Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients.
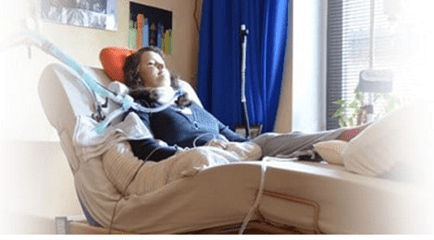
Can My Sister have BIPAP or CPAP Overnight via Tracheostomy?
Good morning, good afternoon, good evening, wherever you are. Welcome to another livestream today from Intensive Care at Home at intensivecareathome.com. But we also now incorporate questions today from intensivecarehotline.com.
Just to draw a quick distinction. With Intensive Care at Home, we provide Intensive Care at Home services for predominantly long-term ventilated adults and children with tracheostomies, but also home TPN, seizure management at home, as well as tracheostomy care as well as non-invasive ventilated adults and children at home. With intensivecarehotline.com, we provide consulting and advocacy for families in intensive care.
Now, before we go into today’s question, just a couple of things. You may wonder what makes me qualified to talk about today’s topic which is, “Can my sister have BIPAP (bilevel positive airway pressure) or CPAP (continuous positive airway pressure) overnight via tracheostomy?” Again, my name is Patrik Hutzel, founder of Intensive Care at Home and intensivecarehotline.com. I’m a critical care nurse by background. I have worked in intensive care/critical care for over 20 years in three different countries, and I have also worked as a nurse unit manager for over five years in intensive care.
We’ve been providing Intensive Care at Home services for the last 10 years, predominantly on the east coast of Australia, Melbourne, Sydney, Brisbane, but we are now also operating all around the country in Australia. And we bring a wealth of knowledge in this space to the market. We bring a wealth of knowledge and intellectual property to this space for Intensive Care at Home. With intensivecarehotline.com, we’ve been advocating and consulting families in intensive care all around the world for the last 10 years as well.
Now without further ado, let’s get into today’s topic, “Can my sister have BIPAP or CPAP overnight by a tracheostomy?” Please type your questions into the chat pad after we’ve gone through today’s questions. I will also open up the phone line so you can dial in live on the show with the questions, but let’s go through today’s questions first.
So, I had an email from a client this week where I thought, “Oh, this is a really good question because we get similar questions quite frequently.” So, I thought this is a really good topic to record in a video and put it on our blog so more people can learn and understand about what’s really happening in home care, but also in intensive care. Where’s the interface and how can patients be safely managed at home whilst having quality of life at home and also no longer block a bed in intensive care?
So, let me read out this email from the reader this week. “My sister was unable to tolerate to return to two liters nasal cannula and left on the tracheostomy collar, 35% humidified oxygen due to thick secretions and she was transferred to physical rehab from ICU.” So, for anyone that doesn’t know what a tracheostomy collar is that this lady is describing her sister that has been on a ventilator with a tracheostomy. She’s now weaned off the ventilator. She’s now having the tracheostomy and she’s still needing humidified 35% oxygen on the tracheostomy. Because when you’re bypassing breathing in through the nose, which is basically what you’re doing when you’re breathing with a tracheostomy, air doesn’t get humidified. When you’re breathing in through the nose, your air automatically and naturally gets humidified. So, because you’re bypassing the nose when having a tracheostomy, air needs to be humidified so that secretions are not drying up, so that the lungs don’t get blocked, but also so that the tracheostomy doesn’t get blocked with thick, dry secretions.
“After four days of rehabilitation, she was returned back to ICU due to elevated CO2.” CO2 is carbon dioxide level. “And now she’s back on the ventilator. My sister wore a CPAP machine at home at night prior to respiratory arresting on the 30th of December. And through her recovery, no one put her back on BIPAP in ICU. My thinking is her CO2 level has been slowly increasing since they’ve removed her from the CPAP/BIPAP.” Now she’s talking about BIPAP as well. “And then the vapotherm and switched her straight to the tracheostomy collar right before the transfer from ICU to the physical therapy center.” It looks to me like critical steps have been missed here straight away where I’d say, most likely this lady should have had a sleep study before even going on the tracheostomy collar, or she should have had at least some arterial blood gases to make sure that her going from the ventilator to the tracheostomy without mechanical ventilation was the right thing to do. And it looks to me like a critical step has been missed there.
So, then she goes on and says, this lady, her name is Ellen, by the way, “My sister has COPD (Chronic obstructive pulmonary disease) and her oxygen have been two liters for about seven years prior to her event on the 30th of December. So, the question that I have is, can she use CPAP or BIPAP via tracheostomy just at night? Her oxygen saturations are fine during the day. She’s eating and speaking and tolerating physical therapy or physiotherapy. Why can’t she just use the CPAP or BIPAP at night to prevent hypercapnia caused by hyperventilation during the sleep?”
Well, you are asking a very good question here, Ellen, and you’re asking the right question. Absolutely, she can definitely use CPAP and BIPAP via the tracheostomy at night and she can do that in the comfort of her own home with our service at Intensive Care at Home. When you look at the mechanical home ventilation guidelines, and I should say, the evidence-based mechanical home ventilation guidelines, you will find that anyone on a ventilator can go home that’s medically stable with a tracheostomy or non-invasively ventilated if they’re looked after by intensive care trained nurses with a minimum of two years ICU/pediatric ICU experience, and that’s exactly what we’re offering here at Intensive Care at Home.
Now, Ellen further says, “My sister caught the flu, and this led to an exacerbation of her COPD. Unfortunately, she had a respiratory arrest and was in VT.” Ventricular tachycardia. That’s what it stands for… “but was resuscitated with one shock on the defibrillator and placed on a ventilator. In February, she was still not off the ventilator, and they were trying to “wean her off” the ventilator. Then on Tuesday, she was transferred to physical therapy rehab off all mechanical assistance and just on the tracheostomy collar 35% of oxygen. But then she’s back in ICU on a ventilator due to hypercapnia. I am unclear of why she wasn’t given pressure support at night, CPAP, or two levels of pressure support, BIPAP, which she had been using prior to December the 30th event. That’s my question. Tracheostomy, CPAP, end goal is getting her home. Is this doable?”
Yes, absolutely. Absolutely, it’s doable. A lot of our clients at home are in similar positions, whether they’re ventilated because of COPD/asthma, or whether they’re ventilated because of a spinal injury, motor neuron disease, cerebral palsy, you name it. Whether they’re ventilated because of a low oxygen level, respiratory failure type one or whether they’re ventilated because of type two respiratory failure, which is high CO2. In your sister’s case, it’s a high CO2 level type two.
So, it also looks to me like your sister was rushed out of ICU without taking small, measured steps. They took her off the ventilator and one day later, she’s in a rehab facility. That’s just simply dangerous and it’s screaming, “Send me back to ICU.” That patient in ICU should be off the ventilator, especially a long-term ventilated patient, which sounds like your sister is a long-term ventilated patient. (A) She has a history of high CO2 and hypercapnia. And now, she’s obviously with the respiratory arrest faced with a situation where she is long-term ventilated with a tracheostomy. So clearly, the next step is for her to go home.
It looks like she’s otherwise medically stable. You’re not talking about that she’s on any vasopressors on any inotropes. You’re not talking about that your sister is sedated. You’re not talking about that your sister is on a dialysis machine or needing TPN (Total parenteral Nutrition). But even so, she could go home with Intensive Care at Home as well.
So clearly, what needs to happen here, Ellen, is you should contact us at intensivecareathome.com and we can walk you through the steps including what funding to get for your sister and then set up a home care for her. It’s really that simple. We, of course, need to find the right nursing staff for her, but once we’ve done that, then it’s all green light from going forward.
Now, here is another thing. Again, if you look at the evidence-based mechanical home ventilation guidelines on our website, intensivecareathome.com, again, you will see that anyone with a tracheostomy or with a ventilator, either/or a combination of both, needs to be looked after, 24 hours a day, with a critical care nurse with a minimum of two years ICU or pediatric ICU nursing experience, because you can’t just send anyone looking after a tracheostomy.
Now, the reason I’m saying that is we’ve had clients at home where we were doing night shifts only because there was no funding for day shifts and those clients were either ventilated, or had a tracheostomy or a combination of both, and those clients passed away during the day because medical emergencies with the tracheostomy could not be managed by family members, support workers. And tragically, two children at the time died even though we were warning families, we were warning the funding body that this is most likely happening, because the service provision around evidence-based and best care was not met.
Again, I point you back towards our website at intensivecareathome.com, look at the section, mechanical home ventilation guidelines. The quality standards in the community that we adhere to. The quality standards in the community that we base our service provision on, i.e., we exclusively employ and hire ICU nurses with a minimum of two years ICU/PICU experience. And with that in mind, we are employing hundreds of years of ICU and pediatric ICU experience in the community. I don’t think that can be matched by any other service provider. So, I hope, Ellen, that answers your question. And your sister could also have physical therapy at home, we can help with all of that. Maybe the recovery needs to take place at home, because when she went into the rehabilitation center, it doesn’t look to me like they knew what they were doing. Again, this is why I’m saying, often in those places there are no ICU/PICU nurses. I’m not surprised that those patients bounce back pretty quickly unless people know what they’re doing.
So, I would be very curious as the next step. Has your sister had an arterial blood gas? Has she potentially had a sleep apnea? Does she need a sleep apnea? Do her ventilator settings need to be changed? Does she also now need to go from CPAP to BIPAP depending on her respiratory status? Because BIPAP gives her two levels of pressure, not only one level of pressure, the pressure support. It’s two levels of pressure support. I think it’s a very valid question you should ask to the respiratory team and map out the next steps. But either way, I do believe she’ll be safest to be at home and we can help with the weaning process at home. So, just contact us at intensivecareathome.com even if you are in the United States, because in the United States now we have a clinical liaison nurse that can help us with setting you up with other providers.
And if you are a provider who believes you can provide Intensive Care at Home services in the U.S., we definitely want to hear from you. Again, go to intensivecareathome.com. Either send us an email to [email protected] or just give us a call on our U.S. number on the website.
For our audience in the U.K., similar, we can help you with Intensive Care at Home in the U.K. We do know of a provider there that can help you as well. Again, send us an email to [email protected] or call us on our U.K. number on the top of our website.
Okay, I hope that helps Ellen with the next steps.
Let’s look at other questions, “Hi, my dad is in ICU for nine days and they took him off sedation four days ago, but he’s still on a ventilator. He’s 75 years of age and has kidney impairment. He opens his eyes when we call him and he’s able to move his head but can’t move the rest of his body. We can’t seem to get a definitive answer as to why this is happening. Would you be able to help, please? Also, my dad has a buildup of fluids. They’re doing physiotherapy in the bed as they can’t take him out because he has high blood pressure. They said he’s all off sedatives, but the nurse said she gives him 200 milligrams of fentanyl when they have to move him. Would this be the reason as to why he’s not responding?” They wouldn’t be giving him 200 milligrams of fentanyl, it would be 200 micrograms of fentanyl, but either way.
So, “Dad in ICU nine days. They took him off sedation four days ago. He’s kidney impairment. He opens his eyes when we call him. He is able to move his head but can’t move the rest of his body. We can’t seem to get a definitive answer as to why this is happening. Would you be able to help?” Look, it’s very difficult to put timeframes on when someone will wake up after an induced coma, very difficult. Is the fentanyl stopping him from waking up? It really depends how often is he getting the fentanyl? Is he getting it once a day? Is he getting it twice a day? Is he getting it four times a day? It depends a little bit on that. You have not shared why your dad is in ICU, so it would be very advantageous to know why your dad is in ICU. For example, God forbid, if your dad is having a brain injury, it might take him longer to wake up anyways, but you’re not mentioning anything like that.
Other question is, what sedatives has he been on? What opiates has he been on? I think we can confidently say the opiate is fentanyl, but what sedatives has he been on? Has he been on propofol? If he has been on propofol, which is a short-term acting sedative, he should wake up reasonably quickly. If he has been on midazolam or Versed, it’s a long-term acting sedative and it might take him longer to wake up.
Now, you are talking about that your dad has kidney impairment and that might really stop him from waking up as well, because some of the sedatives and opiates might not be washed out yet. So, I hope that helps. And again, be patient here and also bear in mind if your dad has a brain injury or has he had a stroke, God forbid, have they done a CT scan of the brain? Other than that, I would just say wait, be patient, physical therapy will help, and then go from there. So, I hope that helps.
Then let’s move on to the next question, and this is a bit of a mixture of a question, but also on a bit of a testimonial where we helped a family couple of weeks ago as part of our consulting advocacy. An email from Lisa.
“Hi Patrik, I hope you’re well. Thank you again for the support you’ve given our family through this difficult time. I can’t imagine how busy you are yet to take the time to personally respond to people’s questions and offer hope in their time of need. That’s what you’ve done for our family. We would’ve given up and given over control of my brother if you hadn’t been willing to educate us about our situation.
It was midnight for you when we had our family meeting, but you stayed on the call with us for almost three hours. I believe the advice you gave us saved my brother’s life. The ICU staff knew they were going to be held accountable, and after that meeting, things improved for my brother. You truly have found your calling. The world would be a better place if there were more people like you.
I wanted to give an update on my brother’s condition. They’ve moved him to acute care within the hospital, so he’s no longer in ICU. We are really pushing the hospital to work with him on the swallowing test so he can have his tracheostomy removed.” And update here. I know that the brother had his tracheostomy removed by now, which is really amazing.
“They’re telling us that he can probably stay another week before they’re going to push him out, so to speak. We’ve continued to hold off on the PEG (Percutaneous Endoscopic Gastrostomy) tube because we are seeing a lot of progress and we hope that he’ll be eating very soon. We just think it’s too soon to agree to a PEG and we would only really do that if he can’t eat beyond a shadow of a doubt.
The hospital case worker told us that the insurance will stop paying when the hospital says there’s nothing more they can do, which according to her is going to be in less than a week. So, she’s trying to force us to do the PEG. We are trying to find the short-term rehabilitation that will not require the PEG, but it’s tough.
We’ve researched exercises to do with our brother to improve his swallowing muscles. My sister and I will be at the hospital every day this week working with him. We can’t trust the hospital to do it. I spoke with your clinical liaison, Nurse Tara, and she’s going to be touching base with me in a few days to see where we’re at as far as my brother’s progress and needs are concerned for home care.
Is there anything else we can do or say to try to extend his time in the hospital for just another week or two? Is it reasonable for us to ask that? Every day my brother is improving, but the hospital is still recommending a PEG tube and a skilled nursing facility. Please let me know if there’s anything else we need to do or know.
Thank you again from the bottom of my heart for all of your help. God bless you for your service.
From Lisa.”
Okay, Lisa, I have sent you an email in regard to that, but I also want to quickly bring it up for our viewers here because I know that many people are in a similar situation. And so, here’s the situation. This gentleman had, I believe, a brain tumor and then ended up in ICU, didn’t wake up. Took him a long time to wake up, needed a tracheostomy. Eventually he woke up, they took him off the ventilator. He was coming around, and now simply he’s not swallowing yet, and he’s still fed through a nasogastric tube. He’s tolerating the nasogastric tube; he’s not pulling it out. So, he failed one swallow test, so what? Maybe they can have a second attempt at that and then they can avoid the PEG.
The PEG is not a great thing. I do believe PEGs have their time and their place for patients who, without the shadow for doubt, will never eat again. But that’s not the case with Lisa’s brother, I believe, because he’s already awake and maybe a few more weeks, then he could start eating and drinking again, even only small amounts because he’s made so much progress in the last week or so, we are positive that he can eat and drink very soon. “Now, what can you say in terms of the insurance?” My advice there always is, if the insurance doesn’t come to you directly, can you trust what the hospital says? I don’t know. I’m not saying what the hospital is saying is not accurate, but please keep in mind that the hospital may or may not have the right information for you.
And as I said, if you haven’t heard from the health insurance, do not worry about it. Do not worry about it. Get it from the horse’s mouth, so to speak, and only then take action. My experience is after having consulted probably hundreds, if not thousands of families in intensive care over the years, as long if you don’t hear from the health insurance, I wouldn’t worry too much about it. I hope that helps. And thanks again, Lisa, for your kind words as well.
So, let’s move on to the next question, and then also just quickly come in with just, yes, that’s also a question we get quite frequently. “Do rehabilitation places take patients without PEG tube and only a nasogastric tube?” Some of them do, some of them don’t. Most do want the PEG tube. But here is the problem that I have with PEG tube particularly. I believe that a PEG tube gives the perception that a person will never eat again, and some might dispute that, but my experience is the PEG gives a perception that people will never eat and drink again, so people stop trying to even get people to eat and drink again. And that’s not good. It’s not serving people’s quality of life. A PEG can make hospital staff complacent by knowing, “Oh, I’ve got a feeding tube, all I need to do is just feed. I don’t need to worry about getting a person to eat and drink again.” Think about that.
Let’s move on to the next question. Here is a quick email or a frustration we had from a reader this week who says, “Fluid overload without diuresis. My wife is significantly swollen in ICU and not outputting urine at a rate to keep up with the IV fluids. What is the solution?” Well in ICU, when patients are fluid overloaded, especially when they’re ventilated, that could impact on not weaning patients off the ventilator because if you have too many fluids on the lungs, you might struggle with weaning off the ventilator.
Now, if diuresis like furosemide, Lasix, or spironolactone is not working, then the next step often is to start hemofiltration or dialysis, that can be the solution here. Now, what can happen there is as a number of risks there if fluids are removed too quickly, blood pressure might drop, electrolytes like potassium, magnesium might drop down too quickly. You got to chase electrolytes, you sometimes have to start inotropes or vasopressors if blood pressure goes too low too quickly. Those are things that need to be considered. But I hope that answers your question that the next step here might be hemofiltration or dialysis.
Also, a fluid restriction might help, but your wife might simply need fluids for her condition. Maybe she’s also still a little bit hypovolemic, she was dehydrated beforehand, maybe her sodium is a little bit on the high side. I don’t know the ins and outs. You haven’t shared that with me. So, just to give you some insights there.
Then, next question. So, this is a comment actually that we had from a client for one of our videos on YouTube or for one of my videos on YouTube where she says, “Justine, I’m so sorry for the loss of your son. I lost my live-in boyfriend of 15 years on February the 7th, 2023 after 2.5 weeks in ICU. Because the ICU doctors fed his family the doom and gloom narrative, they shut him off and watched him die “peacefully”. He could have had some bio, he just needed time. Now the family is torn, and my love is gone forever. ICU is a nightmare.” I’m very sorry, and this is actually from Jolene. I’m very sorry, Jolene, to hear about the loss of your boyfriend. It’s very, very sad to hear.
Well, I’ve made countless videos about the doom and gloom narrative in ICU, and I keep coming back to that 90% of intensive care patients approximately survived. The numbers vary a little bit, but overall, 90% of intensive care patients survive. So, if they’ve been fed the doom and gloom narrative and they’ve bought into it, the ICU team might have stopped treatment and your boyfriend might have passed away. But the best way to find out what’s really happened without jumping to any conclusions is to look at medical records. We would need to do a medical record review to find out what’s really happened. That’s the only advice I can give you there.
With a doom and gloom for family or anyone watching this that has a family member in intensive care, do not buy into the doom and gloom narrative because it doesn’t work for you. Most patients in intensive care survive and you should question everything that the intensive care team is telling you.
Now, let’s get on to the next question before we wrap this up. “Hi Patrik, my dad has passed away from COVID. He also has other health ailments like diabetes and bad kidneys. He was talking for about eight days, and after dialysis, he went into a coma and never woke up. He did have some movements like moving his mouth and he opened his eyes once, but that was it. The doctor also mentioned that he had multiple organ failure. Is it normal to go into a coma after dialysis? Can multiple organ failure cause a person not to no longer wake up?” So, let’s read that again. “My dad has passed away from COVID. He also has other health ailments like diabetes and bad kidneys. He was talking for about eight days, and after dialysis, he went into a coma and never woke up. He did have some movements like moving his mouth and he opened his eyes once, but that was it. The doctor also mentioned that he had multiple organ failures in order to go into a coma after dialysis. Can multiple organ failure cause a person to no longer wake up?”
Yes, multi organ failure can definitely lead to patients going into a natural or into an induced coma and not wake up. Will dialysis in and of itself lead to a coma? No, not at all. There are patients in ICU that might be on dialysis that are awake, so that’s not the issue. It sounds to me like this is very sad what’s happened here, and I believe it’s very important for you that you get closure. And again, the biggest challenge for families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care. Again, this is exactly what you’re dealing with here.
It sounds to me this took you off guard, it sounds to me like you had no idea what was happening, and now it sounds to me like you are debriefing and you’re potentially traumatized from this experience. And the only way I believe we can shed light on this is to get access to the medical records and help you with the medical record review to see exactly what’s happening. What was the cause of death? Was it COVID? Was it another organ failing? Was it multi-organ failure? And so forth.
And we have legal nurse consultants on our team that can do medical record reviews, we also have a team that can help you at Intensive Care at Home with NDIS (National Disability Insurance Scheme) nursing assessments. Or if you are a funding body or another provider and you need nursing assessments for NDIS, we can help you with that as well. We have a team working on that.
But coming back to intensivecareathome.com, again, especially if you are in Australia and you need home care for Intensive Care at Home, if your loved one is long-term in ICU, long-term ventilated tracheostomy, long-term ventilated BIPAP, CPAP, home TPN, seizure management, anything that’s medically complex that needs an intensive care nurse at home, we can help you with that and we can help you with funding as well.
We are TAC (Transport Accident Commission) approved provider in Victoria. We are an iCare approved provider in Queensland. We are an NDIS approved provider all around Australia, and we are a DVA (Department of Veteran Affairs) approved provider all around Australia. And we obviously have third party accreditation for Intensive Care at Home and we employ hundreds of years of intensive care nursing experience. We’re working with doctors very closely to make Intensive Care at Home safe.
So, I do want to wrap this up today. I don’t have as much time as on other days.
Thank you so much for watching.
Now, if you have a loved one in intensive care and you are looking for home care, you should go to intensivecareathome.com and contact us there on one of the numbers on the top of our website, or simply send us an email to [email protected].
If you have a loved one in intensive care and you’re looking for advice, and you have a lot of questions and you don’t know where to start, please contact us at intensivecarehotline.com. Call us on one of the numbers on the top of our website or simply send us an email to [email protected].
Also, have a look at our membership for families in intensive care at intensivecaresupport.org. There, you have access to me and my team, 24 hours a day, in a membership area and via email.
Also, if you need a medical record review or if you need an NDIS nursing assessment, you should contact us as well and we can help you with that. Also, we review medical records for families in intensive care in real time or after intensive care, but we strongly recommend to have medical records reviewed in real time so you can have a really good understanding of what’s happening in real time. And for NDIS nursing assessment, please contact us as well.
Now, thank you so much for watching.
Please subscribe to my YouTube channel for regular updates for families in intensive care, for YouTube live streams where you can get your questions answered on a live stream, share the video with your friends and families, anyone that would benefit from this video, click the like button, click the notification bell and comment below what questions and insights you have from this video or comment on any topic you want me to make a video about.
Thank you so much for watching.
This is Patrik Hutzel from intensivecareathome.com and I will talk to you in a few days.
Take care.









