Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults& Children with Tracheostomies by improving their Quality of life and where we also provide tailor made solutions to hospitals and Intensive Care Units to save money and resources, whilst providing Quality Care!
In the last blog I shared
You can check out last week’s episode by clicking on the link here.
In this week’s blog I want to answer a question from one of our readers of our blog and the question this week is
My 73 year old Mom had a stroke and is intubated in Intensive Care. She can’t come off the ventilator and the breathing tube, can she have a tracheostomy and go home and have INTENSIVE CARE AT HOME?
Hi Patrik,
my otherwise very healthy 73 year old mother had a stroke around 2 weeks ago. She is still in ICU in one of the big public Hospitals in Melbourne as she needs ventilator with pressure support and the breathing tube to help her breathe. The doctors haven’t given her much hope unless her breathing on her own improves. I am wondering if your service INTENSIVE CARE AT HOME can be an option for her?
Just some more details and to shed more light on her current situation. Her CO2(=Carbondioxide) levels were getting high when her pressure support was down to 7 so they’ve put it back up to 8. CO2(=Carbondioxide) levels at the moment are fluctuating between 57-67 mmHg.
She’s currently off all sedation and is getting more and more awake and she seems to be out of the induced coma by now.
She’s responding and she has made it very clear that she wants to fight and that she wants to live!
I was hoping to get the ICU to do a tracheostomy and then get her home with your INTENSIVE CARE AT HOME service if she can’t get off the ventilator soon.
The doctors in the ICU were quite adamant that tracheostomy isn’t an option for her since the amount she is breathing at the moment isn’t enough to sustain life and they seem to have the opinion that most of the swelling in the brain would’ve gone down by now. Anyway, I was adamant with them about giving her time and they agree with that and are relaying my thoughts to the main ICU consultant on duty this week.
They’re saying her breathing levels, the amount she’s taking in, isn’t high enough to sustain life. I.e. she’s taking in 200 mls and she needs to be at 400 mls per breath she’s taking. Also they’re saying no nursing home will take someone with a ventilator and I raised tracheostomy and ventilation at home as an option and they said it be highly involved with 24 hour care needed pretty much.
Can you please let me know what our options are?
Regards,
Steve
Hi Steve,
thank you for your question and enquiry.
We can definitely help you with INTENSIVE CARE AT HOME should your mother have a tracheostomy down the line and can’t come off the ventilator. Even if your mother needs ventilation with a mask(BIPAP mask/NIV) down the line in a home care environment we can help you.
We can provide up to 24/7 Intensive Home Care nursing once your mother is medically stable and off inotropes/vasopressors. It doesn’t sound to me like she’s on inotropes/vasopressors, therefore once your mother has a tracheostomy she should be able to go back home with our service INTENSIVE CARE AT HOME.
It’s good to hear that you are standing your ground and it’s good to hear that you are asking all the right questions and that you’re asking for what you want. Most families in Intensive Care are too timid to do that, they are often too scared and intimidated by the Intensive Care team’s “perceived power” and “perceived authority”.
99% of families in Intensive Care are too timid to ask for what they want and they therefore make no informed decisions, have no peace of mind, no control, no power and no influence!
The good news is that even if your mother can’t breathe by herself without the breathing tube she can have a tracheostomy.
If they don’t want to do a tracheostomy and your Mother has private health cover, you may also want to consider to get her into a private ICU and get the tracheostomy done there.
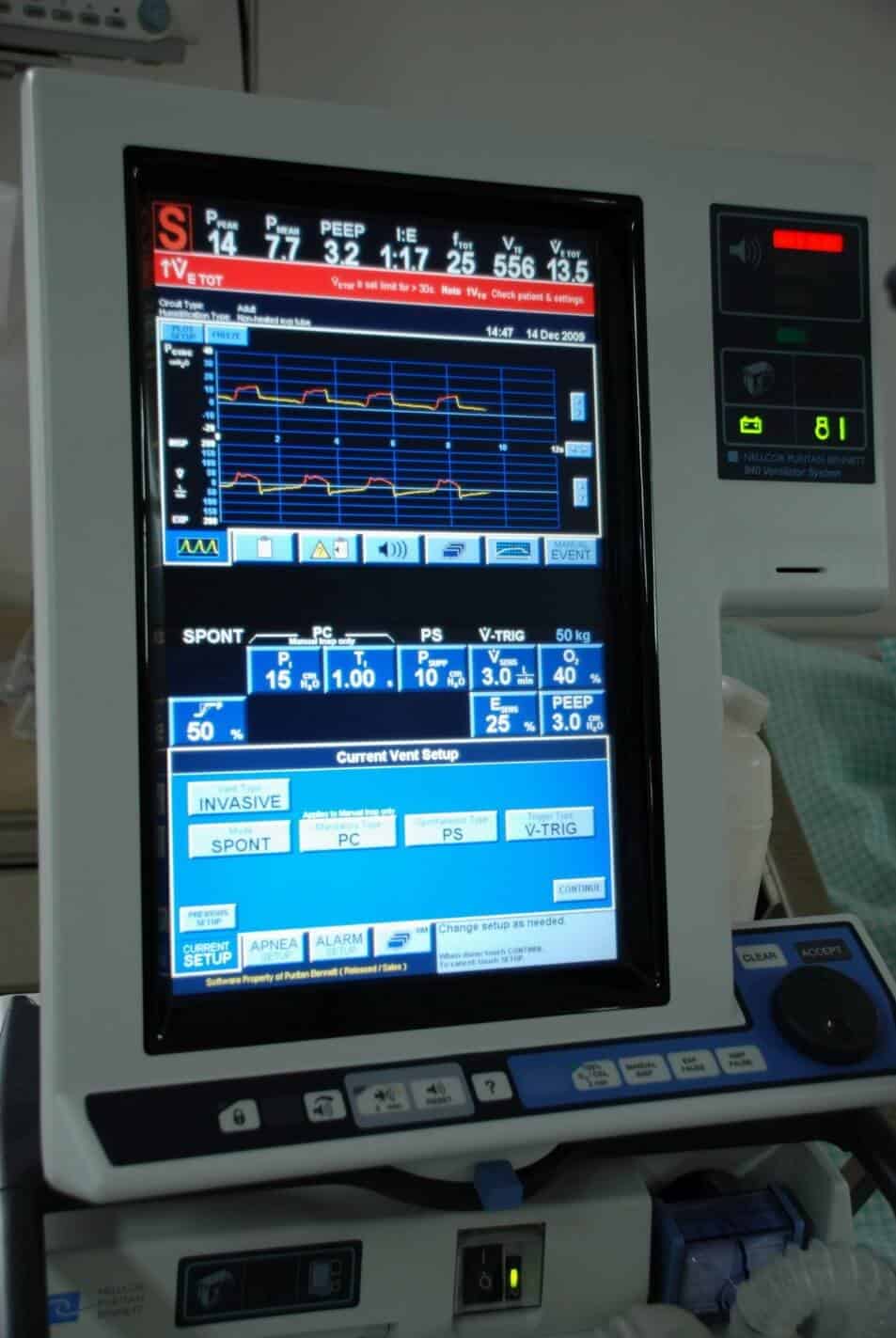
Given that she has now been ventilated for over two weeks it’s time to do a tracheostomy.
Here is more evidence around this and when and why a tracheostomy should be done.
Related articles/videos:
Not doing a tracheostomy after about two weeks is not best practice, especially since your mother is awake, can follow commands and is able to communicate what she wants when asked.
As you would have seen by now, a breathing tube whilst being awake is very uncomfortable and it isn’t really best practice as you can see in the articles and videos that I linked towards.
Once she has a tracheostomy and she’s medically stable we can take her home with INTENSIVE CARE AT HOME. This creates a “win-win” situation because we can give you, your family and your mother what you want and we can reduce the cost of an Intensive Care bed by around 50%.
We therefore also help the Intensive Care Unit to save 50% of the cost and free up one of their precious, expensive and “in-demand” Intensive Care beds.
Also, if her tidal volumes are around 200 mls instead of 400 mls of course her CO2(=Carbondioxide) levels are high.
Increasing pressure support(PS) might help and if it doesn’t help, they will have to put her back into a different ventilation mode such as SIMV where she gets more help and assistance from the ventilator with set breaths per minute.
You see from my perspective, not giving your mother the option to have a tracheostomy could potentially kill your mother and that to me is negligent as far as I’m concerned, especially since you, your family as well as your mother have made your wishes clear!
Furthermore, as you may well know, many Patients can live at home with a ventilator and tracheostomy with our service INTENSIVE CARE AT HOME, therefore why deny this service to your mother?
The Intensive Care team is correct to say that no nursing home will take her and why would you or your mother chose to go to a nursing home anyway if Intensive Home Care is a viable and also more cost effective option compared to an Intensive Care bed?
The good news is that you and your family are positive and staying focused and staying positive helps tremendously in a situation like this!
If they had your mother’s best interest at heart, they would do a tracheostomy because a tracheostomy would make her more comfortable and it would give her time to recover and it will be easier to wean her off the ventilator.
Instead, they are telling you “your mother won’t improve” without looking at what your mother’s life may look like in two months, 6 months or 2 years time.
Of course, there are no guarantees, but throwing in the towel now doesn’t sound right to me and once again not offering a tracheostomy because they think “she’s not getting better” just simply doesn’t sound right to me without trying and without giving her more time.
Your mother is just at the start of what may potentially be a long recovery. There are no guarantees of course, but they need to try and they haven’t really tried yet.
You are doing pretty well, positioning your mother’s diagnosis, prognosis as well as her care and her treatment and I can see you are not scared, timid or intimidated which will help you, therefore well done!
Kind Regards
Patrik
If you want to find out how we can help you to get your loved one out of Intensive Care including palliative care or Long-term acute care(also nursing home) or if you find that you have insufficient support for your loved one at home on a ventilator or if you have any questions please send me an email to [email protected] or call on one of the numbers below.
Australia/New Zealand +61 41 094 2230
USA/Canada +1 415-915-0090
UK/Ireland +44 118 324 3018
Also, check out our careers section here
www.intensivecareathome.com/careers
We are currently hiring ICU/PICU nurses for clients in Melbourne, Sunbury and in South Gippsland/Victoria.
We are an NDIS, TAC(Victoria) and DVA(Department of Veteran affairs) approved community service provider in Australia.
We have also been part of the Royal Melbourne health accelerator program earlier this year!
https://www.thermh.org.au/news/innovation-funding-announced-melbourne-health-accelerator
Thank you for tuning into this week’s blog.
This is Patrik Hutzel from INTENSIVE CARE AT HOME and I see you again next week in another update!







