Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients and the question today is
Can my Mother Be Weaned Off the Ventilator and Tracheostomy at Home? Live Stream!
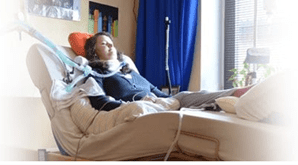
Intensive Care at Home and Intensive Care Hotline, I want to welcome you to today’s livestream, good morning, good evening, good afternoon wherever you are.
Today’s livestream is about, can my mother be weaned off the ventilator and tracheostomy at home? That is today’s topic and that’s what I want to focus on today.
I want to give you some examples and want to answer that question. So, hopefully, there’s no more ambiguity for you and your family going forward what you should be doing next if you find that your mother, or your father, or your spouse, or your brother, or your sister, your child, is in intensive care. And I want to focus on the children as well.
So, before I dive into today’s topic, I want to just quickly introduce myself and also want to talk about what makes me qualified talking about this topic. You might be wondering, well, what makes this guy qualified to talk about this topic?
So, again, my name is Patrik Hutzel, I’m the founder of Intensive Care at Home and also Intensive Care Hotline. I am a critical care nurse by background, I have worked in critical care/intensive care for over 20 years in three different countries.
Out of those over 20 years in ICU, I’ve worked for over five years as a nurse unit manager in intensive care. I’ve also worked with intensive care at home, and I’ve founded Intensive Care at Home here in Melbourne, Australia, in 2012, and we’ve been running Intensive Care at Home ever since then.
So, that’s a little bit about me and my background. I’ve also consulted and counselled and advocated for families in intensive care all over the world through Intensive Care Hotline. And again, that’s been happening for the last nine years now.
So, let’s focus on today’s topic, Can my mother be weaned off the ventilator and tracheostomy at home instead of intensive care? And again, I could replace can my mother, can my father, can my spouse, can my brother, can my child, grandmother, grandfather, you can replace that with any family relation really. Can they be weaned off at home instead of intensive care? That’s a great question to ask.
Now, like with anything medical, it’s very rarely clear cut. The short answer to that question is that it depends, some people can, some people can’t. It also depends on where is your loved one in the weaning process? For example, if your loved one has been in intensive care for three months on a ventilator with the tracheostomy, has had multiple failed weaning attempts.
And if we look at the case and we think, well, they just need another week, and then they can be off the ventilator and then have the tracheostomy removed, it’s probably more complicated to go home rather than wait another a week or so.
So, it is really important that you choose the right path for your loved one in where they’re at. Whilst we are all for home care, you don’t want to be going into a home care situation with Intensive Care at Home if you only have limited time that your loved one needs to get off that ventilator, so there’s really no point in going home because setting up Intensive Care at Home is doable, but it’s also complex.
And I come to that a bit later, that you don’t want to choose Intensive Care at Home just for the sake of it because it sounds good. You got to look at the logistics, you got to look at the safety aspect, you got to look at where you want to go in the long run because you got to keep in mind, Intensive Care at Home, you do need to replicate what’s happening in intensive care at home. And whilst we’ve done it many times successfully, it takes a little bit of time to set up.
Therefore, you can’t just rush into it because you’re desperate to get out of hospital. I get it that you’re desperate to get out of hospital, it’s very frustrating, I understand all of that, but safety is paramount and you can’t be going home without the right support structure in place. So, that it’s absolutely safe for your loved one to leave intensive care and replicate intensive care in the home, which is what needs to happen to make this safe.
So, when would I be recommending for someone to go home on a ventilator with a tracheostomy so that they can be weaned at home? So, one of the prime examples that I would like to take here is really Guillain-Barre syndrome. Guillain-Barre syndrome is a neuromuscular disease where people pretty much have can’t move anymore, and that obviously includes the breathing muscles.
Many of those Guillain-Barre patients end up in ICU being partially paralyzed, at least for a while, end up on a ventilator, end up with a tracheostomy, end up with often immunoglobulin therapy, which often helps. And then, once the therapy is kicking in, they need to very slowly start to learn, to move again, start to learn, to move their arms, move their legs, get mobilized, starting to eat and drink again. It’s a very arduous and slow process, which I actually believe can be speeded up at home rather than in a depressing intensive care environment.
And those Guillain-Barre patients in particular, stay in ICU for a very long time, if no one’s coming to the rescue to take them home, so to speak. So, that is a prime example to take a long-term patient home and wean them off at home.
Very few Guillain-Barre patients stay with the tracheostomy and ventilation for the rest of their lives. Some of them really do recover and they recover well. So, that’s just one example where, going home is a very good next step. Hi, Modema, nice to see you again.
Another case study, if you will, where you can go home and wean ventilation and tracheostomy at home, is for example, children. So, and I’m even talking about the very young ones, I’m talking about premature babies. For example, we’ve had some situations where we weaned a couple of children off the tracheostomy at home, and they’re now hopefully living normal lives. It was a very joyful experience helping those kids to transition from ventilation, to tracheostomy, to home. And now, they’re decannulated and hopefully, they’re progressing well in their lives. Very enjoyable experience.
So, the case studies are there where someone can go home and be weaned off the ventilator at home, definitely doable, but it’s a little bit of right place, right time. And again, as I was saying right in the beginning, you don’t want to be going home on a ventilator with a tracheostomy if your loved one needs another week in ICU to get off that ventilator and get off the tracheostomy, there’s no point in setting up home care with Intensive Care at Home.
Simply, you need a team of 24/7 intensive care nurses, whilst that can all be set up. It’s more something that will be set up for the long term, not so much for the short term. You also want a stable team, you don’t want to have people coming and going.
So, if it can be approached from a long term perspective, you will get more stability and also more safety because unfortunately, if you don’t have 24 hours intensive care nurses at home, for someone on a ventilator with a tracheostomy especially if you want to wean them, it’s a recipe for disaster, absolute recipe for disaster.
Unfortunately, we’ve seen clients pass away where we were only doing night shifts and there was no day shift for a ventilated and tracheostomy patient. And we have seen some tragic cases. So, I’m not making this up, I’m talking from experience.
So, the first step really, the first determination you should be making is, if my loved one can’t come off the ventilator in ICU within a reasonable amount of time, that is the time when you should be thinking about going home, that’s the time when you should be starting to talk to people, how can it be set up.
Again, if you are in Australia in particular, you should be reaching out to us at Intensive Care at Home, you should be reaching out to us if you’re in America too, but you should be reaching out to us one way or another, we can help you, guide you, step by step. We can help you guide with funding, who’s going to pay for it. Please, again, bear in mind that people might tell you, “Oh, no one’s going to pay for this,” and that’s a whole lot of nonsense. We wouldn’t be in business if no one would be paying for it.
Many people have an active interest in paying for Intensive Care at Home because it cuts the cost of an intensive care bed by around 50%, and it frees up an in-demand ICU bed. ICU beds were in high demand before COVID, you probably have an inclination that the demand of ICU beds during COVID has even become higher. So, you can see that people actually have an interest in freeing up ICU beds and getting people home because it creates a win-win situation for everyone, right?
So, but the right timing is critical. Also, if you do think about getting your loved one home on a ventilator, they need to be, generally speaking, liberated from other mechanisms of life support. They need to be off inotropes, off vasopressors, and that is if they’re liberated from all other mechanisms of life support and if you then know that your loved one can’t be weaned off the ventilator within a few weeks or a few months, that is the time when you should be considering going home.
Again, you should be contacting us, we should then be looking at funding sources, who will pay for this? There’s definitely someone paying for this, no question about this, you shouldn’t worry about it. It all comes down to talking to the right people. It all comes down to the right advocacy. Now, with the NDIS, the National Disability Insurance Scheme here in Australia, a lot of doors have opened through that scheme to pay for services like Intensive Care at Home and go from there.
Now, there are many other situations, and I’ve made other livestreams and videos about this where people go home and they’re not going home with a goal of weaning. We are specifically talking today with the goal of weaning someone off the ventilator, because there are many other clients that do go home on a ventilator with a tracheostomy, but they can’t be weaned. They can’t be weaned, for example, take a C1 spinal injury patient, MND (Motor Neurone Disease), those patients, unfortunately, can’t be weaned and therefore, it’s more like the long-term nursing care with the goals of focusing on quality of life day by day, quality of life, focusing and spending time with family. Whereas if you go home to wean someone off the ventilator, the goal is to wean them off the ventilator and liberate them as quickly as possible.
So, once you’ve determined or we’ve determined with you, should they be going home, then we can look at the funding source, then we can look at the team. We need to look at your location, of course, the closer to a metropolitan area, generally speaking, the better it is to set up staffing and find staffing because if you are in a rural area or regional area, it’s much more difficult to find staff, because most ICU nurses are mainly in the metropolitan areas and not so much in rural areas. So, keep that in mind.
That’s not to say that it can’t be done in a regional or a rural area, but it’s going to be more difficult to set up, it’s going to be more expensive. You want to keep that in mind when it comes to setting up Intensive Care at Home.
Next, so, the funding bodies, again, should be having an interest in getting your loved one out of ICU, cutting cost by around 50%. The ICU should have an interest in getting your loved one home, freeing up an ICU bed. Again, this is a win-win situation for everyone.
You need to make sure there’s 24-hour intensive care nursing at home, you need to make sure there’s someone overseeing the medical care. And again, we can help you with setting that up. You need to make sure there’s allied health professionals, for example, that there’s a physiotherapists, a physical therapists, an OT, an occupational therapists, speech therapists. So, you need a whole team to pull this off really. Okay.
But again, it can be done. Once you’re at home, once you’ve got 24-hour intensive care nursing with us here at Intensive Care at Home, with our ICU nurses, the next step is to then look at a weaning plan. So, what does a weaning plan look like? A weaning plan looks like that every day, you’re taking measured steps to be weaning someone off a ventilator.
So, what does that look like? It looks like, for example, taking someone off a ventilator at 10:00 in the morning for an hour. It might even look like taking someone off a ventilator for 10 minutes at 10:00 in the morning, and then maybe another 10 minutes to 2:00 in the afternoon, and then maybe another 10 minutes at 6:00 in the afternoon, and then rest overnight. And then the next day, you do 15 minutes at the same time. And the next day you do 20 minutes.
It can be a very slow process, but you got to start somewhere. Some people develop quicker than others, what is very important that if you do wean at home on a ventilator, mobilization is key. Mobilization is absolute key. You need to combine taking someone off the ventilator with mobilization. Imagine you’re lying in bed all day, you cannot strengthen your breathing muscles, it’s very difficult. Whereas if sitting up, your upper body will automatically strengthen because you got to sit up, that’s one step.
And the next step is then to do breathing exercises, for example. A good ICU nurse can do that, a good ICU physiotherapist or physical therapist can do it. For our American friends, you might have a respiratory therapist involved, but a good ICU nurse knows what to do when it comes to weaning. And it is also directed by the medical team, of course, but most ICU nurses know what to do, not the first time they’re weaning.
Nutrition needs to be optimized. Physical exercise needs to be optimized, again, with a physiotherapist or a physical therapist. So, equipment needs to be optimized such as you need a recliner chair, you need a hoist machine, or lifting machine so you can actually get someone mobilized.
But just picture this, your loved one being weaned at home in a loving, caring family environment, as opposed to weaning in ICU where it’s noisy, it’s loud, people are running around 24 hours a day, where patients have a disturbed day and night rhythm, you can see the benefits of home care straight away.
Some of you that have done your research a bit more closely, you might say, well, how can this be done at home without arterial blood gases? Most patients would go home without an arterial line, yeah, that is correct, but you can do capillary gases. There are ways of monitoring CO2 (carbon dioxide) also through a CO2 capnograph, through the monitor. So, there’s a variety of ways how to monitor vital parameters every day, so you can measure progress. Very important to measure progress every day.
Now, some of you might ask straight away, how long does it take? Well, that is difficult to say. Depending on the underlying condition, as I mentioned a minute ago, Guillain-Barre can take a long time, also, because of other therapy that needs to happen at the same time. With immunoglobulin therapy, which can be given at home as well, by the way, there’s no need to do that in hospital.
And just coming back quickly to Guillain-Barre syndrome patients weaning at home, the number of Guillain-Barre patients I’ve seen in ICU staying there for six or nine months and being depressed, being depressed. And imagine now, where you still have some ICUs in lockdown, where you still have some ICUs limiting the number of visitors, if they allow visitors at all, imagine your loved one stuck in ICU long-term, whether it’s with Guillain-Barre syndrome or anything else, and you can’t visit them, that’s just terrible. That’s just terrible. And thank God there is an alternative for that, thank God there is Intensive Care at Home, and thank God you don’t need to be bowing down to intensive care teams if you don’t like what you’re seeing there.
Now, breaking down the weaning process in a little bit more detail. So, for example, you need a written weaning plan from the intensive care team, or from the respiratory therapist, or from the respiratory physician, so you can put this care plan into place when your loved one is going home.
Again, with measurable goal, clearly defined goals, today we are doing two hours off the ventilator, if that can be tolerated, maybe the next day we extend that to two and a half hours, maybe we extend it to three hours, maybe we double it, who knows? Depends a little bit on the individual and the condition.
It’s a little bit harder with children because depending on how old the children are, can they follow instructions? Some of those kids can follow instructions, others may not be quite there yet. But then again, children, generally speaking, develop in terms of they are growing, they’re getting stronger, that’s a natural progression of children. Whereas with adults, if you don’t treat them well and if you don’t train them, if you don’t exercise them, they’re going backwards, and then you have to start from scratch again. So, to a degree, that’s much easier with children.
Now, here is another thing that needs to happen when someone is going home for ventilator weaning. Now, you might have heard me say in some of my other videos or blog posts that I’m opposing a PEG tube, especially again, for our American friends, when it comes to LTAC and people going to LTAC for home care, for ventilation, weaning, and home care, I absolutely advocate for a PEG tube, because that is the safest option when someone is going home to have a PEG tube, because if the nasogastric tube fell out, it has to be reinserted, it often needs a chest x-ray, so there’s risks attached.
For going home, I would advocate for a PEG. It doesn’t have to be permanent. It shouldn’t be permanent. But in terms of client safety or clinical safety, a PEG tube is the best option for nutrition until your loved one can hopefully eat and drink again. Okay.
So, moving along, what do you need in terms of skills? So, when someone is going home, do we wean off the ventilator and tracheostomy? As I said, you need a team of intensive care nurses, you also need a medical team overseeing it, but the work can be done by intensive care nurses at home, which you can get through us, Intensive Care at Home.
The doctors need to oversee it, but depending on how much research you’ve done, we exclusively work with ICU nurses with the minimum of two years ICU nursing experience. And those people have the experience of weaning patients off the ventilator in ICU, so they can help your loved one going from A to B.
So, very important to look at the quality of staff you’re getting. You don’t want to be working with someone at home that doesn’t hire intensive care nurses, it’s a recipe for disaster and potentially a recipe for death. As I alluded to earlier, some of our clients have passed away at home because we were only funded for night shift and there was no ICU nurses during the day.
And people have passed away because family members, disability support workers, or even general RNs, couldn’t manage medical emergencies for clients at home with a ventilator and a tracheostomy. It’s a tragedy beyond words what happened there, and I need you to be aware of what safety aspects you need to have in place before going home.
Now, then also, I just want to quickly mention, there is the exception to the rule. Patients like for example, C1 spinal injury, C2 spinal injury, MND (motor neurone disease), chances that those people can be weaned off a ventilator at home are pretty slim to null. The Guillain-Barre, it’s also a case of focusing on patients such as, if they have, for example, rib fractures and they’ve been intubated for a while and they’ve had an hemothorax and pneumothorax and so forth, and they’re just a bit slow to wean off, that could be another reason or another clinical condition where your loved one could go home to have the weaning done at home.
And again, very important that you’ve got the right team, and that can take a little bit of time to get the right team together. There’s sometimes a little bit of trial and error. Some people might come to your loved one where you feel a little bit uneasy and either we have to fine-tune their approach. Or you just have to give it a little bit more time until you warm up with some people, but it can be a little bit uncomfortable especially in the beginning, to find the right people for your loved one, so you got to be a little bit patient there until the staff have adjusted and you have adjusted to the staff.
In terms of cost, again, an ICU bed costs probably now around $6,000 per bed day within 24 hours, whereas Intensive Care at Home is probably half of that cost, and the ICU has a bed that’s vacant for more critically ill patients. So it’s a win-win situation over all.
And also, again, for our American friends, weaning at home is a much more desirable option than going to LTAC. I mean, I’ve spoken about LTAC and their deficiencies at length. So, I don’t want to go into detail now, you can type into Google, Intensive Care hotline, and LTAC, you’ll get a ton of information why we are strictly advising against LTAC, and go from there.
So, I really try to condense that today to, (A) so you can see what’s possible, (B) what needs to happen. We talked, not a great detail about equipment. I have again, made videos about equipment for Intensive Care at Home. But you need two ventilators, you need two suction machines, you need two monitors, you need a special care bed, you need a hoist, whether it’s a ceiling hoist or portable hoist, you need nebulizer machines, you need spare tracheostomies, you need tracheostomy dilators, you need resuscitation bags. That’s just in a nutshell to keep your loved one safe at home.
Now, I do want to open up the floor for any questions that you may have. It can be to the topic, and now I’m also happy to answer questions that are not to the topic today. So, shoot away with your questions, type them into the chat pad and I’m looking forward to answering them.
And while I’m waiting for your questions, yes, I should quickly talk about allied health. What does allied health mean? Allied health means health professionals such as physiotherapists or physical therapists such as occupational therapists, such as speech therapists.
Now, especially around physiotherapists or physical therapists, they need to have ICU experience, they need to have the experience where they wean someone off the ventilator. So, they know what to do on a ventilator, they know how to mobilize a patient, what body parts to focus on, how to strengthen their breathing muscles.
Is critically important and that you get someone there that is experienced in that area. We can help you with finding one too, but I can’t stress enough that especially a physical therapist or a physiotherapist is critically important to have at home. They can also advise, for example, would cough assist be beneficial in the weaning process? They’re the experts on that. So, there are many very good reasons why you need a highly proficient physiotherapist or physical therapist for weaning someone off the ventilator and tracheostomy at home.
And once again, going home is the much better option than LTAC for our American friends. If you are in Australia or in the UK, there’s no reason why you can’t go home from ICU directly. There are no LTACs, thank God for that. And that would be my advice.
If there are no questions today, which is a bit unusual, but maybe there are none today, that’s absolutely fine. Then I just want to thank you for your support, and I want to thank you for coming onto these livestreams and I’ll see you again next Sunday at 10:30 AM Sydney Melbourne time. I believe it will be 8:30 PM Eastern time, 7:30 Central time, 6:30 Mountain time, and 5:30 Pacific time. I’ll do another one again next week.
Now, if you have a loved one in intensive care, go and check out intensivecarehotline.com, and call us on one of the numbers on the top of our website, or send us an email to [email protected].
Yeah, even though there’s people here, not everyone wants to ask a question, that’s absolutely fine. I hope that everybody got value out of it anyway, and the recording will be up later today after it’s been uploaded, and you can always ask questions below after the video has been uploaded and has been made available for everyone.
Now, if you are getting value out of this video, give it a thumbs up, subscribe to my YouTube channel for updates for families in intensive care and for livestreams. Comment below what you want to see next, what questions you have, comments or insights, and click the notification bell.
I once again want to thank you for coming onto the livestream and I want to thank you for your support, and I’m sure you’ll have more questions next week when we do another livestream.
Thanks again, everyone, for coming on and I will talk to you next week.
Now, if you have a loved one in intensive care and you want to go home with our service Intensive Care At Home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive Care At Home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Mornington Peninsula, Frankston area, South Gippsland, as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Also, we have been part of the Royal Melbourne health accelerator program in the past for innovative healthcare companies.
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
https://www.melbournehealthaccelerator.com/
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care At Home, and I’ll see you again next week in another update.







