Podcast: Play in new window | Download
Hi, it’s Patrik Hutzel from intensivecareathome.com where we provide tailor-made solutions for long-term ventilated adults and children with tracheostomies and where we also provide tailor-made solutions for hospitals and intensive care units whilst providing quality services for long-term ventilated adults and children with tracheostomies, medically complex patients at home including Home TPN (total parenteral nutrition), tracheostomy care for adults and children not being ventilated, and also BIPAP (bilevel positive airway pressure) and CPAP (continuous positive airway pressure) ventilation, as well as IV antibiotics, IV potassium infusions, IV magnesium infusions, port management at home, PICC (Peripherally Inserted Central Catheter) line management at home, central line management at home, as well as Hickman’s line management at home.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients and the question today is
ICU Doctors are Telling Me Mom Won’t Be Able to Get Off Ventilation & Tracheostomy, Can She Go Home?
Hi, it’s Patrik Hutzel from intensivecareathome.com where we provide tailor-made solutions for long-term ventilated adults and children with tracheostomies and where we also provide tailor-made solutions for hospitals and intensive care units whilst providing quality services for long-term ventilated adults and children with tracheostomies, medically complex patients at home including Home TPN (total parenteral nutrition), tracheostomy care for adults and children not being ventilated, and also BIPAP (bilevel positive airway pressure) and CPAP (continuous positive airway pressure) ventilation, as well as IV antibiotics, IV potassium infusions, IV magnesium infusions, port management at home, PICC (Peripherally Inserted Central Catheter) line management at home, central line management at home, as well as Hickman’s line management at home.
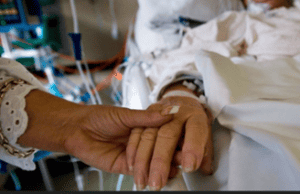
So, in today’s blog post, I want to answer a question from Petra who says, “My mom is 71 years old. She had been on the ventilator for four weeks and they put the tracheostomy and feeding tube in. She has been sedated a few times which takes her longer to come around than others. She has been responding to us with her eyes, she will smile or laugh at things that are funny. But the ICU team is saying it is involuntary and she isn’t doing it for them. They said she can’t breathe without the ventilator and the tracheostomy, and she won’t be able to come off it. We have asked to try different seizure medications along with having a neurosurgeon to examine her and a shunt that was placed from a stroke in 2007. Can my mom go home with Intensive Care at Home?” Well, that’s a great question, Petra.
Absolutely, if she can’t come off the ventilator, which I obviously can’t verify from here, but if they have tried multiple times and she can’t come off the ventilator, then the best place for her to optimize and maximize her quality of life or potentially quality of end of life is at home.
We can bring the intensive care in the home because she can’t really leave intensive care. Going to a hospital ward or hospital floor won’t be safe and it sounds like she would be stuck forever in the day in ICU unless you’re taking her home. So, it makes perfect sense.
Now, I know your next question is who’s going to pay for it and all the rest of it? Now, someone’s paying for the ICU bed, which is $5,000 to $6,000 per bed day. Now, with Intensive Care at Home that costs about 50% of the intensive care bed. So therefore, whoever is going to pay now, whether it’s publicly funded, whether it’s privately funded, someone has an interest to pay half of that because otherwise they keep throwing money in a bucket with a hole, whereas paying for Intensive Care at Home is half of the cost. Keep that in mind.
So, then once the funding is in place and I can assure you funding has never been an issue. All of our clients are not out of pocket that someone is paying for it and it’s not the clients. You got to keep the economics in mind here as well.
It’s not only the money, it’s also ICUs need the ICU bed and therefore, they need the ICU bed. Therefore, they also have an interest in getting your mom home and advocating for her. So, Intensive Care at Home really is creating a win-win situation.
Once the funding is sorted, we’ll get a team of critical care nurses together that look after your mom at home, and we are really excited about this. ICUs are not excited about looking after someone long-term in an ICU, but we are really excited about having or looking after your mom at home a lot. We’re excited looking after all of our clients at home because that’s what we’re in business for. We have the right staff and teams on our books that want to do this work. We’re not negative, we’re very excited about our work that we’re doing. We’re very positive about it and we’re getting the outcomes that our clients want, which is to stay home predictably.
So, I hope that answers your questions, Petra.
Now, currently with Intensive Care at Home, we are operating all around Australia in all major capital cities including regional and rural areas.
We are an NDIS (National Disability Insurance Scheme) approved service provider. We are a TAC (Transport Accident Commission) approved service provider in Victoria. We are an iCare approved service provider in New South Wales and we’re also an NIISQ (National Injury Insurance Scheme in Queensland) approved service provider in Queensland and the DVA approved service provider (Department of Veteran Affairs). We have also received funding from the Department of Health as well as from private health funds and public hospitals as well.
Now, if you are in the U.S. or the U.K., please reach out to us as well. We can probably help you in those countries privately or through other organizations.
Now, if you have a loved one in intensive care in a similar situation, please reach out to us or if you’re at home already and you have insufficient support, you need critical care nurses, but you don’t know how to go about funding, you don’t know how to go home from intensive care, you don’t know how to start the process, please reach out to us.
We’re also offering Level 2 and Level 3 NDIS support coordination to help you with an NDIS plan for nurses.
If you’re an NDIS Support Coordinator watching this and you have a client in a similar situation, we want to help you as well. We can help you with the advocacy. We can help you with nursing assessments, medical letters, and so forth. Please contact us as well.
If you are a CCRN looking for a career change, you have a minimum of two years ICU or ED experience or pediatric ICU experience and you are looking for a career change and you ideally have a postgraduate critical care qualification, we are offering a career change. We have jobs in Melbourne, Sydney, and Brisbane at the moment also in Country Victoria such as Bendigo, Warragul, but also Albury, Wodonga on the new South Wales Victorian border. We want to hear from you.
If you are an intensive care specialist watching this and you are looking for a career change, we are also currently expanding our medical team and I know in your ICU, you have bed blocks and we can help you with your bed blocks including for palliative care, end of life care at home as well.
If you’re a hospital executive watching this, we want to hear from you as well because once again, we know you’ve got bed blocks in your hospital in your ICU. We can help you eliminating those bed blocks and you’re not even going to pay for it, especially with the NDIS.
If you like my video, subscribe to my YouTube channel for regular updates, click the like button, click the notification bell, share the video with your friends and families, comment below what you want to see next or what questions and insights you have.
Thank you so much for watching.
This is Patrik Hutzel from intensivecareathome.com and I will talk to you in a few days.
Take care for now.









