Podcast: Play in new window | Download
The Very 10 Reasons Why You Need an NDIS Nursing Assessment for Medically Complex Disabilities
Good morning, good afternoon, good evening, wherever you are. Thank you so much for joining this live stream and for joining me today. I also want to welcome any of you who watch this on replay.
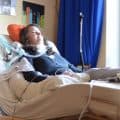
Today’s topic is Intensive Care at Home specific, “The very 10 reasons why you need an NDIS nursing assessment for medically complex disabilities.” So, this is today a live stream that is unique for our Australian viewers that are having complex disabilities or for any family member that has family member with complex disabilities. We are talking mainly about ventilation, tracheostomy or long-term ventilation and tracheostomy, tracheostomy without ventilation, ventilation without tracheostomy. We’re talking about neurological condition seizure management. We are talking about complex disabilities such as when people need TPN (total parenteral nutrition), IV antibiotics, IV potassium, IV magnesium. That’s what we will be covering today. Obviously, this is, like I said, Intensive Care at Home specific for our viewers in Australia.
Before we go into today’s topic, what makes me qualified to talk about today’s topic? Once again, my name is Patrik Hutzel. I’m the founder and director of Intensive Care at Home. I am a critical care nurse by background. I have worked in critical care for nearly 25 years in three different countries where I also worked as a nurse manager for over 5 years in critical care. I have been running Intensive Care at Home in Australia since 2013. I was also involved in the early 2000s in setting up Intensive Care at Home in Germany, in Munich, as part of a private organization, and we were the first ones doing Intensive Care at Home in Germany. So, I have a broad range of experience in intensive care as well as with Intensive Care at Home.
We have been NDIS (National Disability Insurance Scheme) accredited pretty much from Day 1 here in Australia and we’ll talk more about that. I am also running a consulting and advocacy service for families in intensive care at intensivecarehotline.com, and we’ve been doing that since 2013. We have saved many lives with Intensive Care Hotline as much as we have saved many lives with Intensive Care at Home.
So, without further ado, let’s dive into today’s topic about, “The very 10 reasons why you need an NDIS specialist nursing assessment when you have a loved one with a complex disability or when you have a loved one with a disability in intensive care or at home already.” Once again, with Intensive Care at Home, we are currently operating all around Australia. We are NDIS accredited, we are TAC (Transport Accident Commission) accredited and WorkSafe accredited in Victoria. NDIS obviously is a nationwide initiative. We are also an iCare-approved service provider in New South Wales as well as NIISQ (National Injury Insurance Scheme in Queensland), DVA (Department of Veteran Affairs) all around Australia. We are also having received or we have received funding through private health insurance, departments of health, as well as private health funds.
Let’s look into, “The very 10 reasons why you need an NDIS nursing assessment for complex disabilities.” So once again, what are complex disabilities in the NDIS world? Well, complex disabilities are often disabilities that lead to the need of mechanical ventilation, tracheostomy, or they lead to a tracheostomy without ventilation, or they lead to ventilation without a tracheostomy such as BIPAP (bilevel positive airway pressure), CPAP (continuous positive airway pressure) or they lead to the need of TPN. TPN stands for total parenteral nutrition, which in essence means intravenous nutrition, is then also the need for a central line, for a PICC (Peripherally Inserted Central Catheter) line, for a Hickman’s line or for a port, which are all things we can manage with Intensive Care at Home.
With Intensive Care at Home as well, we are sending critical care nurses into the home, 24 hours a day, for clients that otherwise would be stuck in intensive care long-term or would potentially receive palliative care in intensive care would die, whereas if we take them home, we can improve their quality of life and in some instances, quality of end of life. But many of our clients would’ve been in ICU for a long time and many intensive care teams would’ve palliated them, whereas we are an option to prolong life at home, often for many years.
So, the biggest challenge for families in intensive care in situations like that is that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care.
So, we are bridging the gap between hospitals, complex discharges, and home, but we are also bridging the gap for patients that are at home already or NDIS participants that are at home already that don’t get the right level of support and that are at risk of hospital readmissions, ICU readmissions, and they’re at risk of dying.
Case in point, we had some clients at home in recent years where the NDIS was only funding night shifts and wasn’t funding the day shift for critical care nurses and those clients passed away during the day because the NDIS was negligent and not funding the day shift ICU nurse, and then support workers or family members couldn’t manage medical emergencies on ventilation tracheostomy, and it’s been gross negligence from the NDIS. That was in the earlier days of the NDIS, when NDIS was funding nursing care, but obviously they’ve been negligent in other cases too in the meantime, and they’re trying to send support workers to patients with the ventilator and a tracheostomy. That is negligent. That is like flying the airplane with a cabin crew instead of the pilot.
If that happens, patients go back to hospital all the time, they go back to ICU all the time or they die, and then everyone is trying to sweep it under the carpet and no one can be held responsible, whereas it’s the funding body that is responsible not putting the right level of care in the first place. But it’s also the fault of the organizations that take on work they shouldn’t take on they’re not qualified for.
Intensive Care at Home, we are the only organization in Australia in 2024 that actually has accreditation for Intensive Care at Home that has accreditation to look after long-term ventilated adults and children at home with tracheostomy. We are the only provider in the country that has third-party accreditation to look after patients at home on a tracheostomy that has that level of accreditation, and other providers simply don’t have it. Same with home TPN. We are the only provider that has the level of accreditation to provide that level of service.
Now, without further ado, let’s look at the 10 reasons why you need an NDIS nursing assessment for medically complex disabilities. Now, I do need to go one more step back because it is such a sort of complex topic. I’ll give you a real-world example now. So currently, we’re having an inquiry from a patient with a tracheostomy living at home but is going into hospitals all the time. The patient has been at home with support workers and family members, but going into hospital, it’s just a level of care that is not appropriate, it’s not sustainable, and this lady is at risk of dying if she doesn’t get 24-hour nursing care pretty quickly.
So, what needs to happen in a situation like that? First of all, there needs to be the right NDIS Support Coordinator. With the right NDIS Support Coordinator, everything can change, everything can be turned around. The NDIS Support Coordinator knows how to advocate with the NDIS for the right level of care, knows what reports need to be done, knows who needs to be on the team to get 24-hour nursing care, for example. If you’re not having the right NDIS Support Coordinator, you will be fighting an uphill battle.
So, we have our own NDIS Support Coordinator, Amanda, and she can help you with all of that. She speaks the NDIS lingo, whereas we speak the clinical lingo and we can advocate on a clinical level, but there’s also a lot of NDIS language that people need to know about, and they need to know how to speak to the NDIS and advocate in the right way.
So, in a situation like that, just like I mentioned with this client with a tracheostomy, a change of circumstance and a plan review needs to be triggered. When that is triggered, then a number of things need to happen. There needs to be an OT assessment, a functional capacity assessment, there needs to be an NDIS nursing assessment, there needs to be a physio assessment and there needs to be a doctor’s letter as well.
Now, when it comes to the NDIS nursing assessment, that leads me to number one, why you need a specialist nursing assessment is that because we have unique NDIS knowledge and we know how those nursing assessments need to be written, not many providers know about that. So, for example, when you need to advocate or when we advocate for nursing care through the NDIS, the whole report needs to be brought back to disability, not to health issues. So, for example, if you’re advocating with the Department of Health for funding for nursing care, you can talk about the health issues a patient or a participant has. With the NDIS, you need to talk about the disability first and then lead it to the health issue. Only then will the NDIS fund the nursing care, if the primary issue is the disability that leads to the health issues.
For example, case in point, we are looking after some patients at home with MND (Motor Neuron Disease). The motor neuron disease is the underlying disability that leads to inability to breathe, which leads to the need of a tracheostomy and mechanical ventilator.
So, in isolation, the ventilation and the tracheostomy is a medical issue, but it’s actually triggered by a disability, and the report always need to be linked back to the disability causing the health issue, and that’s when the advocacy works. The NDIS will then fund the nursing care. Once again, mechanical ventilation and tracheostomy is the skill of an intensive care nurse, not the skill of a support worker, it’s not even the skill of a registered nurse without intensive care experience. Once again, sending registered nurses without intensive care experience or sending support workers to a ventilated client, that is negligence. It’s madness. It’s like flying the airplane with a cabin crew instead of the pilot, and patients have died because of it, and they will continue to die or take significant harm if that practice continues. It’s actually also not best practice, it’s also not evidence-based practice.
So, if you go to our website, intensivecareathome.com, you will find a section on our website, the Mechanical Home Ventilation Guidelines. The Mechanical Home Ventilation Guidelines are actually evidence-based. The evidence there clearly shows that only intensive care nurses with a minimum of 2 years intensive care nursing experience are safe to provide care at home for a ventilated and tracheostomy client, or if someone is not ventilated but has a tracheostomy, needs 24-hour intensive care nurses. Once again, those intensive care nurses need to have a minimum of 2 years ICU or pediatrics ICU or sometimes ED (Emergency Department), experience as well.
Now, those guidelines are a result of over 25 years of Intensive Care at Home nursing in Germany, and they are a result of over 10 years of Intensive Care at Home nursing in Australia. Because patients have died, if they’re not getting the minimum standards, which is 24-hour nursing care with critical care nurses at home, patients have died, patients go back to ICU all the time and are at high risk of dying. You’re more than welcome to contact me if you want me to show you evidence that patients have died because of it. You’re more than welcome to contact me at intensivecareathome.com. You can call us there on one of the numbers. You can ask for me. I’m more than happy showing you the evidence in case you are questioning what I’m saying. So that’s the first point, so the unique knowledge about how to write this report. Number two, the clients that we are advocating for, the clients with complex medical disabilities, are, generally speaking, on life support.
Now, what does that mean? If a patient is on life support in a hospital, they are in intensive care, or the lowest level of life support might be BIPAP or CPAP, and sometimes patients can be on a respiratory ward, but generally speaking, 99% of patients on life support are in intensive care. So, if the NDIS says we can use support workers or general registered nurses, why are we not having support workers or general registered nurses in ICU in a hospital? Please answer that question. Well, those patients would be dying without an intensive care nurse, which is what’s happening in the community if they’re not looked after by intensive care nurses with a minimum of 2 years ICU experience as is evidence-based by the Mechanical Home Ventilation Guidelines that I just mentioned a minute ago.
So, to write a nursing assessment for patients on life support, that requires the skill of critical care nurses. It doesn’t require the skill of a registered nurse, doesn’t require the skill of an enrolled nurse. It requires the skill of an intensive care nurse. Our people that we have on our team that write our NDIS nursing reports are critical care nurses. Two of them also have completed a legal nurse consulting degree. So, they combine the reports, not only the clinical side of things but also the legal side of things, i.e., if the NDIS continues to be negligent with some clients and won’t fund the nursing care, they are also liable and they’re liable if something happens. So, that all needs to be in the report. So, it’s actually documented that if something was to happen down the line, God forbid, because the NDIS isn’t funding what’s clinically appropriate and what’s appropriate for the level of disability, that they can be held accountable.
Next, an NDIS nursing assessment needs to tie in with an OT report (Occupational Therapy report), needs to tie in with the physio report, and needs to tie in with the doctor’s report. So, all the reports need to be aligned, and that is usually no issue if you have people understanding intensive care and Intensive Care at Home. So, very simple, you need to have the right people on the team to make things happen, and you need to have the team aligned to say the same things to the NDIS, which isn’t difficult when someone is on a ventilator with a tracheostomy. Most of the time they’re bed bound, they have an inability to move, so without 24-hour nursing care, without 24-hour ICU nurses, they’ll be dying regardless.
That leads me to number three, and number three is that the alignment of those reports creates the right multidisciplinary team. It’s very important that when you get the reports together for the NDIS, that you have the right team. The right team starts, obviously, with the right advocacy, starts with Intensive Care at Home, we have our own NDIS Support Coordinator. It continues with the OT, it continues with the physio, it continues with the doctors. Once you gather all these evidences, the NDIS can’t really refuse because when the evidence is overwhelming. What are they going to do? They wouldn’t take the risk to be negligent, but it has to be the right level of advocacy and the pressure has to be applied. So, the right team is critically important. When we work with clients here at Intensive Care at Home where we send critical care nurses into the home, 24 hours a day, for our clients, I believe we have the right team, otherwise it wouldn’t work.
Next, families lack insights. They don’t really know where to start and they think whatever an NDIS Support Coordinator or an NDIS planner is throwing at them is just what it is. Patients have no idea or NDIS participants, and their families have no idea that they actually have rights, but you need to exercise them, and you also need to know where to get those insights. You need to know where to get those insights and you need to have the people that have dealt with the NDIS, how to speak to the NDIS, how to speak to NDIS planners.
Also, what’s also important is you need to find a complex NDIS planner. If you don’t have an NDIS planner who understands the complex disabilities, don’t deal with them. Ask for a different one. You need to know what team to assemble. If your NDIS planner, working for the NDIS, is not a complex disability planner, sack them, get a new one because they don’t understand the complexities. An NDIS planner that’s working in the complex disability world is much better than a general planner because they have a much better understanding of what you and your family need.
That leads me to the next point. It is critically important that you know where to find the relevant expertise. Again, I’ll give you another example. Sometimes we get calls from NDIS Support Coordinators who say, “Hey, I’ve got this patient here in ICU and they’re on a ventilator, they’re with a tracheostomy, and they’ve got an NDIS plan for 24-hour support workers.” They ask me, “Can Intensive Care at Home take this patient home?” I said, “That’s a death sentence to provide 24-hour support workers for an intensive care patient. That’s a death sentence.” Like I said, patients have died because of it.
So, that leads me back to, (A), you need a good NDIS Support Coordinator. Number two, you need to know where to find expertise. NDIS Support Coordinators who want to find a provider for 24-hour support workers for an intensive care patient, they are negligent and they don’t have the level of expertise that is needed to help your family member in a situation like this. If an NDIS Support Coordinator comes to me and brings a situation like that to me, one of the questions that I’m asking is, “What makes you qualified to make decisions or potentially advocate for an intensive care patient?” I get silence. We employ hundreds of years of intensive care nursing experience on our team, hundreds of years, combined. Combining that level of expertise with an NDIS Support Coordinator who’s well versed within the NDIS language, that really rocket fuel for the advocacy. So, it is critically important that you know where to find expertise. Once again, the nursing assessment is a critical component, but it is very important that you have the right people on your team.
At the moment, we are working with a client who is dealing with an NDIS Support Coordinator who didn’t want to advocate for nursing care for tracheostomy ventilation. I’m keeping this very private here, but the client is now talking to us because the client is realizing that the other NDIS Support Coordinator is completely outside of their depth when it comes to ventilation and tracheostomy. They are very negligent, and they would just let the client go home with support workers, which, once again, is a death sentence in many cases. So, it’s critically important that you align yourself with people who know where to find the area of expertise.
Next point, you want a smooth hospital discharge. You want a smooth hospital discharge. Here’s what I mean by that. Recently, in April this year, we have done some shifts with a tracheostomy client here in Melbourne, and we only did a couple of weeks. The tracheostomy client went home earlier this year after a long hospital stay, and went home with a tracheostomy, not ventilated, but this patient is paralyzed. Then one day, we get a phone call saying, “Oh, we need some nursing shifts. Can you help? We’ve heard about Intensive Care at Home, can you help?” So, we went there, started doing some nursing shifts, but we also knew the NDIS plan was running out in a couple of weeks and there was no more funding. Then the client went back to hospital because there was no more funding.
But here’s another thing that the family told us at the time when the client first went home, there was some funding for nursing care and then they went on to Mabel. Mabel is like the Uber for the NDIS. You basically look up people’s profile on the Mabel app and then you can select registered nurses, support workers, and whoever else might be putting their resume on that platform. Then, those registered nurses showed up at the client’s home and as soon as they saw a tracheostomy, they walked out again. So, what that means is, once again, like I said earlier, not even a registered nurse without ICU experience knows how to handle a tracheostomy. That’s what I mean when everything is in place, if everything is lined up, you want a smooth hospital discharge.
Another benefit of Intensive Care at Home and having the appropriate nursing funding is we keep our clients home predictably. So, this client already had multiple hospital readmissions because the funding wasn’t there, the level of expertise wasn’t there even if the funding was there, and the hospital discharge did not go smooth, he’s already bounced back into hospital.
You don’t want any of that. You don’t need any of that drama. You want to go home, and you want to stay at home and maximize your quality of life, and you want to have the service that makes that happen predictably, which is what we do with Intensive Care at Home. Like I said, we employ hundreds of years of intensive care nursing experience in the community. We are actually accredited for Intensive Care at Home. No other provider has that level of accreditation or has that level of expertise and intellectual property than we have with Intensive Care at Home. So, you want a smooth hospital discharge and an NDIS nursing assessment will lead to that.
Now, let’s move on to our next point. Number seven. I briefly hinted to that already, but I think it’s even more important that I mention it again. So, your internal team needs to comprise of a Level 2 or Level 3 NDIS Support Coordinator who actually has dealt with complex disabilities, who actually knows how to advocate for nursing care. That’s number one.
You need the right nursing team, which we can provide for you, you need the right OT, you need the right physiotherapist, you need the right speech therapist, you need the right team to make things happen for you, also includes your doctor as well. But I hinted towards that earlier, you also need the right NDIS planner. So, the NDIS planner is someone working for the NDIS. They approve your plan, but that needs to be a complex NDIS planner.
So, like I said, I believe the level of incompetence at the NDIS is pretty high. Most of them are bureaucrats. They’re not clinicians. They don’t even know what they sign off on. The complex NDIS planners are probably in a little bit of a different category. They often do know about complex disabilities, and they do know the level of risk. They do know the level of care that is needed for those clients.
So, if you are a family member or if you yourself are dealing with ventilation, mechanical ventilation, tracheostomy, neurological condition, seizure management, PEG (Percutaneous Endoscopic Gastrostomy) tube management, TPN, central line management, port line management, IV potassium infusions or palliative care, you need a complex NDIS planner. If you don’t have a complex NDIS planner, you need to sack them and you need to ask for one. It’s inevitable. Once again, a good NDIS Support Coordinator will also be able to help you with finding a complex NDIS planner. So, your NDIS Support Coordinator plays a critical role when you have a complex disability.
So, next reason why you need a specialist nursing assessment is leading to my previous point that you want a smooth hospital discharge, you want to avoid hospital readmissions. So, once again, giving you another real-world example. In the earlier days when we first got started with one client, there was a client who was at home ventilated with a tracheostomy and a ventilator, and he went back to ICU almost every second day because he either had no staff or he had incompetent staff. He had support workers predominantly, or he had registered nurses without intensive care experience, and he was going back into hospital all the time because that provider could not keep him home. That was actually our first client. Well, within a few days of us working up there, we were keeping him home. More importantly, we were keeping him home predictably. He never ever went back to ICU when we worked with him. That is our promise, and that stands.
Like I said, just with this other client who went back to ICU recently, when we were there for a few weeks, it was only a few weeks because of the funding was running out. Again, the NDIS Support Coordinator that would’ve managed that would’ve been sheer incompetence letting funding run out.
The goal is for you not to go back to hospital or for your family member or for anyone for that matter, unless it’s something elective, unless it’s something planned, maybe you need to go for a procedure or whatever the case may be, but the goal needs to be to stay home predictably. Once again, this is what we do at Intensive Care at Home. Our clients stay home predictably. That is all mapped out in NDIS nursing assessment, how do we actually achieve avoiding the hospital readmissions?
Now, number eight. Again, I hinted towards that, but I feel like I need to break it down in much detail simply to avoid death. Once again, many patients at home with ventilation, tracheostomy, seizure management have died because they didn’t have 24-hour nursing care at home with intensive care nurses. So, when someone is on a ventilator and a tracheostomy, they are on life support. Once again, if patients in a hospital are on life support, they are in intensive care and they need doctors and nurses around them that are competent to deal with life support 24/7. Now, we don’t need a doctor at home on site like they are in intensive care, but you need a critical care nurse, 24 hours a day. Once again, that is evidence-based. Have a look at the Mechanical Home Ventilation Guidelines that are evidence-based on our website at intensivecareathome.com. I can’t stress this enough that going home without intensive care nurses is, 24 hours a day, when it comes to ventilation, tracheostomy, when it comes to tracheostomy without ventilation, when it comes to ventilation such as BIPAP, CPAP, could be a death sentence. Once again, I have evidence for what I’m saying here. Please reach out to me if you want to know more.
Number ten, you want to maximize quality of life and, in some instances, quality of end of life. What does that mean? Well, if you’re stuck in hospitals or in intensive care, there is no quality of life, and at home there is quality of life. If you’re at home already and you have insufficient support because you have support workers and there’s gaps and all, and you know that support workers are incompetent. They don’t have the expertise that you actually need to keep your home predictably and live your life, live a good life, once again, you urgently need reach out to us before it’s too late. Your life is at risk, and you don’t even know it. It might be fine 364 days of the year. If your tracheostomy blocks tomorrow and the support worker doesn’t know what to do, that could be a death sentence.
I wish I had nicer things to say here, but that’s just the reality of me having done this work for the last 25 years. It’s just the reality. I’m well aware of the risk. You need to face reality. You need to look in the eye of reality, otherwise you are putting yourself or your family member at risk.
So, that concludes the 10 reasons why you need a Specialist NDIS Nursing Assessment when it comes to complex disabilities. You might be watching this, and you might be dealing with other funding bodies such as private health insurance or TAC in Victoria, maybe NIISQ in New South Wales, NIISQ in Queensland and iCare in New South Wales, maybe DVA. We can write other nursing assessments too, but more and more is moving towards the NDIS, and therefore I thought it was very important to break down the complexities of the NDIS and how we can help. So that is very, very important.
Now, if you have any questions, I also encourage you to type your questions into the chat pad here, or if you do want to get on live on the show here, I can get you on the show here by you clicking on the link here and you can talk to me directly.
Now, once again, with Intensive Care at Home, we are currently operating all around Australia in all major capital cities as well as in regional and rural areas. We are an NDIS approved service provider all around Australia, including Level 2 and Level 3 NDIS Support Coordination. We are TAC approved in Victoria, WorkSafe approved in Victoria, iCare, and WorkSafe approved in New South Wales, NIISQ in Queensland, DVA around the country. We have also received funding through departments of health, through public hospitals as well as private health insurance, so please reach out to us if you have any questions around that. Like I said, we also provide Level 2 and Level 3 NDIS Support Coordination.
We have also sent our critical care nurses into the home to bypass ED (Emergency Departments). So, we have worked for the Western Sydney Local Area Health District, and we have sent for the in-touch service, and we have sent our critical care nurses into the home to prevent emergency department admissions. For example, changing nasogastric tubes at home, changing tracheostomy tubes at home, changing catheters at home, putting on back-slabs. So, we can do the same for your hospital, we can do the same for your nursing home, bringing that level of expertise into the home and avoiding ED admissions of interest for patients at home for patients in residential aged care for obviously hospitals to offload their EDs.
Now, if you’re watching this and you’re an NDIS Support Coordinator working for another organization and you’re looking for nursing care for your participant, we can help you, or if you’re looking for more insights, how to advocate for nursing care through the NDIS, we’d love to help you. If you need an NDIS nursing assessment for your participant, we would love to help you. We have done it successfully, otherwise we wouldn’t be in business.
Your loved one, if you’re watching this and you are in a hospital and you are in a similar situation, either yourself or if you have a family member in a similar situation, please contact us at intensivecareathome.com. Call us on one of the numbers on the top of our website or send us an email to [email protected]. You might be at home already and you might have insufficient support.
Like I said, all of our nurses have a minimum of 2 years critical care nursing experience. We are the only service in Australia that is actually accredited for Intensive Care at Home nursing. We have built the intellectual property. We have built the teams that make Intensive Care at Home possible. Obviously, like I said, our service is evidence-based. There’s no evidence that support workers can do the work that we can do. The evidence for support workers is that people have died. That’s the evidence.
Now, also, if you are a critical care nurse and you’re looking for a career change, we want to hear from you as well. If you have worked for a minimum of 2 years in critical care, ICU, pediatric ICU, ED, and you ideally have completed a postgraduate critical care qualification, we currently have jobs in Melbourne, Sydney, Brisbane, Albury, Wodonga, in Bendigo, as well as in Warragul in Country Victoria, we want to hear from you. We are looking for intensive care nurses and critical care nurses that want to complement our team, people who are team players and people who are looking for regular work. We are a service provider and not an agency. We do pride ourselves on providing a tailor-made solution to our clients, and that includes having a regular team, regular people working with our clients. If you’re an intensive care specialist or ICU consultant, we are currently expanding our medical team as well. Please reach out to us if you have any interest in Intensive Care at Home.
If you’re an intensive care specialist and an ICU consultant and you have bed blocks in your ICU, you can reach out to us as well. We can help you eliminate your bed blocks, and more importantly, we can improve the quality of life and sometimes quality of end of life for your patients and their families, and you won’t even pay for it.
Once again, if you’re a hospital executive watching this, we also want to hear from you because we can help you eliminate your bed blocks in ICU and ED. If you are in the U.S. or in the U.K. and you need help, please reach out to us as well. We can help you there privately.
Once again, our website is intensivecareathome.com. Call us on one of the numbers on the top of our website or send us an email to [email protected].
If you like my videos, subscribe to my YouTube channel for regular updates for families with Intensive Care at Home, but also for families in intensive care, click the like button, click the notification bell, share the video with your friends and families, comment below what you want to see next, what questions and insights you have.
I do a weekly YouTube live, and if you’re a subscriber to my YouTube channel, you can get notification there or subscribe to our email newsletter at intensivecareathome.com and you will get notification there when I do a YouTube live.
Thank you so much for watching.
This is Patrik Hutzel from intensivecareathome.com and I will talk to you in a few days.
Take care for now.