. or in Australia, you’ve got to move patients pretty quickly. You have a real incentive to move them because there are no LTACs. But in either, doesn’t matter which country, you’ve got to watch like a hawk that intensive care teams are weaning your loved one to the best of their abilities one way or another.
So coming back to this sort of point where your loved one has a tracheostomy, the goal still hasn’t changed. The goal has not changed for your loved one to have the tracheostomy removed and the ventilator removed. The goal will never change. Now again, there are exceptions to the rule. The exceptions are, let’s just say someone has a C1, C2 spinal injury. As far as we know in 2023, there are no options for C1 or C2 spinal injury patients but to be ventilated for the rest of their lives with a tracheostomy. Same is applicable for patients, for example, with motor neuron disease, end-stage motor neuron disease, or cerebral palsy. So there are exceptions to the rules. But if your loved one is in ICU with a tracheostomy, let’s just say after a pneumonia, COPD (chronic obstructive pulmonary disease), asthma, ARDS (acute respiratory distress syndrome), sepsis, cardiac surgery, Guillain-Barré syndrome, the list goes on, motor vehicle accident, brain injuries, the list goes on, the goal should always be to have the tracheostomy and the ventilator removed eventually.
And if that all fails, of course you got to look at services like Intensive Care at Home. Of course you do, because that is your best option to go home. But you can see like I’ve explained in the beginning, intensive care is a niche. Patients with a tracheostomy in intensive care are rare, but they do exist of course. So we’re talking about a niche within a niche. And when you then go down that rabbit hole even further, when you look at the patients with a tracheostomy that can’t be weaned off a tracheostomy, that can’t be weaned off the ventilator, that’s when you come to us like Intensive Care at Home. But you can see it is not part of the normal course of an ICU patient. And it shouldn’t be part of the normal course.
Again, I don’t have the stats. I would think that 10 to 20% of intensive care patients need a tracheostomy, temporary or permanent. And then again, I would argue for all of the patients that have a tracheostomy, there would only be a small proportion, but also a growing proportion of people that need a tracheostomy indefinitely.
Okay. So now, if your loved one is then, God forbid, faced with the challenge that they can’t be weaned off the ventilator and have a tracheostomy, absolutely, look, come to us at Intensive Care at Home. Contact us and we can help you take your loved one home, no question asked. Or if you’re at a hospital watching this, if you’re in ICU watching this and you have bed blocks and you need your loved one home with Intensive Care at Home, please contact us. We can 100% help you with that. Same is applicable when let’s just say there are plenty of patients in ICU that have a tracheostomy or ventilated, and then you take them off sedation, you stop the opiates, you wake them up. They might be able to be weaned off the ventilator pretty quickly, but they might require the tracheostomy for a long period of time maybe because of their inability to swallow, maybe because they have a lot of secretions.
So there are definitely some situations where patients need a tracheostomy in the long run but can be liberated of the ventilator. We are having clients with Intensive Care at Home that are not ventilator dependent, but have a tracheostomy and therefore need the intensive care nurse or the critical care nurse 24 hours a day at home to stay out of intensive care predictably, because that’s what it all comes down to with Intensive Care at Home. You want your loved one at home predictably. You don’t want your loved one to bounce in and out of ICU, which is what we’ve seen when patients go home with tracheostomy or ventilated and they don’t have critical care nurses 24 hours a day.
We have seen patients die unfortunately at home when family members couldn’t manage medical emergencies or support workers. People that are employed by other organizations that are picked off the street and all of a sudden are meant to do the work that intensive care nurses are doing who need at least five years of training. So we know the pitfalls. Don’t fall for them.
If you’re stuck in a situation like this where your loved one wants to go home, needs to go home because they’ve been in ICU for too long, contact us because we know there’s no quality of life in intensive care, and there’s also no quality of end of life. Part of what we do with Intensive Care at Home is also palliative care. So we have provided end of life care at home for patients that did not want to pass away in intensive care. And the bottom line is this, for you as a family member, I’m assuming you are a family member if you’re watching this, you don’t want to spend day and night in intensive care. I’m sure you don’t.
And again, if you’re an intensive care unit, if you’re a doctor or a nurse watching this, if you’re a hospital manager, we are cutting the cost of the intensive care bed by approximately 50% and we can free up your intensive care bed that is in high demand anyway. We know that intensive care bed are the most sought after beds in a hospital. Full stop. Intensive care doctors, intensive care nurses are the most sought after staff in a hospital. So we know you’ve got a real problem if you have a long-term patient in intensive care.
Now, another question that we get quite frequently is I talked about the day 10 to day 14 mark when someone can’t come off the ventilator with a breathing tube, that’s the time when someone should have a tracheostomy. Yes, they should. And then we get a lot of questions around, “Well, can we wait just another two or three days before we do the tracheostomy? Maybe my loved one will come off the ventilator in that period of time.” Yes, absolutely. You can probably delay that decision for a few more days only if your loved one has been off sedation for a few days already. They are waking up, they’re obeying commands, they have a good strong cough. They are on minimal ventilator settings like on minimal support. They need to be breathing on pressure support ventilation mode or CPAP ventilation mode. Their arterial blood gases need to look good. PO2 needs to be within a certain range. Carbon dioxide needs to be within a certain range. pH needs to be within a certain range. Yes, that is the exception to the rule.
The problem that we see over and over again, and obviously it’s also something that I’ve seen over and over again when I worked in critical care still, that if it comes to the day 10 to day 14 mark and the inability to wean off the ventilator and the breathing tube, is patients have been too heavily sedated and too long sedated. Sometimes unnecessarily, sometimes it is necessary. Again, one of the biggest contributing factor for someone to be needing a tracheostomy is simply muscle wastage from a prolonged induced coma. This is really something you need to avoid as much as you can. So basically, if you are watching this video and your loved one has been in intensive care, let’s just say, for 24 hours, has been on a ventilator, in an induced coma and a breathing tube for 24 hours, ask them straight away when can they take them off the ventilator. Critical question to ask. Absolutely critical question to ask.
And again, if you look at my interview that I’ve done with Kali Dayton a few weeks ago, she says in her experience, sedation and opiates are not necessary for intubation at all. Now, I haven’t seen it in practice, but obviously there is one unit in particular that can do that. And if one unit can do it, other units can do it as well. So look out for the video or the podcast that I’ve done with Kali and you can get all the information there.
Okay, so I hope that wraps up today’s topic. I will in a minute read out or answer questions that came in during the week. Now, if you have any questions in regards to today’s topic, please type them into the chatpad. If you want to get on live on the show, you can do that as well. I will give you the phone numbers. I’ll type in the phone numbers if you want to dial in live on the show and have your questions answered. I’ll just type them in. If you are in the United States, you can call this number. If you are in Australia, you can call the number that I’m typing in now. And if you are in the U.K. you can type in this number or you can just type your questions in the chatpad and I will answer them in the chatpad.
Okay, so let’s look at questions that came in this week. I’ll just quickly need to look at my phone and look at my emails so that we can get to as many as we can. Just give me one second. Don’t be shy asking questions. You know that I will answer them if you have them.
Okay, so now questions. Okay, question from Anna. “My brother had an aneurysm coil surgery a day after he accumulated liquids in the brain. They put a hole from his head to his abdomen. He’s not waking up for the sedation. The doctors are saying that they need to put a breathing tube in his throat. They need to take him off the ventilator. What do we do to wake him up completely? He moves a little.”
Okay, this actually ties right in with today’s topic really. Now, it is kind of unusual if you had an aneurysm coiling to be intubated. A lot of patients that I’ve seen that had an aneurysm coiling just come out of surgery, go to intensive care for 24 hours for monitoring, and they’re often not intubated. However, something doesn’t add up here. I think if he accumulated liquids in the brain, maybe he had a bleed. And if he had a bleed, he probably lost consciousness, which is probably why they intubated him.
“They put a hole from his head to his abdomen.” Probably to drain some CSF, which is the spinal fluid and the brain fluid. “The doctors are saying that they need to put a breathing tube in his throat,” which they’ve probably done already. “They need to take him off the ventilator.’ Yeah, pretty much ties right in with today’s topic. He should not have a tracheostomy. The goal here is to wake up your brother as quickly as possible and wean him off the ventilator. Take him off sedation. Challenge here is if your brother has liquid in the brain, is that from a bleed? What is it? Where is it coming from? Is it a cyst? Is it something else going on there? Is it a brain tumor, God forbid? That’s the question.
Once they’re taking him off sedation, why is he not waking up? Is there something else going on? Does he have high intracranial pressures? Does he need intracranial pressure monitoring to wake him up so that intracranial pressures are stable before waking him up? If intracranial pressures are not stable, what alternative therapies are there to get those intracranial pressures back to normal and then wake him up? Okay, so it’s always about optimizing care and treatment so that you know can wean someone off the ventilator as quickly as possible.
You are saying the doctors are saying they need to put a breathing tube in his throat. So basically what you might be implying here that he might need a tracheostomy because a tracheostomy does go into the throat, but does go into the throat through the neck, whereas a breathing tube does go into the mouth into the throat. So anyway, “What do we need to do to wake him up completely? He moves a little.” Well, what needs to happen is he needs to have the sedation taken away completely and then needs to be checked out if he can wake up or not. Once again, if he can’t be woken up despite sedation being removed and opiates being removed and he can’t wake up because of the liquids in his brain, that’s when a tracheostomy might be needed.
You haven’t given enough information. So a lot of it depends on what ventilator settings is he on. Have they stopped sedation completely? Have they taken off opiates completely? Like I said, is there still CSF draining? Because you mentioned the hole from his head to his abdomen to drain fluids. Is other fluids still draining? You are probably referring to a VP shunt here. What ventilator settings is he on? Can he potentially be weaned off the ventilator pretty quickly but still needs a tracheostomy because he’s not waking up? He can’t swallow. The brain pressures are still too high. What do CT and MRI scans of the brain show? Is there temporary or permanent brain damage. That’s all contributing to your brother’s situation and the next steps. I hope that helps Anna.
Let’s move on to the next question or comment from Benny. Benny says, “My wife was in an induced coma over two weeks. Her blood pressure went down fast and she passed away from septic infection and pneumonia. I don’t believe the induced coma helped.” Okay, this is a comment that was made on one of my YouTube videos, but anyway. Okay, let’s read this out again to get the nuances of the question or the comment. So Benny writes, “They had my wife in an induced coma over two weeks. Her blood pressure went down fast and she passed away from septic infection and pneumonia. I don’t believe the induced coma helped.”
Okay, great question or great situation. And again, you’ve heard me saying it before, but I’ll say it again, the biggest challenge for families in intensive care is that they don’t know what they don’t know. They don’t know what to look for, they don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care. They’re also often jumping to conclusions and they’re not connecting the right dots.
Now, when someone goes into intensive care with a sepsis or a septic shock or a septic infection like you mentioned it here, Benny, an induced coma is inevitable, because again, someone needs to be intubated, they’re losing consciousness, they need treatment for the sepsis. You haven’t shared where the sepsis came from. Was it sepsis from a pneumonia? Was it a bloodstream? Fake sepsis? What was it a UTI, a urinary tract infection? Wherever the source of the sepsis was. Most patients that come to intensive care with septic shock need to be intubated and i.e need to go into an induced coma. And then these treatment options for sepsis go their cause, like often IV antibiotics, IV antifungals, sometimes IV antivirals depending on what infection it is.
Furthermore, you mentioned that your wife’s blood pressure went down fast. She would’ve needed inotropes or vasopressors. Lot of patients with sepsis go into kidney failure in intensive care. They need often kidney dialysis or kidney hemofiltration at least temporarily. They also need often steroids. Your wife might have been on steroids. Now, I obviously can’t say from here with limited information why your wife passed away. You mentioned she had a septic shock and pneumonia, but maybe there was something else. I don’t know.
Sepsis does have a higher mortality rate attached to it compared to other diseases in intensive care. So it’s hard to say what exactly happened, whether your wife had all treatment options that were available. You haven’t shared whether you think your wife was in a good ICU, should she have been transferred to another ICU, maybe where other treatment options are available. Sometimes we have families contact us and they’re somewhere in a rural area, in a small ICU, and you can already see that ICUs have limited resources, limited experience. Is it then worthwhile for your loved one to get transferred to a metropolitan ICU? You haven’t shared where your wife was. But those are the questions that need to be asked in such a situation.
There’s also the question that remains, Benny, was your wife in a real or in a perceived end of life situation? So what I mean by that is a real end of life situation is no treatment, no surgery, no nothing can save someone’s life. A perceived end of life situation is existent for many patients in ICU where ICU says, “Well, we don’t think that your loved one will have any quality of life if we keep treating here and that any treatment is ‘futile’.” Futile means it is of no perceived benefit for a patient. But again, what is your perception?
And again, the perceived end of life situation is when treatment is being stopped and patients die despite of you could have continued treatment and the patient would’ve probably lived for longer and could have turned the corner if they had only continued, right? And I’ve seen this many, many times where intensive care units are not putting their best foot forward where they’re not treating to the best of their abilities, right? Okay, Benny, I’m very sorry to hear about your wife’s passing, but this is my take on the situation and I hope that helps.
Now, here’s an email from Andrew who writes, “My dad has come down with a streptococcus infection, and then it turned into streptococcus A, bacterial infection into his kidneys for months and went undetected by several doctors. He finally went to the emergency department where he collapsed and went into a coma, medically induced I believe. The doctors kept telling us and my father’s wife that she should consider donating his organs and she said no, because she knew my dad’s wishes. Then two weeks later, I went into my dad’s room because I had been treating him using solfeggio frequencies to aid in his healing, and I grabbed his hand and his eyes opened wide. Since then, he has been getting somewhat better, but they had a tube in his throat for breathing and it punctured his lung and so they put in a tracheostomy. Well, if they punctured his lung, it means they caused the pneumothorax, so they put in a tracheostomy.”
Well, there’s no need to put in a tracheostomy just for a pneumothorax. What you need to do for a pneumothorax is put in a chest drain and suck the air out of the lungs so they can expand again.
“We are in Catherine’s, Ontario, Canada, and the levels of care here are very poor due to bad management and bad attitudes. We have been asking about physical rehabilitation, but they keep making excuses as to why they didn’t do it. But the one nurse told me she was one nurse taking care of three ICU patients alone. I know a number of staff that have left this hospital because of COVID job mandates, and they’re always short-staffed. So he gets taken off ventilation maybe two times a day for an hour or two. Long story short, is your Intensive Care at Home something you have in Canada, Niagara, Ontario, Canada? We want to be able to help my dad and his wife to get better care, but the hospital system here is very difficult to deal with and his level of care is not to a good standard. If he could be home, it would be great. And he’s also using dialysis every three to four days,” from Andrew.
That’s a very sad situation, Andrew, and I’m very sorry to hear that. Unfortunately, we are not in Canada at the moment. We are operating all around Australia in all major capital cities. So if you are watching this, if you’re in Australia and you have a similar situation, please contact us. But we are not in Canada as yet.
But Andrew, coming back to your question, I’m surprised they had to put in a tracheostomy just because they punctured his lung and your dad had the pneumothorax. They should just treat the pneumothorax with a chest tube, suck out the air and let the hole close itself, and then the lung should be back to normal. So there might have been other things going on as well why they put in the tracheostomy. And I’m very sad to hear that the levels of care are poor due to bad management and bad attitudes. If one nurse is taking care of three ICU patients alone, that’s simply unsafe. That is very, very unsafe and that’s really sad to hear.
If he gets taken off the ventilator maybe two times a day for an hour or two, is he getting mobilized as part of that? Is he getting mobilized… You also haven’t said how long your dad has been in ICU. It’s not clear to me. No, it’s not clear to me how long. It also depends on how long. If someone has been in ICU in a situation like that for a couple of weeks, it’s probably too early to look at Intensive Care at Home. If your dad can’t come off the ventilator beyond the shadow of a doubt, yes, absolutely, Intensive Care at Home is definitely an option. If the ventilator can be removed but the tracheostomy can’t be removed, absolutely look for Intensive Care at Home. But again, we are not in your area, Andrew. But a practical tip for you in this situation is really get him mobilized. Let them do weaning trials, breathing trials, coughing exercises, encouragement, good nursing care such as regular washes, but also things like a shower will do wonders.
A good ICU will have shower facilities for those patients. They can put them on a shower trolley. If they don’t, they’re simply making excuses. But what is concerning is that there’s one nurse for three patients in ICU. That is simply dangerous. That is unsafe. One has to question whether the COVID jab mandates that you’re referring to and get staff to leave intensive care are making sense if there are not enough nurses and doctors to look after these critically ill patients. So I hope that helps. Also, you’re mentioning he’s having dialysis every three to four days. Again, dialysis is not an issue with Intensive Care at Home. If we were in your area, we could do that. Or if you are in Australia watching this and you want your loved one at home with dialysis, we can definitely do that as well. Even if they’re ventilated and having a tracheostomy and dialysis, that won’t stop us from doing that.
So Andrew, keep up the fight for your dad and do not give up. Watch them for what they’re doing. Keep holding them accountable and make sure he’s getting mobilized every day. Make sure he’s getting very, very good nursing care. Make sure he’s getting all the TLC he needs there. But that’ll be very difficult with one nurse looking after three patients. When I worked in ICU, most ICUs that I worked in, it’s a one-to-one nurse to patient ratio, and that’s how it should be. It should not be not less than that. Everything else is simply dangerous.
Okay. Then next question comes from… That’s not good. It doesn’t give me the name. It’s just an email that’s been sent with an email address that doesn’t allow or doesn’t give away the name. So reader writes that her frustration is that, “Comfort care for my mother, being they won’t allow her home with me, being that they don’t see it as a safe discharge and the only other options are out of our area and she’ll continue to be bedridden with no forms of therapy. She suffered a stroke where she’s now paralyzed and can’t speak and neurological status isn’t great. They think this will be her life in a vegetative condition.” Right. And I can see that this subscribe as actually in the U.S.
But anyway, you haven’t shared whether your mom has a tracheostomy, is ventilated, you haven’t shared any of that. But let’s just run it in both scenarios. Let’s just make up two scenarios here. One is your mom is in a hospital with a stroke, doesn’t need a ventilator, doesn’t need a tracheostomy, breathes spontaneously, but she’s incapacitated and bedridden with a stroke. Can you take her home? Of course you can. If we can take clients home on a ventilator with a tracheostomy, you can take your mom home with a stroke without a tracheostomy and without a breathing tube. You just need to set it up correctly.
Now, it is negligent in my mind one way or another, whether she does or she doesn’t have a tracheostomy or a ventilator, it’s negligent in my mind why they’re not mobilizing her. There’s no reason why you can’t mobilize a patient that’s immobile. You look at everyone that’s driving around in a wheelchair. The commonality for those people is they’re all immobile and you can still mobilize them. So by your mom being bedridden and no form of therapy, that is simply negligent. Now, not much changes. Let’s just say your mom has a tracheostomy or has a ventilator or has both, not much changes. Once again, she could be mobilized. What does change is if you’re going home with a ventilator or with a tracheostomy, she will need ICU nurses 24 hours a day or critical care nurses 24 hours a day with Intensive Care at Home.
So one way or another, your mom can go home. The only reason she might not be able to go home, but you haven’t elaborated on that, is if she’s unstable, i.e, she might still be hemodynamically unstable. She might have high blood pressure, she might have low blood pressure, she might be on inotropes or vasopressors, she might be on dialysis, she might be on hemofiltration. You haven’t shared any of that. So I’m assuming that none of it is there. Therefore, for your mom to go home seems absolutely reasonable and it also seems necessary because there’s no quality of life in wherever she’s at the moment.
And if you don’t agree with comfort care, which is a euphemism for end-of-life care, then you should object that with every core of your being. You should object that. You should challenge it. I presume you are the power of attorney. You have every right to let your mother live and wait for improvement. You have every right to challenge whatever the intensive care team is telling you. They can’t just kill your mother without your consent. And they have to do everything beyond the shadow of a doubt to keep her alive and keep her improving, right?
So one way or another, whether your mom is ventilated or not ventilated, no tracheostomy or tracheostomy, she can go home. If we can take patients home on ventilation with tracheostomy, your mom can go home. The only caveat there might be you’ve got to set it up properly. We can help you with Intensive Care at Home if she’s ventilated, has a tracheostomy. If she’s not ventilated, you have to get some support structure at home, whether it’s with carers or support workers, disability support workers to make it safer because you can’t look after your mom 24 hours a day. If she’s bedridden and immobile, you’ll burn yourself out and she will probably be back in hospital in no time. So you got to look after yourself. You are paramount here. You can only look after your mom if you are well. Don’t burn yourself out. Set it up properly.
Whether it’s here in Australia, the NDIS (National Disability Insurance Scheme) or health insurance would pay for it, and it’ll probably be the same for you in the U.S. Someone will need to support you at home. Someone is paying for a hospital bed at the moment. Why would they not pay for home care? Generally speaking, home care is much more cost-effective.
So that might be another avenue for you to look at as a next step. Get the funding, get the money to get your mother out, and then look at what services are available. There would be home care companies that can do that level of care for your mom. Probably not so much with Intensive Care at Home. I do believe we are pretty unique. But if your mom is not ventilated, doesn’t have a tracheostomy, there must be a home care organization out there that can help you with taking your mother home. So I hope that helps.
Now, if you have any questions, just type them into the chatpad because I’ll be wrapping up very shortly, see whether I have time for one more question depending how long it is. Oh, yes, here is a good one. Last question for today from Fred. Fred says, “My father is on the ventilator in ICU with a tracheostomy and he’s immobile. He has Guillain-Barré syndrome. Can he go home?”
That is a fantastic question. Absolutely, yes. So with Guillain-Barré syndrome, it’s sort of the typical example of someone staying in ICU for months and months on end. Slow respiratory wean. Very slow wean of the ventilator. And yes, your father would be a prime example to go home with Intensive Care at Home. I can’t see where you’re located, Fred, but if you are in Australia, which I assume you are, then you should absolutely contact us at Intensive Care at Home. We can help you take your father home with Guillain-Barré syndrome and wean him off the ventilator at home. I’ve seen so many patients in ICU with Guillain-Barré syndrome that have no quality of life, that are suffering immensely because they’re locked in a bed with no natural daylight in a busy, noisy ICU, and that’s simply not good enough. There’s quality of life at home with the Intensive Care team coming to your home. So definitely contact us with Intensive Care at Home there, Fred.
And also with Intensive Care at Home, if you’re an NDIS support coordinator or NDIS specialist support coordinator and you’re looking for a service that can help you with your participants with ventilation and tracheostomy, also Home TPN, please contact us as well. We can help you with any of those clients. It’s right our specialty. And if you are challenged with getting the nursing care funding through the NDIS or any other funding body, please contact us as well. We can help you with all of that. We wouldn’t be in business if we hadn’t developed enough insights about how to obtain the funding for the service for our clients.
Now, if you have a loved one in intensive care, go to intensivecareathome.com if you’re looking for home care for long-term ventilation and tracheostomy, BiPAP, CPAP ventilation, even if you loved one isn’t ventilated but has a tracheostomy, Home TPN, home IV fluids, home potassium infusion, IV antibiotics, seizure management, we do anything that requires an intensive care nurse at home. Please contact us at intensivecareathome.com. Call us on one of the numbers on the top of our website or send us an email to info intensivecareathome.com.
Also, if you are at home already and you are ventilated, have a tracheostomy, or you are on BiPAP, CPAP ventilation, but you can no longer manage with current supports, please contact us as well. Again, all of our clients have 24-hour nursing care at home funded through NDIS, TAC (Transport Accident Commission), DVA (Department of Veteran Affairs), iCare, New South Wales, NISQ (National Injury Insurance Scheme in Queensland) and so forth, so we know how to go about it. Please contact us.
Go to intensivecarehotline.com. If you have a loved one in intensive care and you need help and you have questions, please call us on one of the numbers on the top of our website or send us an email to [email protected] with your questions.
Also, have a look at our membership for families in intensive care at intensivecaresupport.org. There you have access to me and my team 24 hours a day in a membership area and via email. And we answer all questions intensive care and Intensive Care at Home related. Once again, I also offer one-to-one consulting and advocacy for families in intensive care. We can participate and represent you in family meetings or with any negotiations with intensive care teams as well.
Now, if you need a nurse, an NDIS Nursing Assessment or any nursing assessment for your loved one, for the NDIS or for any other funding body, please contact us as well. We have a team of senior intensive care nurses that can help you with nursing assessments. If you need a medical record review for your loved one in ICU in real time and get a second opinion, please contact us as well. And if you need a medical record review after Intensive Care, please contact us as well. We offer medical record reviews after intensive care as well if you have unanswered questions, if you are needing closure or if you’re suspecting medical negligence.
Thank you so much for watching. Subscribe to my YouTube channel for regular updates for families in intensive care. Click the like button. Click the notification bell. Share the video with your friends and families, and comment below what you want to see next or what questions and insights you have from this video.
Thank you so much for watching.
This is Patrik Hutzel from Intensive Care at Home and intensivecarehotline.com, and I’ll talk to you in a few days.
Take care for now.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Sunbury, Bendigo, Mornington Peninsula, Bittern, Patterson Lakes, Frankston area, South Gippsland, Drouin, Warragul, Trida, Trafalgar and Moe as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran Affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care at Home, and I’ll see you again next week in another update.







