Podcast: Play in new window | Download
Hi it’s Patrik Hutzel from INTENSIVE CARE AT HOME where we provide tailor made solutions for long-term ventilated Adults & Children with Tracheostomies and where we also provide tailor made solutions for hospitals and Intensive Care Units whilst providing quality services for long-term ventilated patients and medically complex patients at home, including home TPN.
In last week’s blog, I talked about,
END OF LIFE CARE AT HOME WITH INTENSIVE CARE AT HOME, SOME CASE STUDIES!
You can check out last week’s blog by clicking on the link below this video:
In today’s blog post, I want to answer a question from one of our clients.
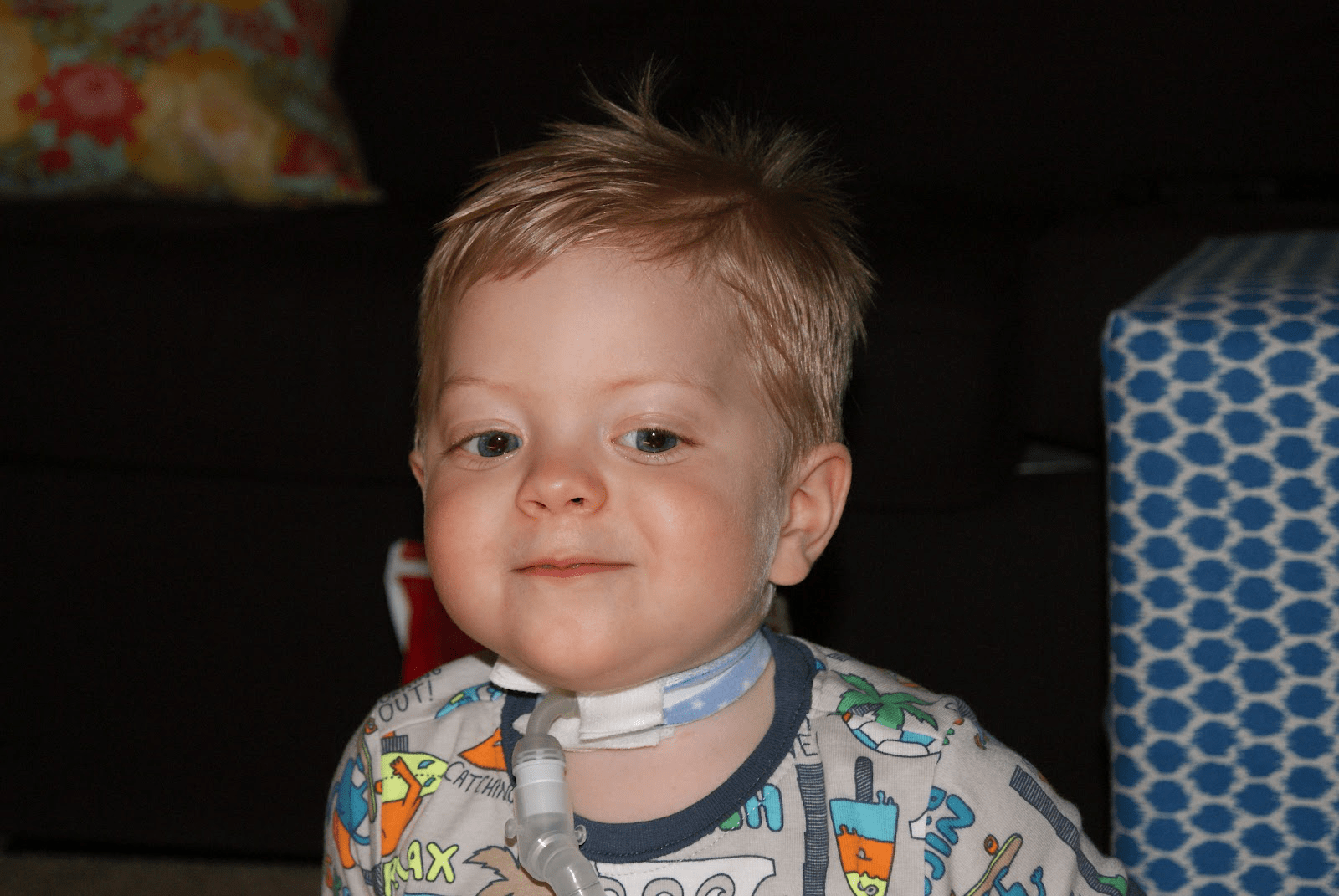
22-year-old Daughter with Cerebral Palsy’s Ventilated with Tracheostomy, How to Manage Excessive Secretions?
Hello, good morning, good afternoon, wherever you are. Welcome to another livestream for Intensive Care at Home and Intensive Care Hotline. I’ll give people a couple of more minutes to come in before we get started with today’s topics. I’ll just give it a couple of more minutes and then we will get started with today’s question, or with today’s questions I should say. So, I’ll just give it another couple of minutes.
So, welcome again to today’s YouTube live for Intensive Care at Home and Intensive Care Hotline. Before we go into today’s topic, thanks for coming into the show, whether you’re watching it live now or whether you watch it in the recording later on. Thanks for watching it. Thanks for your support.
If you have any questions today, just post them into the chat pad or you can also dial in live on the show on the numbers that I put in the chat pad. You can type your questions into the chat pad. Even if you watch it as a live stream, type your questions into the chat pad or below the video and then I will answer them on the next show or make a quick tip video about it.
Now, just quickly some housekeeping issues. So, type your questions into the chat pad. I will answer them. We will probably go for about an hour after today’s topic about the secretion management. I have other questions lined up that we were getting during the week. If you want to dial in live on the show, you’re more than welcome. I post the phone numbers into the chat pad.
Now, before we get started, in case you wonder what makes me qualified to talk about today’s topic, I am a critical care nurse by background. I have been working in intensive care/critical care for over 20 years in three different countries. I have also worked as a nurse unit manager for over five years in intensive care. I am the founder and also managing director of Intensive Care at Home, where we send intensive care nurses and pediatric intensive care nurses into the home to manage and look after predominantly long-term ventilated adults and children with tracheostomy at home, but we also provide services for non-invasively ventilated adults and children with BIPAP (Bilevel positive airway pressure)/ CPAP (Continuous positive airway pressure) ventilation. We provide tracheostomy management for non-ventilated clients, adults and children. We provide home TPN.
In a nutshell, we provide a genuine alternative to a long-term stay in intensive care. We help families to achieve their goals at home, and we help intensive care units to manage bed blocks, and we help the health system to save 50% of the cost of an intensive care bed.
I’m also the founder and critical care nurse consultant for intensivecarehotline.com and Intensive Care Hotline. We consult and advocate for families in intensive care and we have been doing so for the last 10 years. The same with Intensive Care at Home, we have been operating now for the last 10 years.
Intensive Care at Home, we are providing services all over Australia in all major capital cities, but also in regional and remote parts of Australia. Most of our clients are funded through the NDIS (National Disability Insurance Scheme), but also other schemes like the DVA, the Department of Veteran Affairs, accident schemes, work safe schemes, and so forth, but also sometimes through the Department of Health and Hospitals directly. So, if you are in Australia and you need Intensive Care at Home, you should contact us. But even if you’re not in Australia and you are in the U.K. or in the U.S., you should contact us as well if you need Intensive Care at Home. We can guide you with the next steps.
Without further ado, let’s get into today’s question. I had an email from a client this week who says, “My 23-year-old daughter with cerebral palsy is on a ventilator and has a tracheostomy. The question is what can be done for excessive sputum management? She’s in ICU at the moment and we want to go home as a next step, but we believe we need to manage and control the sputum first before we can go home with a service like Intensive Care at Home.”
So, that’s a great question because we have a number of clients at home with ventilation and tracheostomy where we manage sputum all the time, and we also have clients at home with cerebral palsy with ventilation and tracheostomy. So, this is actually a very good and timely topic because we encounter that issue every day with our Intensive Care at Home clients, and I want to break it down in manageable steps so you can understand what to do and what the hospital might want to do as well, what the ICU might want to do.
So, the first step in a situation like that where there’s excessive sputum production or anyone on the ventilator with tracheostomy is to start using a closed suction system. So, most ICUs nowadays use a closed suction system, but even in home care, you should start thinking about a closed suction system.
So, what are the advantages of a closed suction system? So, in the “old days,” when I first started in ICU, now 25 years ago, we were using single-use suction catheter. So, we disconnected the patient from the ventilator, we would suction down the tracheostomy tube. There’s a number of issues that came with that. Number one is patients lose the PEEP on the ventilator, so it decreases their respiratory function. Number two, there’s an increased infection risk because you’re basically opening up the airway to infection. Number three, it takes a lot longer to get ready for suction as opposed to a closed suction system. So, you’re losing valuable time in suctioning the patient or the client, and it needs to be quick and efficient.
So then about 20 years ago, the closed suction systems came in. What that means is you’re attaching a closed suction system between the tracheostomy and the ventilator. You don’t need to disconnect, or you only need to disconnect once in 72 hours because those closed suction systems need to be changed every 72 hours. But more importantly, patients do not lose PEEP, oxygen. It’s much easier to handle. It’s much quicker. You can really suction way more often because it’s really smooth and you can use it very quickly, and especially in emergency situations as well, it’s much easier to deal with. So, that’s the first step that they might want to look at using a closed suction system.
Then, other things that they need to look for is simply regular nebulizers. Regular nebulizers that can go from saline nebulizer, normal saline nebulizers to Atrovent, atropine nebulizers to help manage the secretions as well.
Next, maybe a little bit counterintuitive, but really important is chest physiotherapy or chest exercise, breathing exercises, coughing exercises. I know that’s very difficult with cerebral palsy, but a good chest physio can still do massage, use creams, use gentle rubs to mobilize secretions as well. So, there’s a lot that can be done on that level as well with a good physiotherapist that has the experience and the knowledge to manage secretions.
Next, a cough assist machine. If you are watching this, you may not have heard of a cough assist machine. Now, a lot of our clients at home with spinal injuries, C1, C2, spinal injuries, but also C4 or C5 sometimes use a cough assist machine, whether they’re invasively or non-invasively ventilated, i.e., whether they’re ventilated with a tracheostomy or whether they are ventilated non-invasively by CPAP or BIPAP. Sometimes the cough assist is even used for patients with a tracheostomy that are not ventilated.
So, what does the cough assist machine do? How does it work and how does it help to manage secretions? So, without getting too technical here, cough assist works as follows. So, you’re attaching the cough assist machine to the tracheostomy or even for a non-tracheostomy client if someone is on BIPAP, CPAP, then using a mask, applying it to the face. You are giving a high PEEP of about 20, 25, sometimes even 30 for about three or four breaths, and then you’re giving a negative PEEP of around minus 25 or 30, and that is what makes a patient cough. It can be very uncomfortable, but it’s extremely effective to clear out any secretions at one go.
Obviously, you then need to have the suction machine ready so that you can suction straight away. That’s what we do with most of our clients at home with Intensive Care at Home. Many of them have a cough assist machine. It’s incredibly effective, but you need to know what to do. Again, clients have it whether they are invasively ventilated with a tracheostomy or whether they are non-invasively ventilated. Very, very effective, but you need to know what to do. ICU nurses can do that to use a cough assist machine. So, we talked about the nebulizer already.
Then let’s look at medication management, how you can manage the excessive secretions? Some medications that can be used for excessive secretion management is glycopyrrolate, atropine, and I talked about the Atrovent nebulizer already. We have a number of clients at home that are on glycopyrrolate or atropine. Look, for anyone that’s ventilated, I would still argue from my experience that the cough assist is more effective, but certainly glycopyrrolate or atropine and Atrovent nebulizers can be used as well to minimize excessive secretions.
By the same token, you don’t want to dry up secretions either. You want to have the natural flow of it. You want to get rid of them with the techniques that I described earlier whether it’s suctioning with a closed suction system, whether it’s with a cough assist machine. There are techniques that can be very effective.
Next, positioning. So, what do I mean with positioning? So, during COVID for example, a lot of patients in ICU ended up in prone position for ARDS (Acute respiratory distress syndrome), COVID ARDS, or COVID pneumonia. The effect of that is simply secretion drainage. The lungs have shut down. A lot of secretions have accumulated in the lungs, whether through ARDS or COVID pneumonia. So, by putting someone head down on their abdomen, you’re draining out secretions. You can do the same in this situation, assuming that your loved one doesn’t have any contractions, but head down and prone position or potentially 135-degree position for short periods of times, assuming your loved one is hemodynamically stable.
But again, with Intensive Care at Home, we can manage all of that. Our ICU nurses can monitor hemodynamic status and so forth and make sure it’s safe if we do go down that track of prone position or 135 degrees. We’ve had clients where we’ve done that at home. We put them in semi-prone in 135 degrees, head down, very effective to get secretions mobilized and manage secretions that way.
Next, you can use a vaporizer. So, what happens when there’s a tracheostomy? You’re bypassing the natural air intake or oxygen intake. So, by using a vaporizer in the room where your loved one is in or where you are in really helps with moisturizing airways, helps with fresh air and so forth. So, that’s another way to help managing secretions.
Next, another very important thing when it comes to excessive secretion management, whether it’s for cerebral palsy, MND (motor neuron disease), C1, C2 spinal injury, but also for any other clients that are at home on a ventilator with the tracheostomy or in ICU for that matter, assuming that most patients will have a tracheostomy with an inner cannula, you need to change your inner cannula regularly. You need to inspect it regularly, making sure that there’s no blockage, because if there’s excessive sputum, the risk of a blockage is very high, and the last thing you want is a blockage and a respiratory arrest. So, inner cannulas need to be changed regularly. I argue at least three times a day, sometimes even more often depending on sputum production.
Now, there are some clients that have a tracheostomy without an inner cannula, and then you need to make sure the tracheostomy is getting changed regularly without the inner cannula because there is no inner cannula. So, we would advocate a monthly tracheostomy change if there’s no in inner cannula.
Next, what is important to understand as well is the more you suction, generally speaking, the more sputum will be produced. That’s certainly my experience. You find it in the literature as well that the more you suction, the more sputum is generally speaking produced. So ideally, try to minimize it as much as you can. Try to change the interval, try to slow suctioning down as much as possible and see whether there’s a result on the other end.
Next, humidification. So, when you have someone on a ventilator with a tracheostomy, you need to humidify the air and the oxygen that’s going in, whether it’s through the ventilator or whether it’s through a tracheostomy collar or a tracheostomy mask. Humidification is important. For anyone breathing naturally, when you’re breathing through the nose, air is automatically getting humidified. It’s a natural process. Now, when you have a tracheostomy, the nose is bypassed, and if you would inhale the air through the tracheostomy, it would be very dry, so therefore humidification is very important. You can’t really go without a humidifier.
You might find that when you go out, for example, with a patient or with our clients or when we take them out from their home with Intensive Care at Home, we find that when they go on an HME filter and go off the humidification, sometimes sputum can dry up or can be produced excessively because it’s just very irritable, but humidification is a big one.
Also, sometimes hydration. Now, you might argue, “Why would you hydrate if there’s excessive sputum production?” Well, if there is excessive sputum production, you might also lose some fluid. So, keeping your hydration up or your loved one’s hydration up is very important too, but again, we do all of that with Intensive Care at Home. We check and manage fluid balances so that everything is in check and well balanced.
Next, another way to manage excessive sputum is with cuff deflation. So, when someone is having a tracheostomy, assuming they’re not pediatrics, they have a tracheostomy with a cuff, so to prevent aspiration and also make sure that any ventilation that’s going on that there’s no leak. So therefore, once or twice a day, you might as well deflate the cuff, and I’ll tell you why you might want to deflate the cuff. You might want to do a subglottic. When you deflate the cuff, then you need to suction so that everything that’s accumulated around the cuff is being eliminated as well. Again, that’s the skill of an intensive care nurse or respiratory therapist if you are in the U.S., but all of our intensive care nurses here are able to manage the cough deflation procedure.
And then also, some tracheostomies have a subglottic port. If you’re watching this and you’re wondering what’s a subglottic port, it’s basically a port where you can aspirate secretions from the subglottis as well below the tracheostomy. Again, that is important to get rid of any secretions around the tip of the tracheostomy below the cuff, so that there’s no excessive sputum accumulation there as well. So, there’s definitely some nuances here that you need to be mindful of, how to manage secretions effectively, making sure there’s no blockages, and so forth.
Next, again, I keep coming back to chest physiotherapist from earlier. You could also use some coughing techniques. Again, that’s where a good physiotherapist is coming in or chest physiotherapist that can work with a client and manage their cough. Sometimes when you suction, there is this cough attack or a violent cough, and that is really difficult to manage. Sometimes, you don’t want the violent cough. Again, a good physiotherapist can manage that and help clients with that.
Also, a good physiotherapist can train clients with breathing techniques. Slowing breathing down, slow inspiration, slow expiration, assuming that the client has some form of spontaneous breathing efforts.
Next, early mobilization, of course. Early mobilization should be done for any patient really in ICU or even at home with Intensive Care at Home, we mobilize our clients almost every day, again, to mobilize any secretions that might be lingering around to prevent pneumonia, to prevent chest infections so that the lungs can get fully expanded.
So, I talked about that. I talked about regular inner cannula changes, regular tracheostomy changes. Then also, you got to make sure that it’s a sterile suction technique, but we talked about that when using a closed suction system that it is sterile.
Monitor vital signs. When someone is getting suction regularly, monitor their oxygen saturation, monitor their pulse because oxygen can drop during lengthy suction procedures so you got to make sure that everything is monitored. Sometimes you need to give a little bit of extra oxygen before suctioning.
Also, when there is excessive mucus, obviously you will find that your tracheostomy dressing and your tapes are often wet and you need to change them probably more often, more frequently, which could then in retrospect produce more coughing, and that could create a vicious cycle. So, when you do have to tracheostomy dressings change, the ICU nurses with Intensive Care at Home, we always try to do them very carefully so we are not setting off another coughing fit or another violent cough. So, that’s really important, but you need to know what to do. You need the experience with tracheostomy dressing changes, which we have at Intensive Care at Home.
Also, last but not least, my last tip to manage excessive secretions before I come to your questions, Lisa.
Last but not least, the length of the tube can sometimes be irritating as well. So, what that means is, for example, let’s say a patient has a size 8 tracheostomy and the tip of the tracheostomy sits at the end of the trachea and sits on the tissue, on the tracheal tissue, that can be very irritating and can produce coughing, excessive sputum production. If you think that’s the case, then either you need to use a smaller size, maybe a size seven, or you need to cut the length of the tracheostomy so that there’s no sitting off the tracheal tip on the tissue. So, maybe the size of the tracheostomy is an issue as well.
So, I think if there are any questions about, “How to manage excessive secretions when having a tracheostomy?”, please type them into the chat pad, or if you’re watching the video in the recording, you can type it below the video and then I can make a video about it or in another live stream, or you can just contact us at intensivecareathome.com and we can help you from there.
Hi, Lisa. Nice to see you again. I’ll just have a look at your questions now. “So, my brother is on a ventilator and we’re wondering if it’ll help him if we tell him to breathe and gently shake him when he starts to get tired. My sister did that today and noticed that he started breathing whenever she told him to. We’re meeting the family that had the meeting on Thursday morning that you were part of. Thank you so much. You really made a huge difference.”
Thank you. Lisa, I think that’s a great idea. If you tell your brother what to do and he’s doing that and obviously that helps him moving forward, then you should be doing that, absolutely, 100%. Just be gentle about it. Keep talking to him and remind him. The other thing is obviously you’re saying that gently shake him when he starts to get tired. One issue in ICU is often that patients have difficulties getting back into a normal day and night rhythm.
In the ideal world, your brother will breathe spontaneously during the day, have a rest overnight, go back on full ventilation support overnight, and then the same again the next day, and then ideally increase the length of time he can breathe spontaneously. Maybe on the first day, he can breathe spontaneously from 10:00 to 4:00. Next day maybe he can do 10:00 to 6:00. Next day he can do 8:00 to 6:00 and so forth. And then, lengthen the time that he breathes spontaneously back on a controlled ventilation mode overnight. And then eventually, hopefully, he can be in a spontaneous mode, 24 hours a day, and then take him off the ventilator eventually.
But just as I mentioned before, one important aspect, we didn’t get to talk about it in the family meeting on Thursday, is mobilization. I couldn’t hear whether, (A), your brother was getting mobilized. (B), they didn’t give any indication whether he couldn’t be mobilized. From what I understand, he could be mobilized. You can only really strengthen breathing muscles by mobilizing patients. He needs to start sitting up. Maybe that’ll also help him getting more awake. If you’re not stimulating someone, he may not start waking up. That’s just some thoughts there, Lisa, that I believe he needs to get mobilized.
When we were in the meeting on Thursday, you heard them saying he was stable. It was really just that he wasn’t waking up and that he was at a crossroads whether he needed a tracheostomy or not. I hope that makes sense, Lisa. You’re welcome to continue asking questions.
So, let’s look at other questions that came in this week. So, here’s a question from Christina that came in this week.
“Hi, Patrik. My father just died on the 2nd of February 2023. He was due to have a procedure, a tricuspid valve replacement. About four hours into the surgery, a doctor called and told us that they had lost the valve, didn’t know where it was, and that he wouldn’t make it off the operating table, and that they needed to do open heart surgery.
My father had open heart surgery about 10 years prior and was 68 years of age. He was in ICU when we saw him. Many hours later, doctor came in the waiting area and told us that he may have had a stroke and that the valve had started turning into the artery. They left his chest opened and only closed the skin. He basically told us that he didn’t think he was going to make it through the night and that they were worried about his kidneys.
About 2:00 AM, a doctor called and said that my father’s blood pressure was rising and that he wasn’t doing well. The next morning when we got to the hospital, they told us that they had stopped sedation, that he was responding. He would maybe slightly open one eye, but he was swelling and filling up with fluid, and he has stopped urinating. We hated seeing him like that, and the doctors were saying he wasn’t going to make it, and we had them take him off life support.
We need help, help understanding what happened, help getting closer to the truth, help figuring out if we did the right thing, help figuring out how it was just a rare circumstance or if a doctor had done something wrong.
Please help.”
Oh, Christina, I’m very sorry to hear that. So, what I do understand is that unfortunately, he passed away if we have to take it. You’re not saying it in those words, but you are insinuating that your dad has passed away, but it’s not 100% clear from the email for me whether he has or he hasn’t passed away. Anyway, let’s just break this down.
“He was due to have a procedure, a tricuspid valve replacement. Four hours into the surgery, doctor called us and told us they had lost the valve.” Christina, in over 25 years of doing this, I have never heard of someone losing a valve during a valve replacement or repair surgery. I’ve never heard of this. Now, I would argue if they’ve lost the valve, his heart would’ve stopped beating if they didn’t have a quick fix, maybe put him on ECMO (Extracorporeal membrane oxygenation). I mean, replacing a valve requires to put someone on a bypass machine or on an ECMO machine to have the ECMO machine or the bypass machine doing the work of the heart while they’re operating on it.
If they’ve lost the valve, I argue his heart stopped operating and he would’ve died. So, I’m just assuming from what I’m reading here that they put him on ECMO or on a bypass machine to replace the function of the heart. So, then you’re saying he had to have open heart surgery. So, what I’m assuming is that if the valve repair minimally invasive, which they can do this in this day and age, but again, I have never heard of a valve going missing.
So then, “They did open heart surgery and then you were told he may have had a stroke and that the valve had start turning into the artery. They left the chest open and only closed the skin. And then they were worried about his kidneys. Blood pressure was rising, that he wasn’t doing well. The next morning when we got to hospital, they told us that they had stopped sedation and that he was responding. He move maybe slightly open one eye, but he was swelling and fitting up with fluids and he stopped urinating. We hated seeing him like that, and the doctors were saying he wasn’t going to make it, and we had to take him off life support.” Well, it’s hard to say for me whether they had to take him off life support or not. I presume he would’ve been on ECMO. Patients can be on ECMO for a few weeks until the issues with the heart can be replaced or resumed. Maybe you needed a heart transplant, maybe you needed another valve. I don’t know. There’s not information in there for me to say what’s really happened.
Have you made the right decision by taking him off life support? I don’t know. I would need to know, we would need to look at the medical records and find out what’s exactly happened. “Was taking him off life support the only option?” It often isn’t the only option, irregardless of what they’re telling you.
So, I have made videos about topics such as, “The difference between real or perceived end-of-life situations in intensive care.” What do I mean by that? So, a real end-of-life situation in ICU is that no matter what you do in intensive care, treatment, surgery, medication, whatever it is, you cannot save a life. The situation is so grave that organs are failing and no treatment, no surgery, no nothing will save a life. That’s a real end-of-life situation. A perceived end-of-life situation is when the doctors might tell you, “Well, your loved one is going to die for sure.” And then maybe we come in and give a second opinion and say, “Well, what about this treatment? What about that treatment?” And then treatment is started and then a life might be saved. So, you can see a difference there.
What I don’t know about your situation, Christina, is, was it a real or a perceived end-of-life situation? I.e., was there something they could have done to save his life? If someone is on life support and you take off life support, chances that someone is dying are real, assuming they’re not ready to come off life support. But the question here is could they have done another surgery, replace or repair the valve? Could they have kept him on ECMO and wait for the heart to recover? Could he have gone on a heart transplant? Could he have gone on LVAD (Left Ventricular Assist Device), RVAD (Right Ventricular Assist Device), wait for a heart transplant? I don’t know. We would need to look at the medical records, Christina, and I’m very sorry to hear what’s happened here.
Another question we had from Yolanda this week is, “My mom had a massive heart attack surgery. They put my mom in ICU and turned her upside down, i.e., a prone position, and she got a blood clot in her brain. Can that kill her?” Let’s put this in perspective. Anyone can die at any given time. That’s just human nature. When someone is in intensive care, they’re probably as close to death as they’ve ever been. That’s why people are in intensive care to have all the equipment, treatment, especially skill to save lives. Now, chances are that your mother in a situation like that is probably as close to death as she has ever been. So, let’s break down some stats here.
When you look at the stats, approximately 90% of intensive care patients survive intensive care. So, that’s one out of 10 not surviving intensive care, but it’s 9 out of 10 surviving intensive care. So, my question to you Yolanda will be, why should your mother be one out of 10 as opposed to nine out of 10 in surviving this?
Now, by reading your short email, you are giving me 5% of the information that I would need in order to guide you with this. Again, I read it out again. You’re saying, “After my mom is in ICU after a massive heart attack, she had surgery. They put my mother in ICU in the prone position upside down, and she got the blood clot in her brain. Can that kill her?” Again, when someone is in intensive care, there are dozens of things happening simultaneously, and we would need to look at the medical record or talk to doctors and nurses directly in order to really answer that question. It’s not enough information. We need to look at what exactly happened. What was the open-heart surgery for? Where did the blood clot come from? What medications is she on? What do chest X-ray, CT scan results look like and so forth? What do blood results look like? What medications is she on? The list goes on.
So unfortunately, it’s not enough information, unfortunately, for me to guide you with this. What I can guide you with is what’s the information that we need. Again, the information we need in a situation like that is full diagnosis, full prognosis, get access to medical records, CT scan result, X-ray results, doctors’ notes, medications she’s on, ventilator settings, vital signs, pathology results and so forth. So, the list goes on.
Let’s move on to the next question from Jolene. Jolene wrote in this week, “My boyfriend had a cardiac arrest, and it was caused from the hospital. Of course, they want everybody to shut him down because they don’t want us to find out. I, on the other hand, have been investigating what led to my boyfriend’s cardiac arrest. It’s only been a week. They’re telling me and his family to withdraw life support and his family wants that. I just feel like I know he’s going to come back if we continue treating him. I feel like I keep telling them ICU always, because I believe they want to kill him because they want to get patients in and out. I am making myself crazy trying to reason with them, and they think I am crazy. They say all of my research I am doing is anecdotal. I don’t know if you respond to your comments, but please help me.” Yes, I do respond to comments. So, this is a comment from one of the YouTube videos this week.
Well, you are absolutely right that in some situations in intensive care, when treatment is withdrawn or suggested to withdraw treatment to families, it’s often to manage beds because you could potentially continue to treat patients. It comes back to what I said a minute ago, the difference between real and perceived end-of-life situations. Is your boyfriend in a real or in a perceived end-of-life situation? I argue with what you’ve shared with me he might be in a perceived end-of-life situation. So, rather than withdrawing life support, life support needs to continue to see whether he can recover.
Now, one of the challenges that you might be facing is as the girlfriend, you may not have any decision-making authority unless you are the power of attorney for your boyfriend. I don’t know. You haven’t shared anything there whether that is or isn’t the case. But at the end of the day, life is a negotiation on all levels, and you should continue advocating for your boyfriend. Best way to keep advocating for him is to contact us. We can talk to the doctors directly. We can find out very quickly what’s really going on by talking to them, by asking them a series of questions or by looking at medical records or ideally do a combination of both.
Let’s move on to the next question from Jonathan, “Please give me some input as to whether or not I am providing the realistic care and have the proper thinking process for my loving and dear 22-year-old cerebral palsy daughter.” This is actually another email from the reader that we had earlier where I answered the question about excessive sputum production.
“Em got pneumonia in 2016, and for one year she was fighting infections going in and out of hospitals. We were advised that she needed a tracheostomy. It was placed on and off a ventilator. Presently, she is in a nursing home. Although they did try to wean her, the respiratory staff was very concerned that her cerebral palsy prevented her from being successful. I was seeking to have her reevaluated by an outside doctor, but COVID has stopped the process. Em, who is alert, eating pureed food because they feel she will aspirate. Em keeps asking to have tracheostomy and ventilator removed, which I don’t think is realistic. However, the hospital has no plan for her care except maintenance. My concern is that she has excessive mucus and all they appear to do is the suctioning on an ongoing basis. Can something else be done for this problem? What is the danger in trying to have weaning try again?”
So, here is the answer to that. Well, it’s probably recently unlikely to have your daughter wean off the ventilator with her condition, but if she’s still in hospital, I talked about how to manage the secretions earlier and I think what she really needs is to go home with Intensive Care at Home. Otherwise, she just keeps ending up getting infections over and over again while she’s in ICU. So, the short answer to your problem really is for her to go home with Intensive Care at Home, and you should contact us with that. You should contact us for Intensive Care at Home because I think that’s a solution going forward. She should no longer be in ICU.
It’s unlikely she can be weaned off the ventilator with cerebral palsy. We can manage the secretions like I explained earlier in the video, and then she’ll be so much safer at home. She’ll have her own team. She’ll have her own 24-hour ICU nursing team at home and that is such a better option. You don’t need to worry about what’s happening in the hospital. You have control of what’s happening at home. So, I hope answering that question.
Let’s move on to the next question from Sylvia. Sylvia writes,
“On December the 5th, my 86-year-old father had surgery to remove his kidneys due to surgery. The surgery went well. The cancer was localized, and the doctors told us that he was 100% cancer-free. However, a few days later, he suffered a complication pneumonia. He was intubated and taken to ICU. He was intubated for almost a month. During this time, he developed ARDS.” The synonym for ARDS (Acute respiratory distress syndrome) is also lung failure.
Eventually, they tried to wean him off the respirator, but were unsuccessful. They performed a tracheostomy, transferred him to the critical care unit from ICU. He has been there for almost a month and a half. They tried to wean him off the ventilator and a couple of times without any success. During the time in ICU, he has developed three different infections. He’s currently fighting the third infection and he’s on antibiotics.
They are pressuring us to transfer him to an LTAC (long-term acute care), but we are refusing to have him transferred because we feel that he will not receive the best care there. This has been a very difficult time for our family. My sister and I have practically been living at the ICU for over two months now since our father cannot be left alone because of all the mistakes the nurses and doctors have made. We ask ourselves if our father will ever be able to come off the ventilator and we are making the right decisions to keeping him on life support.
One day, the doctors are telling us that he’s very strong despite his age and has a good chance of coming off the ventilator. And literally the next day, they’re telling us that they believe that his lung muscles are too weak to ever come off the ventilator. We don’t know who or what to believe anymore and what to do.
My question is does my father have a chance of ever coming off the ventilator? If so, what should they be doing to try to wean him off the ventilator? Are there certain exercises therapy that the RTs (Respiratory Therapist) should be performing to help him, such as inspiratory therapy?
His oxygen level is currently at 50% because he’s fighting off an infection, but it was a 25% not too long ago. We are hoping he can get back to that number. His oxygen saturation level is 100%.
Thank you.
From Sylvia.”
First thing that stands out here, Sylvia, is they probably should have done the tracheostomy earlier and not wait for four weeks because he was probably in an induced coma for four weeks. The longer someone is in an induced coma, the harder it’ll be to wean them off the ventilator.
Now, with ARDS, chances are they may not have been able to do a tracheostomy because he was too unwell. His respiratory support was too high. I don’t know. That’s just me talking from experience.
Anyway, what they should be doing as a next step is really start mobilizing him. Start aggressive physical therapy. You cannot wean someone of a ventilator who’s been in a coma for four weeks without starting to mobilize them. Breathing muscles are weak after four weeks in a coma. Deconditioning is happening. Muscle wastage is happening.
So, the next step is to start mobilizing someone and start mobilizing your dad. When someone is sitting up in a chair, for example, their breathing muscles start to strengthen because someone is sitting up. Imagine you’re lying down in bed, breathing muscles can’t strengthen. So that is the first thing. The next thing you should be looking for is do not let him go to LTAC under any circumstances. LTAC, he’ll just go from a bad situation to a worse situation.
So other questions are, and it’s always good to work with facts. It’s always good to work with facts. What are his ventilator settings? How much oxygen is he on? You mentioned that he’s on 50% of oxygen, sometimes he’s 30% of oxygen. That’s one way. So, the question is what ventilator settings is he on? Is he breathing spontaneously? Is he not breathing spontaneously? So, a lot of it comes down to what ventilator settings is he on? Is he still on sedation? What’s the medications he’s on? What’s his chest X-ray like? Is he still sedated and so forth? So, it’s really important to break it down to the nitty-gritty.
That’s why I keep saying over and over again, the biggest challenge for families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care. I think that’s exactly what you’re talking about.
Also, I guess you are saying that the doctors tell you one day, he can be weaned off the ventilator and the next day they tell you he can’t. Bottom line is probably nobody really knows unless you keep trying. So, that would be my answer to this.
But most importantly, do not give consent to let him go to an LTAC. Do not let him wither away. Get him out of bed as quickly as possible. They need to stop making excuses. I mean, mobilizing someone is very time-consuming, very labor-intensive, but it needs to happen. It needs to happen. You cannot wean someone off a ventilator without mobilization. I just haven’t seen it really.
But one way we can help you is if you contact us directly at intensivecarehotline.com, we can help you to break things down. We can look at the medical records. We can talk to doctors and nurses directly. We can talk to the respiratory therapists. There’s a number of things we can do there, Sylvia. I hope that helps.
Hi, Tom. Nice to see you. I’ll just read out your message. “Hi, Patrik. After a transfer of my ventilator-dependent son from bed to chair via Hoyer and then returned from chair to bed, he suctioned as normal, and the suction returned significant blood. It was so much more than we have seen in more than a year caring for him at home. Local ICU determined that he had aspiration pneumonia. In your opinion, was the bleeding source unknown the cause of the pneumonia or was the bleeding a result of the pneumonia itself?” No, you need more facts definite. Well, I’m sorry to hear that. Do you know whether the bleeding was before they diagnosed him with an aspiration pneumonia or after? From what I’m reading here is it sounds like to me the bleed happened before the aspiration pneumonia.
The first question that I have, Tom, is he on blood thinners? Is he on heparin, Clexane, Lovenox, Fragmin, warfarin? Is he on a blood thinner? That would be my first question. “Before he was, so no longer so they stopped the blood thinner.” That could be one cause. I mean, your son is immobile, i.e., he would need a blood thinner or at least some TED stockings to prevent deep vein thrombosis. So, he’s not on the blood thinner.
So, then the other question is, I said that earlier, Tom, that when there’s excessive secretions, sometimes the tip of the tracheostomy might be a little bit too long and might be sitting on the trachea tissue and it may cause some friction and it may cause a bleed there. So, sometimes you might need to shorten the tracheostomy a little bit. You might need to try a different size. You might just simply need to change the position of the tracheostomy a little bit. That could be one reason.
The other reason could be depending on what you’re using. I talked about a cough assist machine earlier, Tom. Sometimes one of the side effects of a cough assist machine might be to cause some bleeding. Do you know, Tom, if you are using a cough assist machine? Sure. Tom, I was just saying do you use a cough assist machine at home for your son? Do you know what I mean by a cough assist machine? You might know it as a Volara. Anyway, I talked about this earlier, I don’t think you were there, but a cough assist machine basically delivers a high PEEP, positive and negative, and makes patients cough, and eliminates secretions, avoids chest infections, avoids atelectasis and so forth. So, the question is, do you use a cough assist machine? Because if you do, that might cause a bleed as well, especially in combination with a blood thinner. So, I would be curious to find out whether you do or you don’t use the cough assist machine.
In the meantime, while I’m waiting for your answer, Tom, there was a question from Urban Poet who says, “What’s the reason of avoiding LTAC?” One tip here, Urban Poet, is read up on LTAC reviews. Start with reading up LTAC reviews.
Tom, that was my theory. “Tracheostomy tube abrasion during transfer.” Yep, that could be the most likely cause. It could be. You have to look at all other causes as well. But if he’s not on a blood thinner, and no cough assist, thank you for sharing that. If he’s not on a blood thinner and you’re not using a cough assist machine, then I would think an abrasion might be the cause for this. So, I hope that helps, Tom. Look at that and maybe either cut the length of the tracheostomy or change the size. Get a chest X-ray or potentially CT scan even, or potentially a bronchoscopy.
Coming back to our Urban Poet, “What’s the reason of avoiding LTAC?” So, we advise families in intensive care not to go to LTAC after a tracheostomy. LTACs are a better version of a nursing home and you’re sending patients from ICU to a better version of a nursing home. That’s a no-go. That’s an absolute no-go. We literally have families that have loved ones in LTAC begging us to help them to get out of LTAC. It’s often too late when patients are in LTAC.
So, LTAC is being pitched to families in intensive care as specialists for ventilator weaning. Well, nothing could be further from the truth. You’re going from ICU nurses, ICU doctors to RNs without ICU experience. You’re going to having no doctor attendance there. It’s just a big mess. It’s just a big mess at LTAC, Urban Poet, and we argue, stay clear of it. We’ve created a lot of content about what’s happening at LTAC, why people shouldn’t go to LTAC. But in a nutshell, it’s the better version of a nursing home. When you’re sending someone from ICU to LTAC, it’s just madness, absolute madness.
Also, when someone goes to LTAC, the clock is often ticking. Patients get 30 days at LTAC. If they’re not weaned off the ventilator, then they’re going from bad to worse. They’re then going to a skilled nursing facility, which is even worse. You’re setting off a downward spiral and that’s no good.
Also, a lot of patients that go to LTAC from ICU directly, they often end up back in ICU anyway within a few days. And then the issue is that they’re going to a different ICU. So, within a few days, they’ve been to three places, three different teams. That’s madness and insanity. Healthcare needs to be holistic, and it needs to be a team approach. If you’re going from ICU to LTAC, then you’re bouncing back to ICU, but then you’re going back to another ICU because the discharging ICU has no longer had any bed available. It’s madness. I’ll just leave it there.
Well, thank you so much everyone for your questions. I want to wrap this up for today. I hope you find this valuable.
Now, if you have a loved one in intensive care, go to intensivecareathome.com especially if you want to go home. Again, Intensive Care at Home, we are operating all over Australia and all major capital cities, as well as in regional and rural areas. You should contact us if your loved one is in intensive care and you are in Australia and you want home care, especially if you’re talking about ventilation, tracheostomy, non-invasive ventilation, CPAP, BIPAP, tracheostomy care, home TPN, central line care, PICC line care, Hickman’s line care. We can do all of that at home. But even if you’re overseas, if you’re in the U.S. or in the U.K., you should contact us as well, if you need Intensive Care at Home. We can probably point you in the right direction.
If you have questions about care in intensive care, contact us at intensivecarehotline.com. Call us on one of the numbers or send us an email to [email protected] and we can help you from there or call us on one of the numbers on the top of our website.
Also, have a look at our membership for families in intensive care at intensivecaresupport.org. There, you have access to me and my team, 24 hours a day, and we answer all questions intensive care and Intensive Care at Home related.
Also, if you need a medical record review in intensive care or after intensive care, please contact us as well. We do medical record reviews in real time while patients are in intensive care, and we can give you a second opinion or we can review them after intensive care if you have unanswered questions or if you need closure or if you are suspecting medical negligence.
Now, subscribe to my YouTube channel for regular updates for families in intensive care. Share the video with your friends and families. Click the notification bell and comment below what you want to see next and what questions and insights you have from this video.
Thanks for watching.
This is Patrik Hutzel from intensivecareathome.com and from intensivecarehotline.com, and I’ll talk to you in a few days.
Now, if you have a loved one in intensive care and you want to go home with our service intensive care at home and if you want to find out how to get funding for our service and how it all works, please contact us on one of the numbers on the top of our website, or send me an email to [email protected]. That’s Patrik, just with a K at the end.
Please also have a look at our case studies because there we highlight more about what we can do for clients, how clients can live at home with ventilation and tracheostomies and you can look at our case studies as well at our service section.
Intensive care at home Case studies
And if you are at home already and you need support for your critically ill loved one at home, and you have insufficient support or insufficient funding, please contact us as well. We can help you with all of that.
And if you are an intensive care nurse or a pediatric intensive care nurse with a minimum of two years, ICU or pediatric ICU experience, and you ideally have a critical care certificate, please contact us as well. Check out our career section on our website. We are currently hiring ICU and pediatric ICU nurses for clients in the Melbourne metropolitan area, Northern suburbs, Sunbury, Bendigo, Mornington Peninsula, Bittern, Patterson Lakes, Frankston area, South Gippsland, Drouin, Warragul, Trida, Trafalgar and Moe as well as Wollongong in New South Wales.
www.intensivecareathome.com/careers
So we are also an NDIS, TAC (Victoria) and DVA (Department of Veteran affairs) approved community service provider in Australia. Also have a look at our range of full service provisions.
Thank you for watching this video and thank you for tuning into this week’s blog.
This is Patrik from Intensive Care at Home, and I’ll see you again next week in another update.