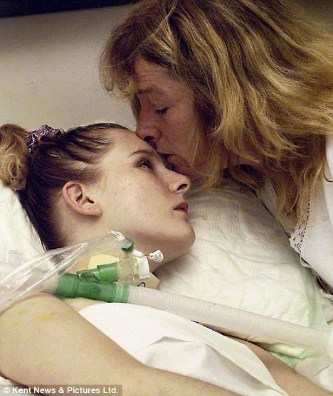Podcast: Play in new window | Download
Hi, it’s Patrik Hutzel, from INTENSIVE CARE AT HOME, where we provide tailor made solutions for long term ventilated adults and children with tracheostomy by improving their quality of life and where we also provide tailor made solutions to hospitals and intensive care units to save money and resources by providing quality care.
In last week’s blog, I answered a question from one of our subscribers and clients and Charlie asked last week,
You can check out last week’s question by clicking on the link here.
In today’s episode of of the INTENSIVE CARE AT HOME video blog, I want to answer another question from one of our readers and clients and the question today is
How long does a tracheostomy prolong life?
And that is a very good question.
And the question comes about because you know many of our prospects, clients and also people that just inquiry about our service have a loved one in intensive care with a tracheostomy and they simply want to know is the tracheostomy short term is it medium term is it long term?
Now in this particular situation, we’ve got an inquiry from a family who has their 19 month old daughter in intensive care with a tracheostomy after an anoxic brain injury.
Now, unfortunately, that little girl was born and was starved of oxygen during birth and ended up with an anoxic brain injury. She spent and has spent pretty much all of her life in intensive care on a ventilator with a tracheostomy and she is on the ventilator still, after all this time,
And obviously with a lack of specialist services in the community, she hasn’t been home yet. But obviously with a service like ours intensive care at home, she can go home. But the question is how long does a tracheostomy prolong the little girl’s life or anybody’s life for that matter?
And to cut the long short a tracheostomy and ventilation can prolong life for a long time. And you know, there could be debate about it, is it the right thing to ventilate someone for years to come or should it just be stopped?
But in this particular situation, you know, the family is grounded in strong religious faith and in their mind, only God can take away life.
And it shouldn’t be up to the intensive care team to stop life support just because the intensive care team thinks that this little girl wouldn’t have any quality of life.
Now, from my experience after having worked in intensive care for decades, there is definitely no quality of life/ quality of end of life in intensive care, that’s for sure.
But also after having worked for the same time with intensive care at home, there is definitely quality of life/ quality of end of life at home, not only for the little girl, but also for the little girl’s family.
You know, in intensive care,there’s a lot of noise. There’s a high risk for infection, especially at the moment with COVID-19.
But even outside of COVID-19 times, the risk for an infection in intensive care is simply through the roof. It’s huge.
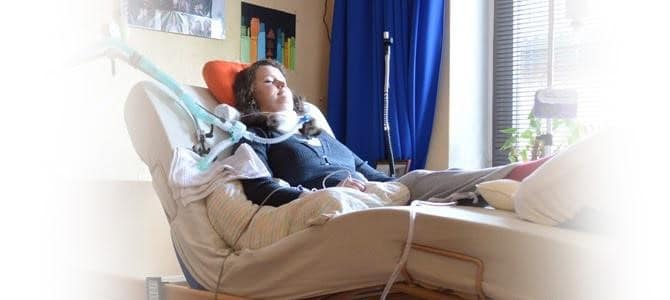
At home, you’re in a clean environment, and it’s just so much nicer, more client and family friendly and simply more holistic!
Also, intensive care units are very noisy places.
The lights are on 24 hours a day, people come and go 24 hours a day.
People have no privacy, no dignity.
Compare that with a homecare environment especially since this little girl is stable. She’s not on any inotropes or vasopressors.
She’s not on any sedation, it’s simply the ventilation and tracheostomy that’s keeping her in intensive care because obviously ventilation and tracheostomy requires the skill and expertise of intensive care and pediatric intensive care nurses.
So the only option for the little 19 month old girl is to go home with our service INTENSIVE CARE AT HOME.
So let’s look at the economics of this as well.
So an intensive care bed is around $5,000 to $6,000 per bed day. And intensive care at home is about 50% of that cost.
So, on an economic level, this is a no brainer that using intensive care at home cuts the cost of an intensive care bed by 50%
Furthermore, intensive care beds are in high demand, meaning that every bed that is more or less blocked with a long term patient, which is certainly the case with this 19 month old girl costs the health system $5,000 or $6,000 per bed day and you can do the maths how much that is over a 19 month period.
Also, if there are bed blocks in intensive care some critically ill patients, whether adults or children can’t get access to intensive care, can’t get access to those valuable resources and often surgery gets delayed or cancelled because of no ICU/PICU beds.
Sometimes patients get deferred to other hospitals via the emergency department because there are no intensive care beds available.
Again, what we do at intensive care at home is really giving patients and families choice.
But we’re also giving intensive care units and hospitals choice, by cutting the cost of an intensive care bed by 50%, and by creating valuable resources in intensive care by freeing up valuable, scarce, in-demand and precious ICU/PICU beds and other resources, such as equipment and staff.
I hope that answers the question.
How long can a tracheostomy prolong the life of someone?
And again, it can go on for a very long time. And it simply gives patients and families choice, irrespective of the judgment of other people what they consider as a good or not so good quality of life.
And in some instances it’s also about quality of end of life.
At the end of the day, this is up to the individual and we can help our client families to achieve that quality of life/quality of end of life at home.
Thank you for tuning into this week’s blog.
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care (also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator, if you want to know how to get funding for our service or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
And if you are an intensive care nurse or a pediatric intensive care nurse, and you’re looking to get out of the craziness of an intensive care unit and work for us in a much nicer and more holistic and client-centric family environment, you should contact us as well and should check out our career section on our website here.
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in the Melbourne metropolitan area, northern suburbs, Mornington Peninsula, Frankston area and in South Gippsland/Victoria (Warragul/Leongatha and Trafalgar).
We are an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
Also, have a look at our range of full service provisions here
https://intensivecareathome.com/services
We have also been part of the Royal Melbourne health accelerator program for innovative health care companies!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
https://www.melbournehealthaccelerator.com/
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update.