Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home.
In last week’s blog, I talked about,
SHOULD MY DAD GO HOME WITH INTENSIVE CARE AT HOME, SHOULD HE STAY IN ICU OR GO TO LTAC? LIVE STREAM!
You can check out last week’s blog by clicking on the link below this video:
So in today’s blog post, we want to elaborate on the ABC article from earlier in 2021, “Queensland mum with motor neurone disease denied life-prolonging surgery.” Now, for anyone that doesn’t know what life-prolonging surgery means in a situation where a patient has motor neurone disease, it quite frankly, refers to a tracheostomy. And a tracheostomy for a motor neurone disease patient, simply is life prolonging.
Now the most prominent figure that everybody knows is Professor Stephen Hawking that lived with motor neurone disease for decades with the tracheostomy. And he had much to contribute to society, much to contribute to science. And he lived a good quality of life, I think until his mid-seventies, until he passed away.
Now here at Intensive Care at Home, we are looking after clients at home with motor neurone disease. And some of those clients have a very good quality of life. They also contribute to their family’s lives. They contribute to science. They contribute to some of their employers and they live an incredible quality of life because of the lifesaving surgery, hence, a tracheostomy.
Now, who is anyone in this world to say, who should have a tracheostomy, and who shouldn’t. This is up to the individual to make that choice. Because in this day and age with Intensive Care at Home services, patients don’t need to live in intensive care. They can have a tracheostomy even if they stay on the ventilator for the rest of their lives, and they can go home with services like Intensive Care at Home, and it’s up to the individual to make that choice.
And it’s not up to intensive care professionals or anyone because the services are there. The choice is there. And the funding is there as well, especially here in Australia with the National Disability Insurance Scheme, the NDIS. But also hospitals can pay for it too, because it saves half of the cost of an intensive care bed if hospitals do a tracheostomy, get patients out of intensive care quicker, instead of letting patients die. End of life is a choice that people need to make themselves and not based on perceived resources, the resources are there, and it’s up to the individual to use Intensive Care at Home and go home instead of staying in intensive care with the tracheostomy, if they have motor neurone disease.
Here is the article I want to share from the ABC News posted on 18 Aug 2021,
“Queensland Mum with Motor Neurone Disease Denied ‘Life-Prolonging’ Surgery”

Queensland mother Gabriel Watkin says she has been denied “life-prolonging” surgery in her fight to live with motor neurone disease.
Day by day her lungs are weakening, so 53-year-old Ms. Watkin becomes more reliant on an oxygen mask to breathe. 
But a tracheostomy, she said, would allow her to breathe and live for longer through a tube inserted into her trachea.
“They’re taking away the right to extend my life,” Ms. Watkin said.
“Each day my lung capacity is reducing and my body’s ability to handle the life-prolonging surgery is decreasing.”
Ms. Watkin said the tracheostomy would also mean she could use her eye gazing technology to communicate.
Currently, she cannot wear her glasses with non-invasive ventilation, which stops her from speaking, emailing, using the internet, reading books, and staying connected with her friends and family.

In a statement, the chief executive of the Central Queensland Hospital and Health Service, Steve Williamson, said there was currently little evidence in Australia to suggest the clinical benefits would outweigh the risks of the procedure.
“These are very complex cases that are decided around individual circumstances. I cannot provide comment on other cases around Australia,” Mr. Williamson said.
“My first reaction was disbelief, then I was distraught,” Ms. Watkin said.
“Essentially they’ve handed me a death sentence.
“My five sisters have moved to Queensland to be near me, to support me, but the irony is that I probably should have moved to Victoria — maybe I would have been able to access a medical team that would accept my decision to choose to want to go on living.”
Motor neurone disease (MND) is a progressive and terminal disease that attacks the nerves in the brain and spinal cord, with respiratory muscle weakness occurring eventually in everyone with the disease.
There is no known cause or cure.
While tracheostomies are not widely performed in Australia for people with MND, it has been done in some cases but is performed more regularly in countries such as Japan.
Renowned physicist Professor Stephen Hawking underwent the procedure in 1985 and it kept him alive for 33 years.
The average life expectancy after diagnosis, however, is one to five years.

‘Medical lottery’
Victorian doctor Ian Haywood has MND and underwent a tracheostomy after developing pneumonia.
He said he faced initial hesitation from medical staff, who wanted to refer him to palliative care, but his wife pushed for the surgery and an ICU doctor who attended the same medical school as Dr. Haywood performed the procedure.
“I don’t know how difficult it would have been without my advantages, like private health insurance and lots of health industry contacts, but I’m concerned it would have been a lot harder,” Dr. Haywood said.

“Having that extra time with family meant a great deal to me and my family. Our son was four when I was diagnosed [in 2016] and I am so grateful to continue to be part of his life.”
Dr. Haywood said the case against Ms. Watkin appeared “manifestly unfair”.
“It seems to be a state-based medical lottery,” he said.
The Central Queensland Hospital and Health Service said it had and would continue to do everything it could to work with Ms. Watkin and her family to determine her ongoing needs and plan of care.
“Central Queensland Hospital and Health Service sympathizes with Ms. Watkin and her family and we understand they are working through a very difficult and debilitating diagnosis,” Mr. Williamson said.
He said a team that included specialists in intensive care, respiratory medicine, palliative care, and clinical ethics considered Ms. Watkin’s request over a number of meetings.
A passion for life
Despite the decision, Ms. Watkin hoped Queensland Health would reconsider.
MND Queensland confirmed that there were surgeons who are willing to do the procedure in New South Wales, but they were unable to take referrals from outside their own regions. 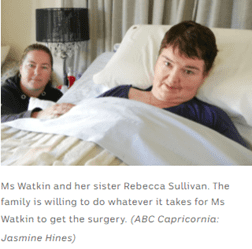
Ms. Watkin said she was also considering moving from central Queensland to Brisbane to pursue private treatment and said there was a private surgeon who was willing to perform the procedure.
She considered her life to be “bloody good”, and had already had percutaneous endoscopic gastronomy (PEG) surgery to feed, and saw the tracheostomy as the next — and final — step to prolong her life.
“[The surgery] will mean I’ll get to keep on living my life and hopefully be here to become a grandma,” she said.
“That’s a big hint to my sons.”
REFERENCE:
1 . Queensland mum with motor neurone disease denied ‘life-prolonging’ surgery
ABC Capricornia / By Jasmine Hines
2. Images credit to:
Now, if you have a loved one in intensive care and you want to go home with our service Intensive Care At Home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive Care At Home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Mornington Peninsula, Frankston area, South Gippsland, as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
https://www.melbournehealthaccelerator.com/
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care At Home, and I’ll see you again next week in another update.







