Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults& Children with Tracheostomies by improving their Quality of life and where we also provide tailor made solutions to hospitals and Intensive Care Units to save money and resources, whilst providing Quality Care!
In the last blog I shared
You can check out last week’s episode by clicking on the link here.
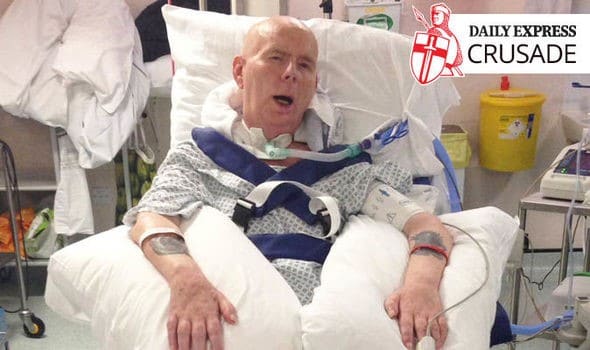
In this week’s blog I want to share another story of a 69 year old gentleman Alan Sheppard who has been unnecessarily confined to an ICU bed since December 2017 because Mr Sheppard is on a ventilator with tracheostomy since he has been diagnosed with MND (Motor neuron disease).
Mr Sheppard could go home with a service like INTENSIVE CARE AT HOME, however the health authorities prefer to pay nearly $4,000 per bed day in ICU instead of taking Mr Sheppard home, improve his quality of end of life and cut the cost of the ICU bed to less than 50%.
Health Service In Crisis: Daughter begs for terminally ill father to have care at home
The following article from the Express has been published a couple of weeks ago and illustrates once more how inefficient most ICU’s are run when it comes to long-term ventilated Patients and their families.
Health authorities keep Patients in ICU for much longer than necessary, pay a premium price on it, waste Millions of Dollars or Pounds of tax payers money and deny Patients and their families quality of life during what is an extremely challenging situation for Mr Sheppard and his family!
The article illustrates once again how basic human rights are being denied in the name of a bureaucratic and dysfunctional system.
Solutions are easy to come by with common sense, by creating win-win situations as INTENSIVE CARE AT HOME is a proven a successful care model, providing a genuine alternative to a long-term stay in Intensive Care!
We also know from experience that transitioning Patients home on ventilation with tracheostomy requires specialist skills form an accredited health service like INTENSIVE CARE AT HOME who operates according to best practice international guidelines when it comes to mechanical home ventilation. You can look up the best practice guidelines here
Unfortunately, most Intensive Care Units around the world chose to stay 30 years behind what has been common and best practice now in many countries for nearly 20 years and provide INTENSIVE CARE AT HOME services instead of Hospital Intensive Care when it comes to long-term ventilation with tracheostomy.
Here are the highlights and main points of the article
- “This situation is killing me,” Mr Sheppard’s 34 year old daughter Simone said yesterday. “We all just want Dad home. He wants to come home – his condition is deteriorating in hospital.”
- “I trained myself to look after him but I can’t do it 24 hours a day. We need some help. He’s on a ventilator and can’t be left alone.” Simone continues on.
- Hospital bosses have warned that they could “withdraw all NHS care” unless Mr Sheppard agrees to being sent away from his family.
- “This is all about money but where’s the sense in keeping him in an expensive intensive care bed instead of paying a lot cheaper rate to have him at home? “I know that’s more expensive than the cost of the private home in Peterborough but it’s only for a limited time and he will be with his family and friends.” His daughter Simone continues to advocate for her terminally ill Dad!
- His whole support group and life is here. “When the solicitor received a letter saying NHS care could be withdrawn, it terrified me.” Simone Sheppard
- “What does that mean? He’s paralysed and on a ventilator. The hospital has already told me they will not resuscitate him if something happens, which is not what he wants.” Simone Sheppard
- “He wants to live but they also won’t give him any antibiotics if he develops an infection. When palliative care in a hospice was mentioned, I was shockingly upset.”, Simone Sheppard
- “He’s stable, I’ve been told he’s got around two years, but Stephen Hawking made it to 76. This is not the first time we as a family have come up against a funding block.”, Simone Sheppard
Related article/video:
- This lack of appropriate care close to home is a sign of an underfunded care system. It needs to be urgently tackled by the Government so that the aspirations that the health and care system is personalised become a reality.
You can access the original article here or read it below
A PENSIONER with only two years to live has been trapped in hospital for six months – despite his family wanting to take him home. Allan Sheppard, 69, is unable to leave his intensive care bed because the NHS does not want to pay for local carers.
By SARAH O’GRADY
PUBLISHED: 00:06, Thu, Jun 14, 2018 | UPDATED: 22:42, Thu, Jun 14, 2018
However, it is happy to pay £5,300 a week for a private nursing home in Peterborough – 77 miles away from his home in High Wycombe, Bucks.
His devoted daughter Simone, 34, has been her father’s main carer since he was diagnosed with motor neurone disease at the beginning of 2016.
“This situation is killing me,” she said yesterday. “We all just want Dad home. He wants to come home – his condition is deteriorating in hospital.
“I trained myself to look after him but I can’t do it 24 hours a day. We need some help. He’s on a ventilator and can’t be left alone.
“He’s been in that hospital now without his friends, not sitting up, not going out. He’s only got a limited time left. I want him home. Peterborough is a long way from High Wycombe. It’s an hour and half drive at least.
How can I do that every day?” Motor neurone disease is the same condition that physicist Stephen Hawking suffered from before his death at 76 in March this year.
It is a fatal, rapidly progressing disease which attacks the nerves leaving people paralysed, unable to move, talk and eventually unable to breathe.
Mr Sheppard’s condition deteriorated to the point that he was admitted to intensive care at Wycombe Hospital in December last year.
Miss Sheppard, who was forced to resort to a solicitor and family advocate to help her fight her case against Buckinghamshire Healthcare NHS Trust, has also been banned from taking photographs of her father.
Hospital bosses have warned that they could “withdraw all NHS care” unless Mr Sheppard agrees to being sent away from his family.
Miss Sheppard, a former warranty claims engineer before she gave up her job to look after her father, found a local nursing care company which quoted £7,500 a week to help her care for her father, a former mechanic. The cost of keeping a patient in an intensive care bed is around £14,000 a week – rising to as much as £10,000 a night for those suffering from spinal injuries and other complex conditions such as MND.
“Since he’s been in hospital he’s lost his voice and lost weight,” she said.
“When he was at home he would have his dog Brogan and his friends around. “We would take him out in his wheelchair to walk Brogan and he could sit in his garage where his friends would come round to work on our project car.
“This is all about money but where’s the sense in keeping him in an expensive intensive care bed instead of paying a lot cheaper rate to have him at home? “I know that’s more expensive than the cost of the private home in Peterborough but it’s only for a limited time and he will be with his family and friends.
His whole support group and life is here. “When the solicitor received a letter saying NHS care could be withdrawn, it terrified me.
What does that mean? He’s paralysed and on a ventilator. The hospital has already told me they will not resuscitate him if something happens, which is not what he wants.
“He wants to live but they also won’t give him any antibiotics if he develops an infection. “When palliative care in a hospice was mentioned, I was shockingly upset.
He’s stable, I’ve been told he’s got around two years, but Stephen Hawking made it to 76.” This is not the first time the Sheppard family have come up against a funding block.
Miss Sheppard and her partner Ricky Thomas, 31, a fitness trainer and nutritionist, are £8,000 in debt after paying for care to supplement their efforts when funding was stopped last year before Mr Sheppard went into hospital.
Chris James, director of external affairs at the Motor Neurone Disease Association, said: “It’s important that people with terminal conditions like motor neurone disease have maximum choice and control over their care package – including their place of treatment. “It’s vital that care services and local councils are responsive when it comes to care in the home, including housing adaptations, as this has a massive impact on the quality of life for those living wit Emily Holzhausen, director of policy at Carers UK, said: “Coming out of hospital and getting the right care can be hugely stressful for families and the person needing care. “Delays in putting in place care arrangements and support for families pile unnecessary pressure and worry on families. Our research published only this week found 72 per cent of carers were suffering mental health problems as a result of their caring role with major stress factors including getting enough sleep and financial worries.
“Increasingly research is showing that people with complex needs are struggling to find the right kinds of care either in the home or close to home, which is what they want – to stay close to family and friends. This lack of appropriate care close to home is a sign of an underfunded care system. It needs to be urgently tackled by the Government so that the aspirations that the health and care system is personalised become a reality.
“There is a right to family life under the Human Rights Act which must be considered when putting care in place.” In March this year there were 154,600 occasions when a bed was occupied by a patient who was fit enough to leave hospital. Of these, 102,600 were in acute care wards.
As well as costing the NHS money, bed blocking increases the risk of infection for patients, leads to poor emotional health and a loss of independence and confidence. Phillip Blond, director of thinktank ResPublica, said: “The way health and social care work together needs to improve dramatically.
“The bed blocking crisis in the NHS is only getting worse, clogging up wards and leaving newly arrived patients on trolleys in corridors.”
A spokesman for Buckinghamshire Clinical Commissioning Group said: “Although we cannot comment on individual cases, it is the responsibility of NHS Buckinghamshire Clinical Commissioning Group to make every reasonable effort to ensure the specific needs of patients eligible for Continuing Healthcare are met through the Care Support Packages we commission.
“Any ongoing care for our patients must be safe, sustainable and at a level appropriate for their needs. Unfortunately, there will be occasional circumstances where, despite our best attempts, home care packages for those with very complex needs are not achievable or sustainable.
“In such cases, alternative care arrangements are sought as close to home as possible so that patients can maintain contact with family and friends. Sometimes, there may not be local organisations with the capacity or skills to meet specific needs and a placement may have to be sought beyond the patient’s local area.
“We recognise this is not ideal for either patient or family, and have every sympathy with them, but we must ensure we offer safe and sustainable care in the most appropriate environment, specific to individual clinical needs.
“Such out-of-area arrangements are often made on a temporary basis, until longer term solutions can be found closer to home.
“To this end we endeavour to work with patients and their families to ensure they receive the support they need while we continue to explore every care option available.
“When patients have complex healthcare needs, sometimes potential solutions that may seem appropriate on the face of it may not be fully able to meet those requirements, which is another consideration the CCG must bear in mind when making such arrangements.
“Patients with the capacity to make decisions about their own care have every right to refuse any proposed Care Support Packages if they wish, but regrettably must do so at their own risk.”h the disease.”
What is motor neurone disease?
MND is a fatal, rapidly progressing disease that affects the brain and spinal cord.
It attacks the nerves that control movement so muscles no longer work. MND does not usually affect the senses such as sight, sound and feeling. It can leave people locked in a failing body, unable to move, talk and eventually breathe.
More than 80 per cent of people with MND will have communication difficulties, including for some, a complete loss of voice.
It affects people from all communities. Around 35 per cent of people with MND experience mild cognitive change, in other words, changes in thinking and behaviour.
A further 15 per cent of people show signs of frontotemporal dementia which results in more pronounced behavioural change. It kills a third of people within a year and more than half within two years of diagnosis.
A person’s lifetime risk of developing MND is around one in 300. Six people per day are diagnosed with MND in the UK. It affects up to 5,000 adults in the UK at any one time.
It kills six people per day in the UK, just under 2,200 per year.
It has no cure. Source: Motor Neurone Disease Association
COMMENT – JAYNE CONNERY, Care Campaign for the Vulnerable
Allan Sheppard walked into a hospital A&E department in 2015, collapsed with stomach pains and was soon diagnosed with motor neurone disease. If that was not heart breaking enough to both him and his family – three years later, they are now forced into an unwanted battle with authorities to grant him his wish of returning home to receive care for however long he has left.
Care Campaign for the Vulnerable is now contacted by more and more families and carers telling us the care sector grows a ‘invisible cloak’ and families voices are no longer heard.
It’s a lonely existence battling the care system.
Families contact us begging to highlight their ‘unfair’ treatment – knowing it’s at last a way of finally being listened to. I’ve been there on a personal level with my mum – hence my reason for setting up Care Campaign for the Vulnerable over five years ago – and the Sheppard family is no exception.
A loving dad stricken with motor neurone disease, still has mental capacity to make his own decisions and he’s made one he wants to go home to receive his care with his devoted daughter with a package of care available and not to a care home over 77 miles away from his family.
This should never be about what the system only deems to be ‘not sustainable’ in achieving.
His daughter and a nursing care agency is willing and able to offer a care package support to her father and Mr Sheppard wants to return home to continue his family life. The many shocking elements to this case are, I’m sad to say, not unusual.
Care Campaign for the Vulnerable receives cries for help every day from families and family carers telling us they feel they are ‘invisible’. Receiving good care is becoming more of a lottery.
This tragic case is not about what’s achievable or what’s deemed to be in the best interest of Mr Sheppard. Let’s face it, if that was really the case, Mr Sheppard would now be on his way back home into the care of his devoted daughter and a team of qualified care staff.
Family life should be what matters here and even more so with the Sheppard family.
Time spent with their dad at home is now against them, while wasting their precious time fighting to be heard.
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care (also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator, if you want to know how to get funding for our service or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
Also, check out our careers section here
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in Melbourne, Sunbury and in South Gippsland/Victoria.
We are an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia.
We have also been part of the Royal Melbourne health accelerator program for innovative health care companies last year!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update!







